Cardiovascular Radiology — MCQs

On this page
The investigation of choice in aortic dissection is:
Comment on the diagnosis of the patient?
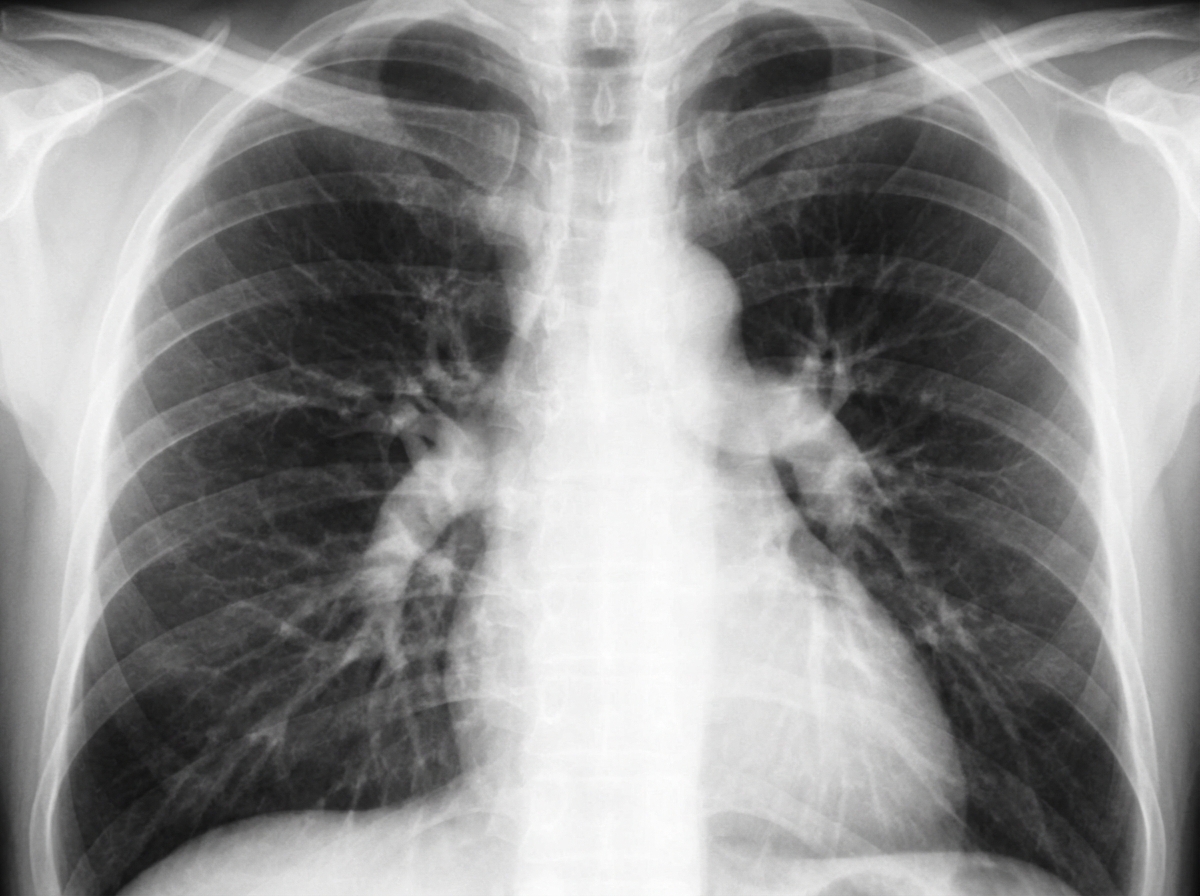
Which of the following conditions places the aorta at the greatest risk of inflammation (aortitis)?
During cardiac imaging, which phase of the cardiac cycle exhibits the minimum motion of the heart?
What is the investigation of choice for aortic dissection?
In which of the following conditions is the left atrium not enlarged?
Which drug is used to perform stress echocardiography?
Which artery is most commonly occluded in an inferior wall myocardial infarction?
Rapid high-frequency fluttering of anterior mitral valve leaflets during systole on 2D echocardiography is characteristically seen with which condition?
Hilar dance on fluoroscopy is seen in which condition?
Practice by Chapter
Cardiovascular Anatomy
Practice Questions
Cardiac CT Techniques
Practice Questions
Cardiac MRI Techniques
Practice Questions
Ischemic Heart Disease Imaging
Practice Questions
Valvular Heart Disease
Practice Questions
Cardiomyopathies
Practice Questions
Pericardial Diseases
Practice Questions
Congenital Heart Disease
Practice Questions
Aortic and Great Vessel Imaging
Practice Questions
Peripheral Vascular Imaging
Practice Questions
Cardiovascular Interventional Procedures
Practice Questions
Post-Surgical Cardiovascular Imaging
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
