Cardiovascular Radiology — MCQs

On this page
Which of the following is the most reliable imaging technique for detecting cyanotic congenital heart diseases in newborns?
A child with Tetralogy of Fallot presents with cyanosis. Which imaging modality is essential for surgical planning?
Which imaging modality is essential for diagnosing Tetralogy of Fallot and planning surgical intervention in infants?
Kerley B lines are seen in mitral stenosis when the resting left atrial pressure exceeds which value?
Which view is taken for aortic window?
Which of the following is a radiological feature of coarctation of the aorta?
Which imaging modality is most effective for assessing plaque morphology in coronary arteries?
Identify the condition in the X-ray given below:
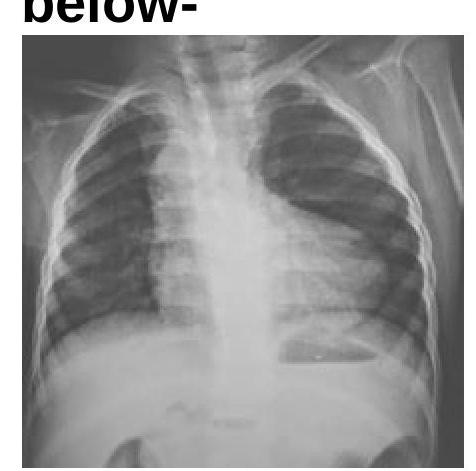
The chest radiograph shown below is from a 25-year-old male patient presenting with hypertension. The image demonstrates bilateral inferior rib notching. What is the most likely diagnosis?
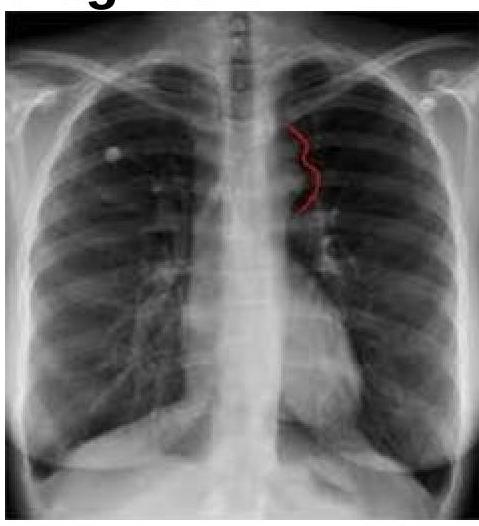
Pulmonary plethora is typically seen in all of the following conditions except:
Practice by Chapter
Cardiovascular Anatomy
Practice Questions
Cardiac CT Techniques
Practice Questions
Cardiac MRI Techniques
Practice Questions
Ischemic Heart Disease Imaging
Practice Questions
Valvular Heart Disease
Practice Questions
Cardiomyopathies
Practice Questions
Pericardial Diseases
Practice Questions
Congenital Heart Disease
Practice Questions
Aortic and Great Vessel Imaging
Practice Questions
Peripheral Vascular Imaging
Practice Questions
Cardiovascular Interventional Procedures
Practice Questions
Post-Surgical Cardiovascular Imaging
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
