Cardiovascular Anatomy — MCQs

Posterior cardinal veins develop into:
All the following openings in the right atrium are guarded by a valve except
Left anterior descending artery is a direct branch of
What is the cardiothoracic ratio in children?
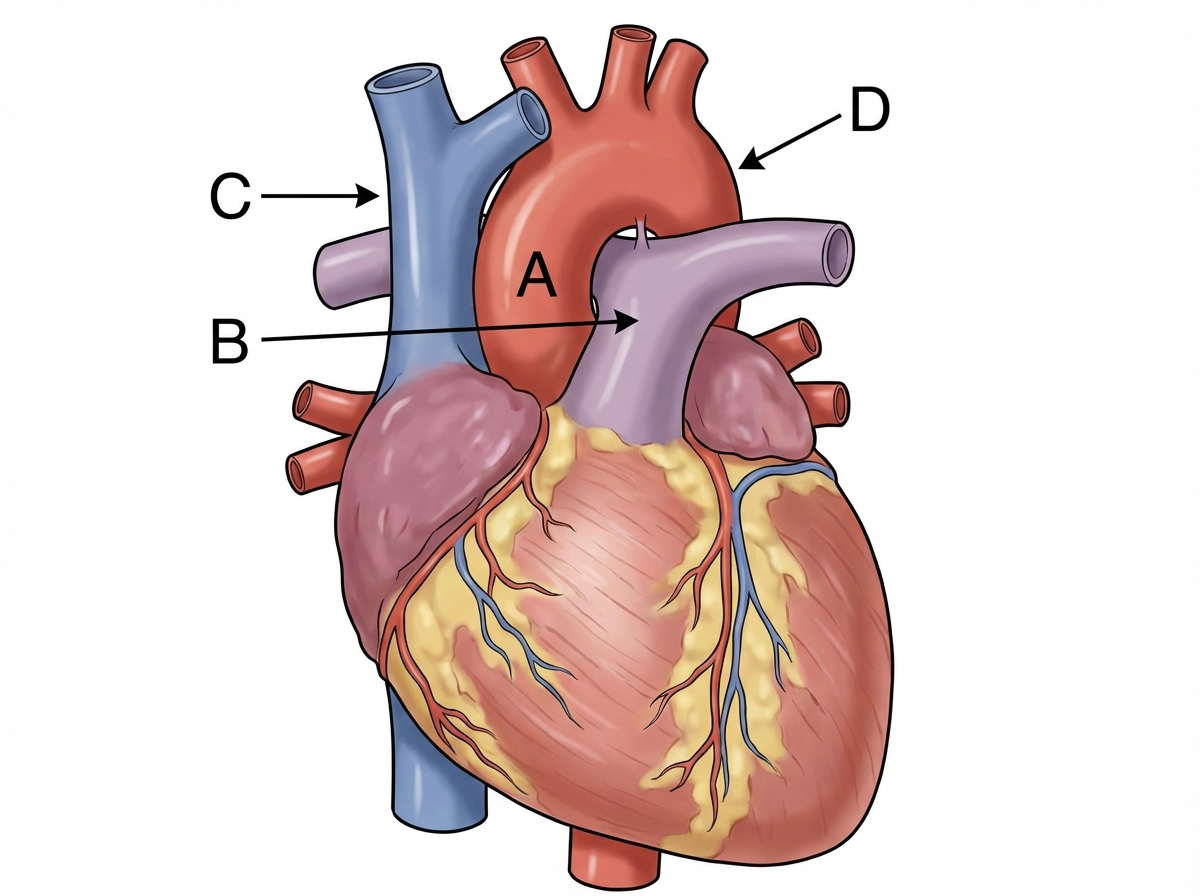
Identify the labeling correctly 
For pericardial calcifications, which is the best investigation?
Which X-ray finding is more characteristic of ASD compared to VSD?
All of the following arteries are common sites of occlusion by a thrombus except:
Which heart chamber has the thickest wall?
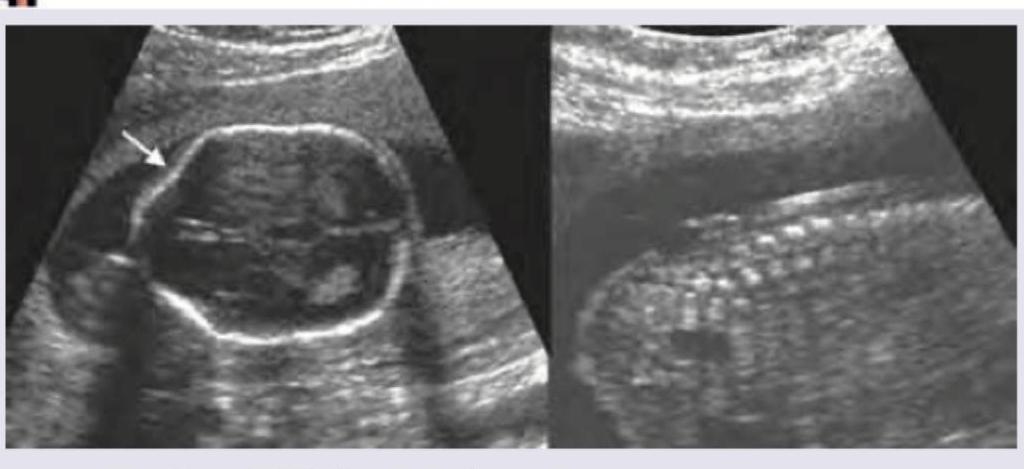
Keyhole sign on fetal ultrasound is seen in:
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
