Cardiovascular Radiology — MCQs

On this page
Which one of the following is used in Cardiovascular imaging?
Which of the following is NOT a characteristic feature of mitral stenosis on X-ray?
Transesophageal echocardiogram (TEE) is preferred to transthoracic echocardiogram (TTE) in which of the following evaluations?
Which of the following statements is true regarding cardiac MRI?
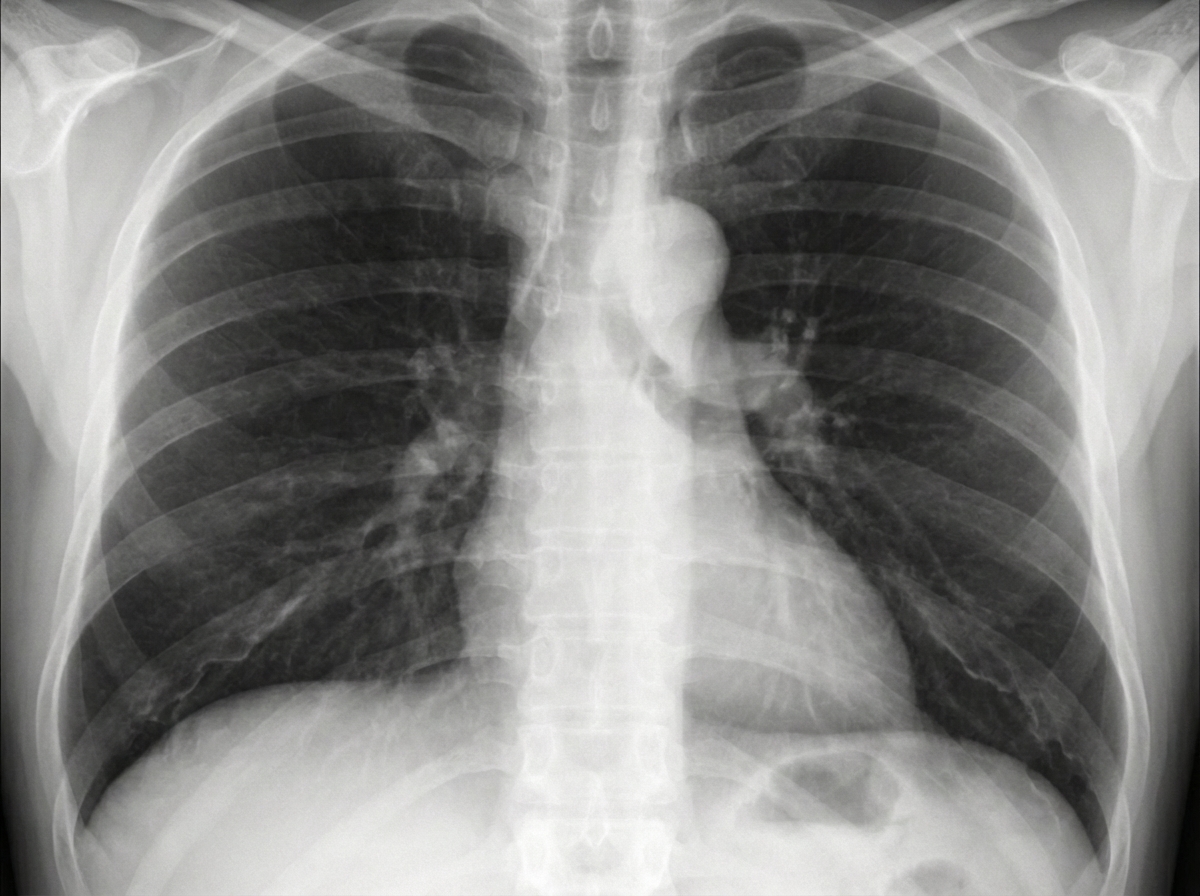
A patient presents with chest pain. What is the diagnosis?
Practice by Chapter
Cardiovascular Anatomy
Practice Questions
Cardiac CT Techniques
Practice Questions
Cardiac MRI Techniques
Practice Questions
Ischemic Heart Disease Imaging
Practice Questions
Valvular Heart Disease
Practice Questions
Cardiomyopathies
Practice Questions
Pericardial Diseases
Practice Questions
Congenital Heart Disease
Practice Questions
Aortic and Great Vessel Imaging
Practice Questions
Peripheral Vascular Imaging
Practice Questions
Cardiovascular Interventional Procedures
Practice Questions
Post-Surgical Cardiovascular Imaging
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
