Breast Imaging — MCQs

On this page
What does the abbreviation DIBIRADS stand for in the context of breast imaging?
What is true about screening mammography?
When is mammography optimally performed in relation to the menstrual cycle?
Which one of the following is the most sensitive and specific screening test to detect breast cancer?
What is the hallmark of breast malignancy on mammography?
What is the typical effective radiation dose used in mammography?
Identify the investigation shown in the image:
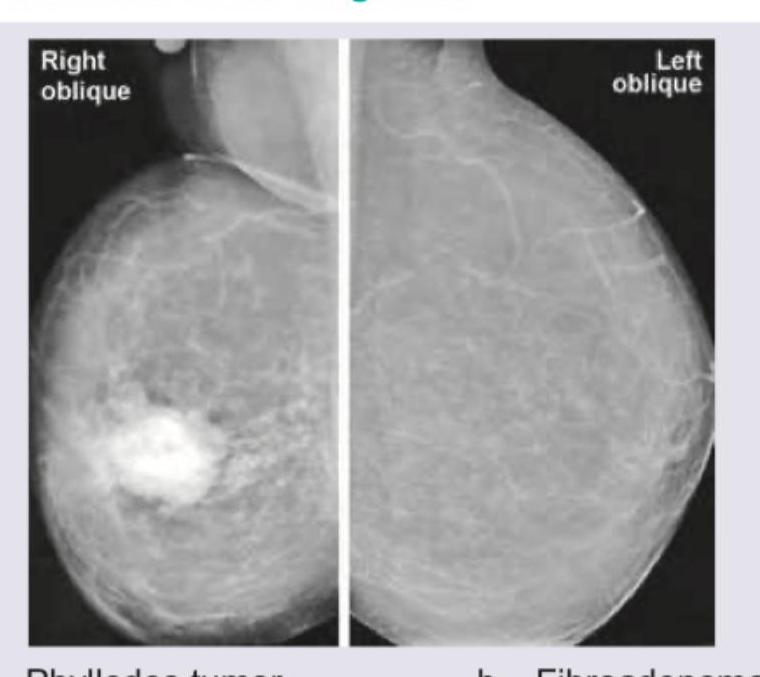
A 35-year-old woman presents with a rapidly enlarging palpable breast mass over the past 3 months. Mammography is performed. What is the most likely diagnosis?
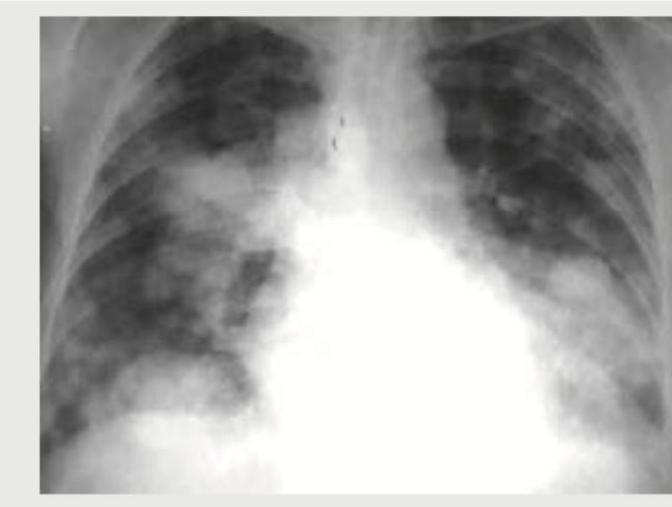
A breast cancer patient presents with difficulty in breathing. CXR shows:
Breast imaging reporting and data system (BI-RADS): Final assessment categorized a 45 year old female to have Category 5 disease. What does the report signify?
Practice by Chapter
Breast Anatomy and Physiology
Practice Questions
Male Breast Imaging
Practice Questions
Mammography Techniques
Practice Questions
BI-RADS Classification
Practice Questions
Breast Ultrasonography
Practice Questions
Breast MRI
Practice Questions
Digital Breast Tomosynthesis
Practice Questions
Benign Breast Diseases
Practice Questions
Breast Cancer Detection and Diagnosis
Practice Questions
Interventional Breast Procedures
Practice Questions
Breast Cancer Screening
Practice Questions
Male Breast Imaging
Practice Questions
Post-treatment Breast Imaging
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
