Breast Imaging — MCQs

On this page
For normal mammography, what is the nominal focal size of the X-ray tube used?
What is the typical radiation dose delivered during mammography?
Which of the following is NOT an indication of malignancy on mammography?
What is the primary purpose of the BIRADS score?
A patient presents with a suspicious breast lump. Ultrasonography reports the lesion as BI-RADS-4. What is your inference?
Which of the following is NOT an indication for MRI in breast carcinoma?
What is a mammographic abnormality seen in breast cancer?
An MLO view of the left breast is shown. What is the MOST likely diagnosis?
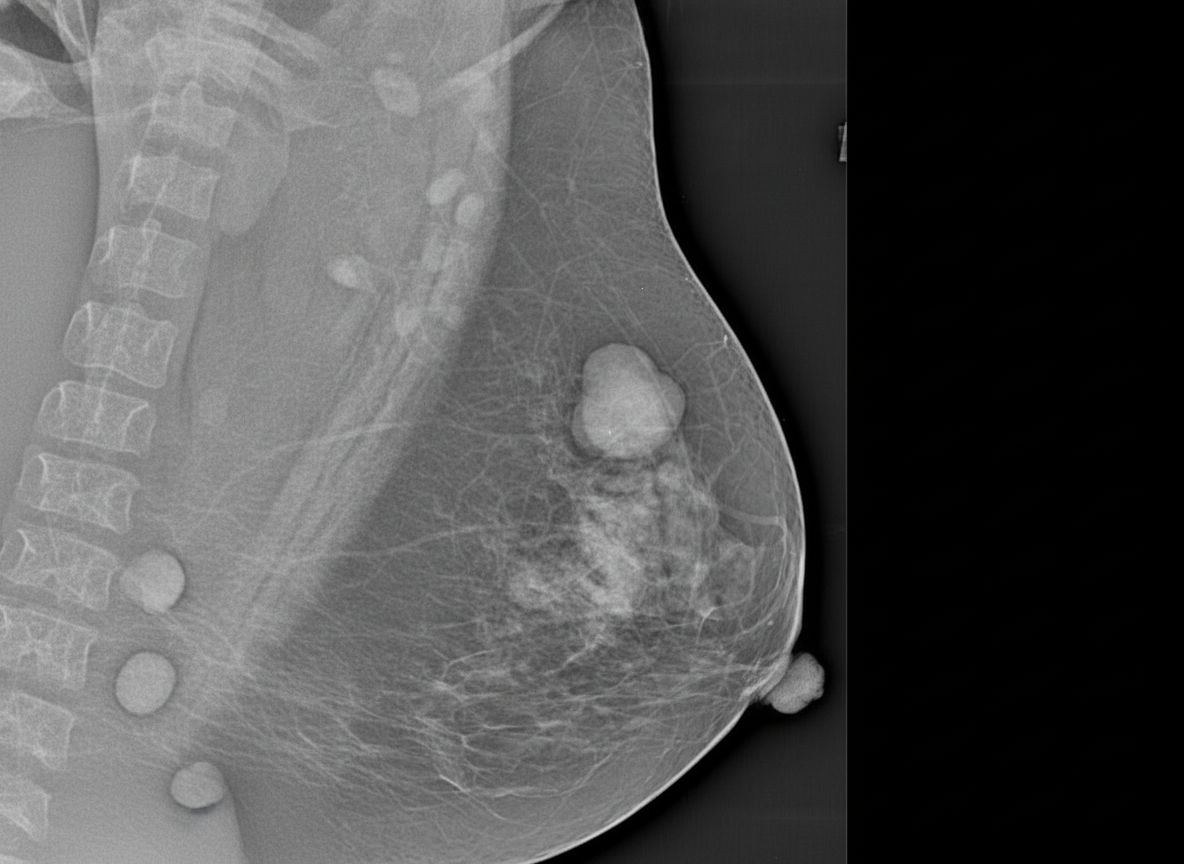
What is the best investigation to differentiate scar tissue from recurrence after mastectomy for breast carcinoma?
Which of the following statements about MRI is NOT true?
Practice by Chapter
Breast Anatomy and Physiology
Practice Questions
Male Breast Imaging
Practice Questions
Mammography Techniques
Practice Questions
BI-RADS Classification
Practice Questions
Breast Ultrasonography
Practice Questions
Breast MRI
Practice Questions
Digital Breast Tomosynthesis
Practice Questions
Benign Breast Diseases
Practice Questions
Breast Cancer Detection and Diagnosis
Practice Questions
Interventional Breast Procedures
Practice Questions
Breast Cancer Screening
Practice Questions
Male Breast Imaging
Practice Questions
Post-treatment Breast Imaging
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
