Imaging of Peritoneal Cavity and Retroperitoneum — MCQs

Identify the imaging modality given below.
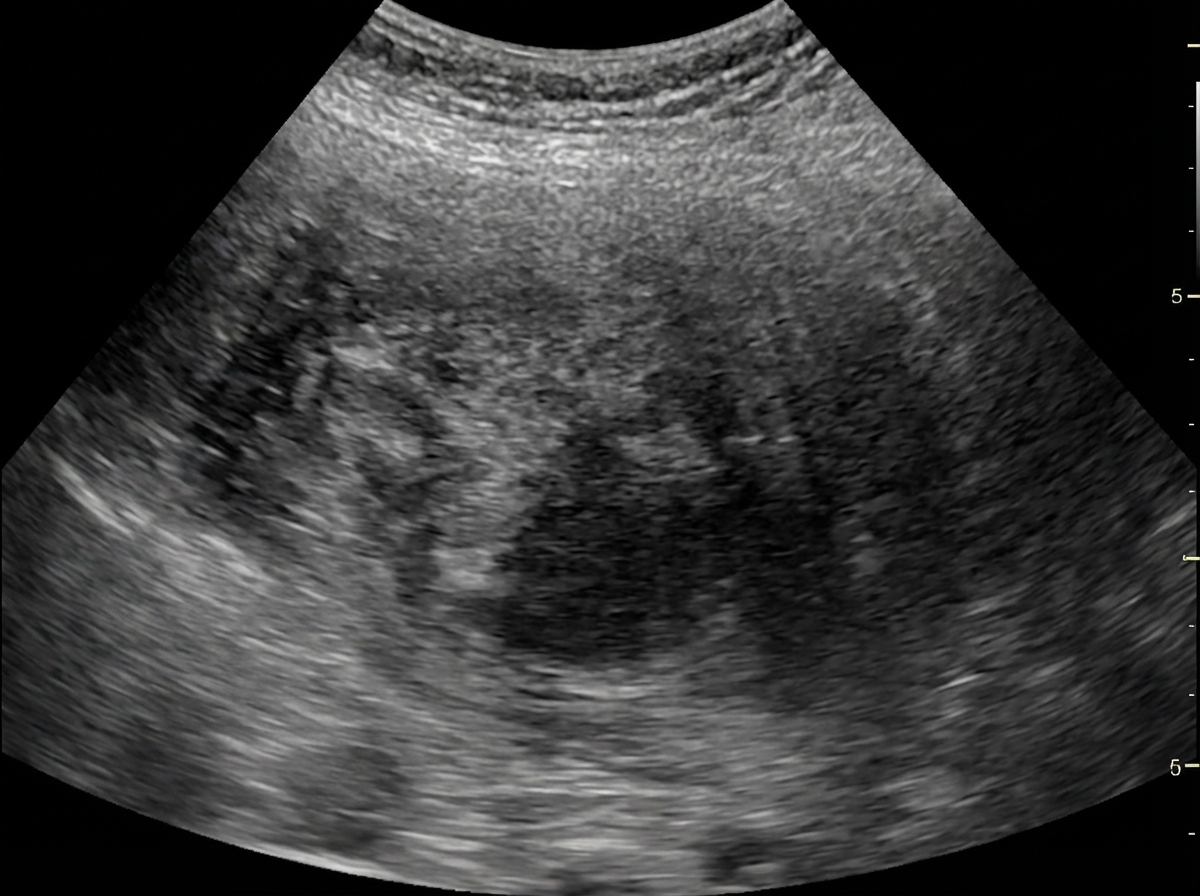
Most sensitive investigation for abdominal trauma in a hemodynamically stable patient is-
Clinical examination of a symptomatic patient shows a Sister Mary Joseph nodule. It is most commonly associated with which of the following?
A child is being assessed for possible intussusception; which of the following would be LEAST likely to provide valuable information?
What are the potential symptoms of malignant transformation in a retroperitoneal lipoma?
Organ which is commonly involved in retroperitoneal fibrosis is
Gas absent from intestine (gasless abdomen) on x-ray is seen in which condition?
What type of uterine anomaly is shown in this X-ray HSG image?
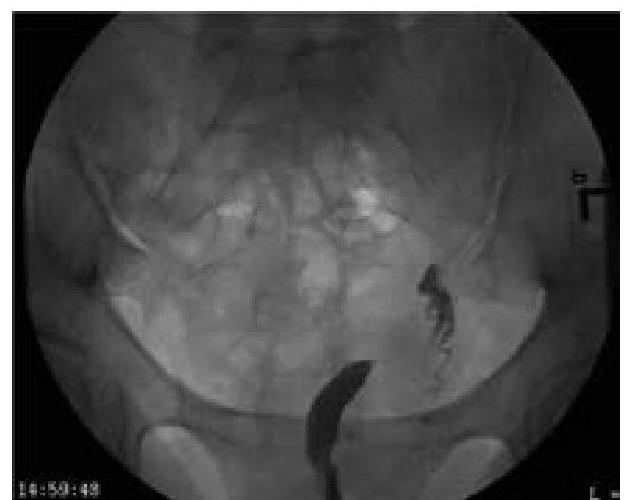
In a patient with a tender and rigid abdomen, what is the expected finding on X-ray?
Blumberg's sign is
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
