Adrenal Imaging — MCQs

A patient presents with headaches, palpitations, hypertension, and urine VMA positivity. The biopsy findings are shown in the image. Which of the following statements is correct?
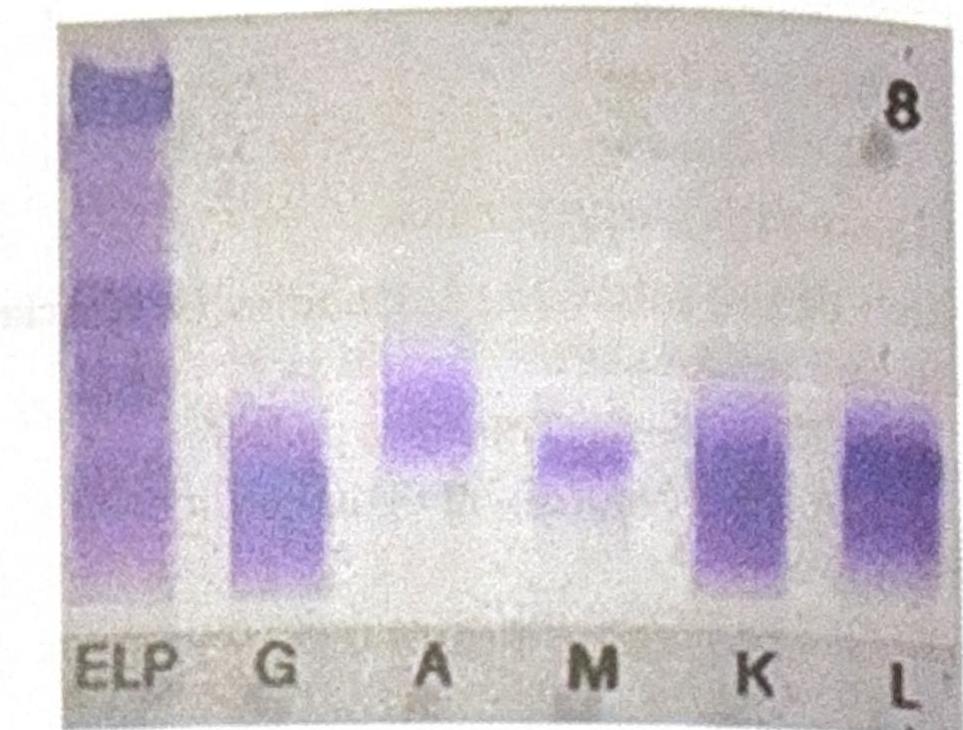
Pheochromocytoma is characterized by excessive secretion of:
What is the Diagnosis based on the CT Scan given below?
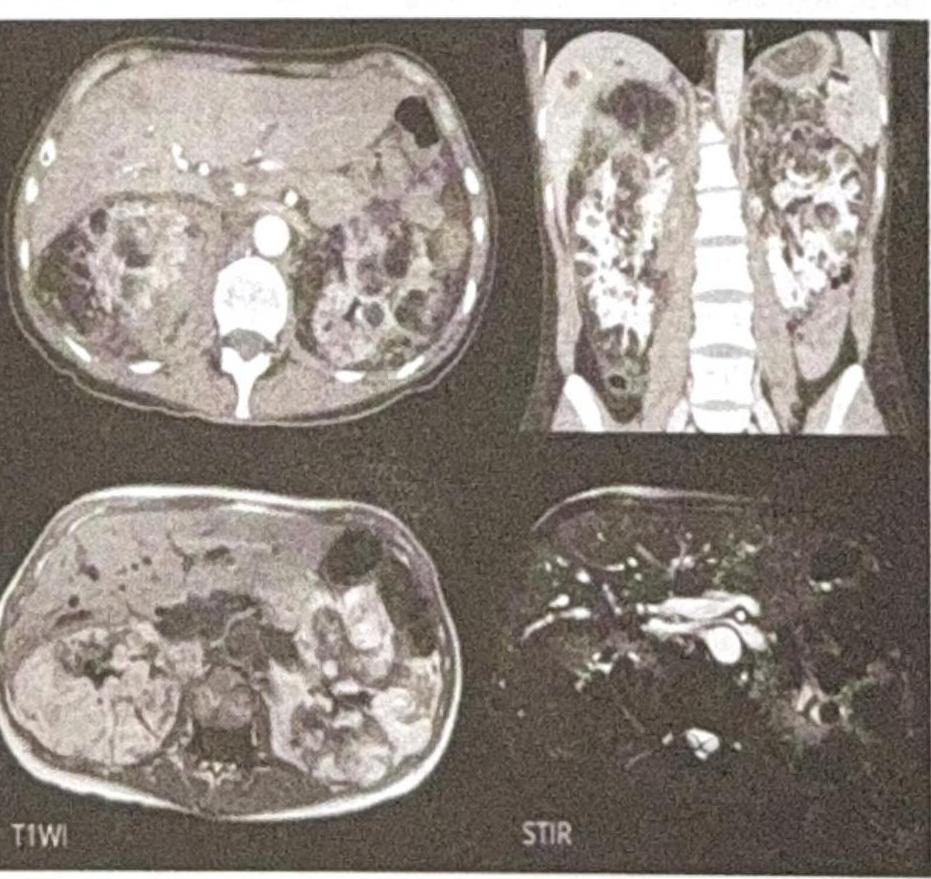
Enhancement in CT contrast is due to -
Which of the following statements about CT imaging is the MOST accurate?
What is the best investigation for diagnosis and staging of renal cell carcinoma with thrombus extending into the IVC?
A pseudo gestational sac is seen on ultrasonography in which of the following conditions?
Which of the following radiographic presentations cannot be seen in a patient with intussusception?
Which of the following conditions typically presents with a 'pseudokidney sign' on ultrasound?
What condition is indicated by the thumb print sign on an abdominal radiograph?
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
