Acute Abdomen Imaging — MCQs

Ultrasound is the best initial investigation of choice for:
What is the investigation of choice for blunt abdominal trauma in an unstable patient?
Most sensitive investigation for abdominal trauma in a hemodynamically stable patient is-
The "Target sign" ultrasonographically means:
In a patient with a tender and rigid abdomen, what is the expected finding on X-ray?
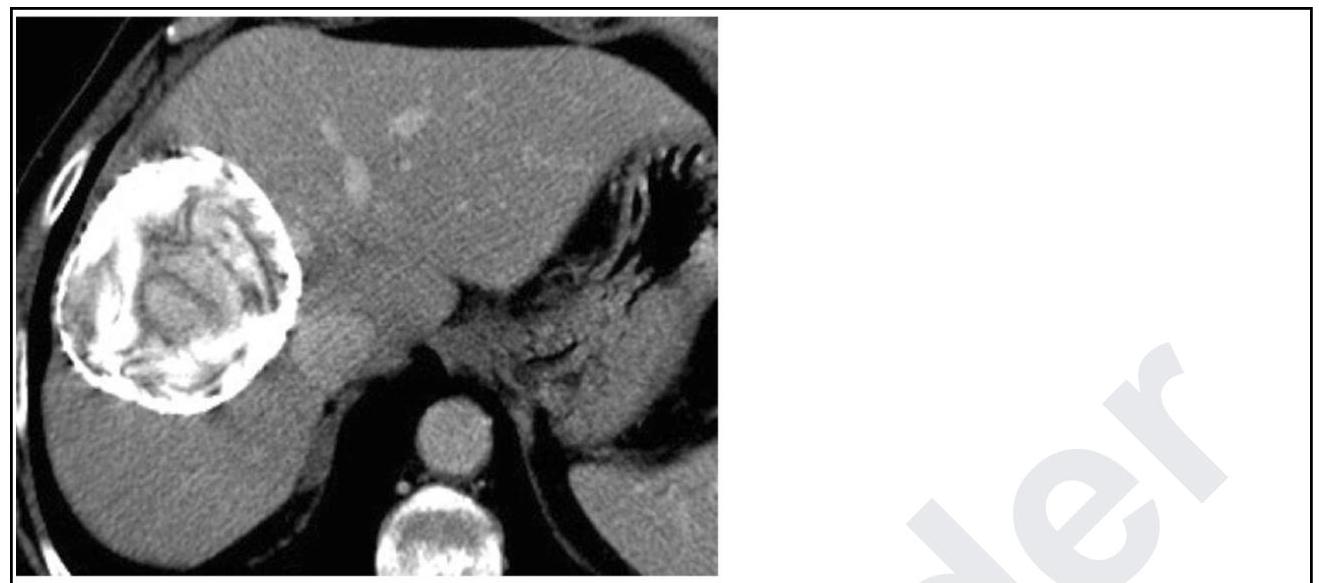
Identify the condition based on the non-contrast CT scan of a patient given below.
Gas absent from intestine (gasless abdomen) on x-ray is seen in which condition?
Gasless abdomen seen in-
What is the investigation of choice for an 8-year-old child presenting with an acute abdomen?
A patient presents to the emergency department with pain and distension of abdomen and absolute constipation. What is the investigation of choice ?
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
