Psychopharmacology — MCQs

On this page
Which of the following statements is true regarding Clozapine?
All of the following are characteristic features of Neuroleptic Malignant Syndrome EXCEPT:
Which of the following drugs are used in the treatment of ADHD?
Depression is not a known side effect of which of the following medications?
Which mood stabilizer is used in the management of drug-induced neutropenia?
Sudden development of a severe throbbing headache is a characteristic side effect of which psychotropic medication?
Which antidepressant drug is known to have both high sedative and anticholinergic activity?
A child with schizophrenia was on medications and suddenly developed neck stiffness and spasm. What is the most probable cause?
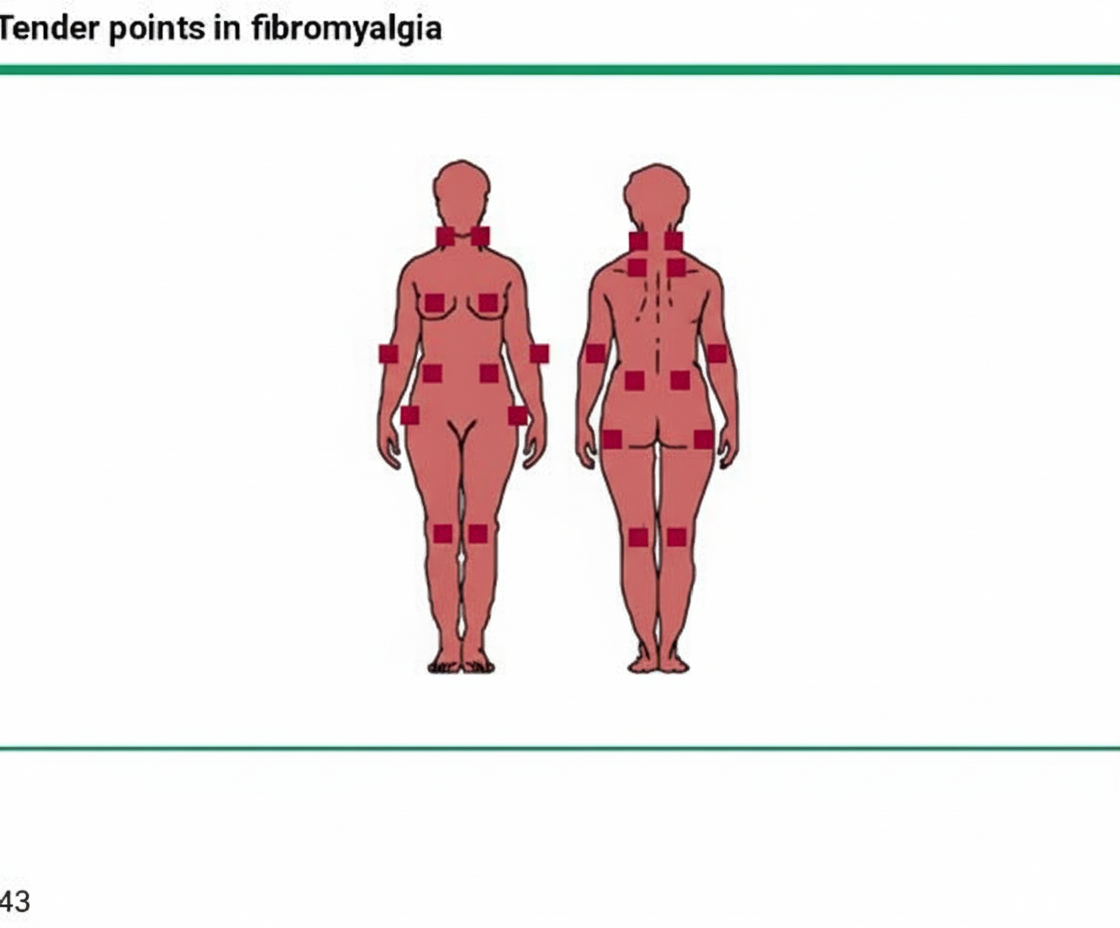
Which serotonin-norepinephrine reuptake inhibitor is predominantly used in the condition shown above?
Which of the following medications is not used in the management of delirium?
Practice by Chapter
Principles of Psychopharmacology
Practice Questions
Antipsychotic Medications
Practice Questions
Antidepressant Medications
Practice Questions
Mood Stabilizers
Practice Questions
Anxiolytics and Hypnotics
Practice Questions
Stimulants and Cognitive Enhancers
Practice Questions
Pharmacokinetics and Pharmacodynamics
Practice Questions
Drug Interactions
Practice Questions
Adverse Effects and Management
Practice Questions
Pharmacogenomics in Psychiatry
Practice Questions
Special Populations Considerations
Practice Questions
Treatment Algorithms and Guidelines
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
