Eating Disorders — MCQs

On this page
Pagophagia involves eating which of the following?
"Russel sign" is:
Anorexia nervosa can be differentiated from bulimia by which of the following?
Which of the following drugs is used for anorexia nervosa?
Which of the following is an eating disorder?
Which of the following psychiatric disorders is characterized by the clinical sign presented?
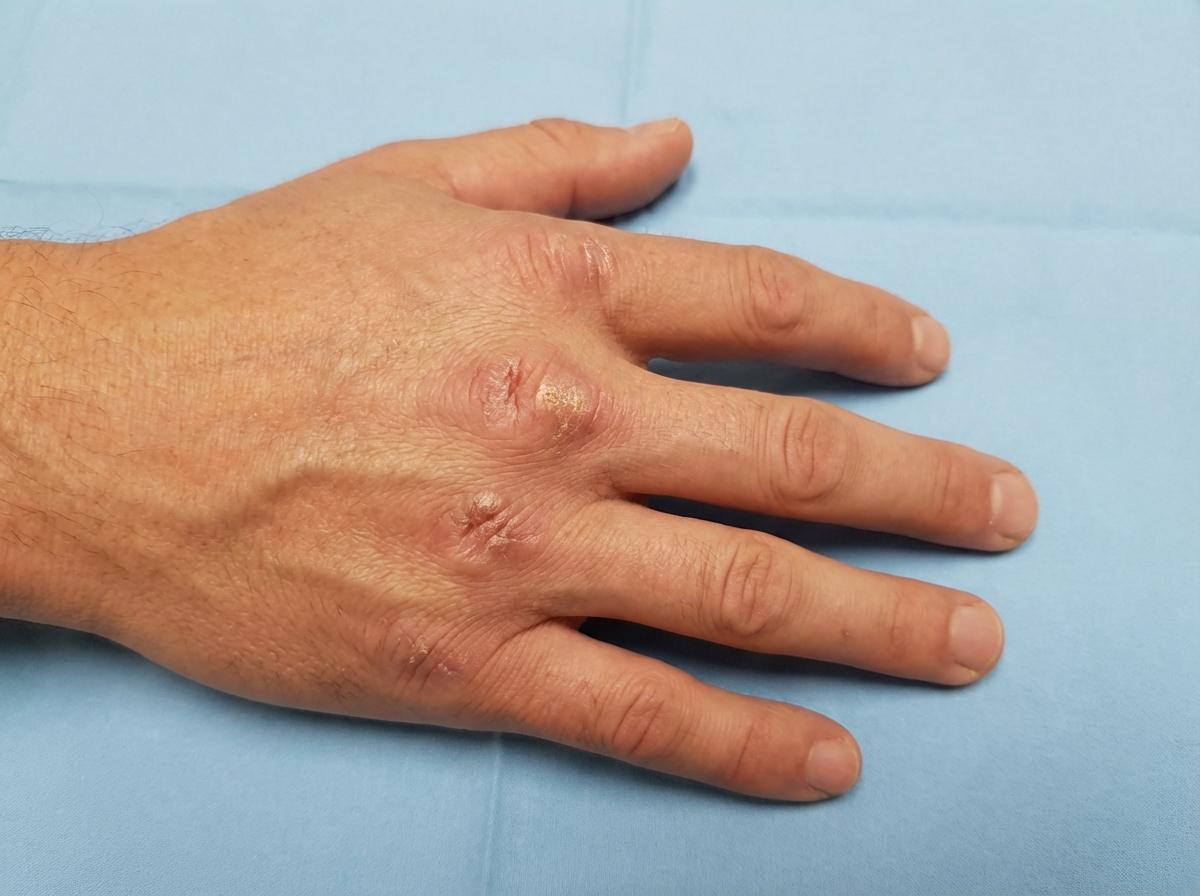
Which of the following is NOT true about trichobezoars?
Type II Anorexia nervosa is characterized by?
Anorexia nervosa is most common in which demographic group?
Which of the following changes is least likely to occur in anorexia nervosa, binge-purging type?
Practice by Chapter
Anorexia Nervosa
Practice Questions
Bulimia Nervosa
Practice Questions
Binge Eating Disorder
Practice Questions
Avoidant/Restrictive Food Intake Disorder
Practice Questions
Pica and Rumination Disorder
Practice Questions
Medical Complications of Eating Disorders
Practice Questions
Inpatient Management
Practice Questions
Outpatient Treatment Approaches
Practice Questions
Family-Based Treatment
Practice Questions
Cognitive-Behavioral Therapy for Eating Disorders
Practice Questions
Pharmacotherapy
Practice Questions
Prevention Strategies
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
