Dermatology
2 questionsA child with a sore throat starts developing skin lesions as in the image below. Which of the following is the diagnosis?
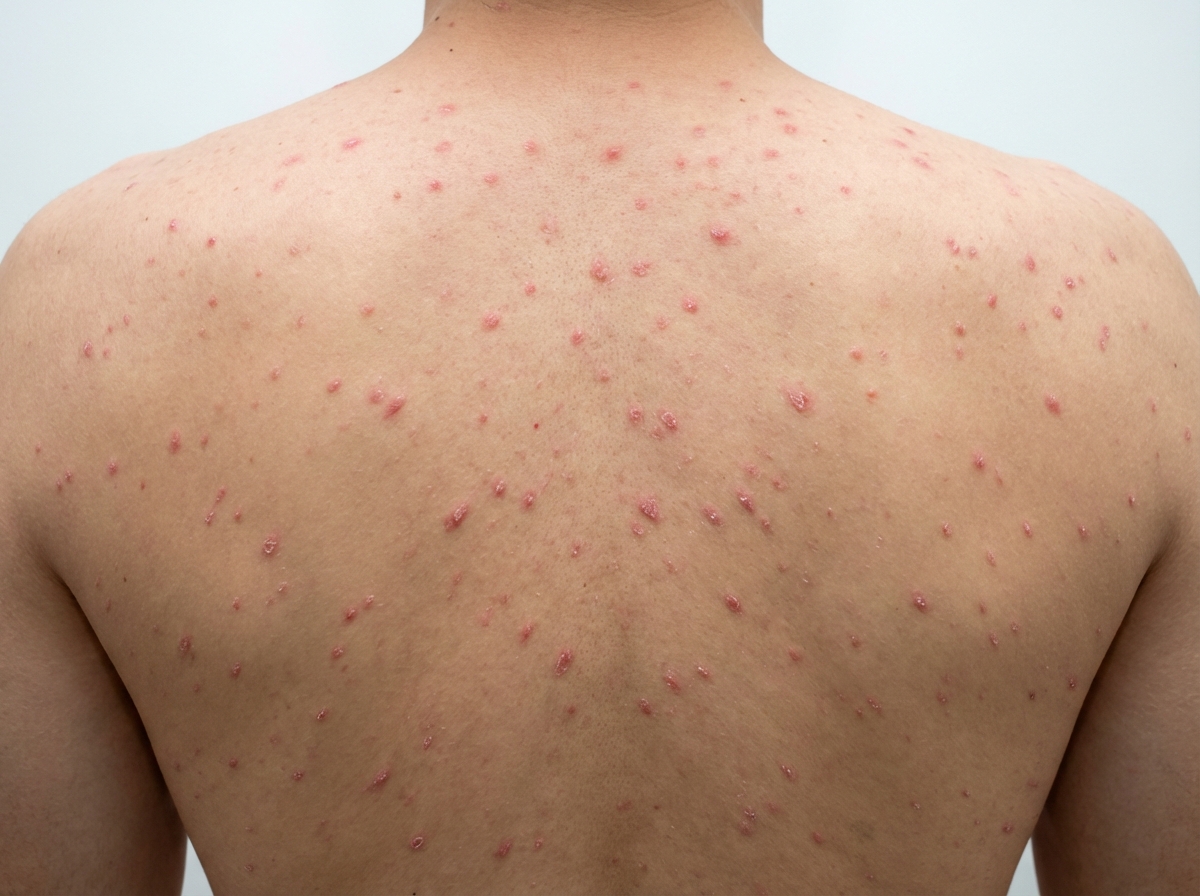
A female patient presents to the OPD with complaints of recurrent lesions on lips, which is associated with fever. Which of the following is the characteristic feature seen in Tzanck smear?
ENT
1 questionsWhich structure is most commonly involved in the compression of the anterior ethmoid nerve, leading to anterior ethmoid nerve syndrome?
Forensic Medicine
2 questionsDuring measurement of a rifled barrel weapon, the caliber depends on?
During the forensic examination of semen from a rape victim, the identification of distinctive yellow needle-like crystals raises attention. What is the specific test employed to confirm the presence of semen?
Obstetrics and Gynecology
2 questionsWhich of the following is the correct definition of postpartum pyrexia?
A 32-year-old woman presents with intermenstrual bleeding following the insertion of an intrauterine device (IUD). She reports no other complications. What is the most appropriate initial management step?
Pediatrics
2 questionsWhat is the most commonly used test for newborn hearing screening?
For how long is exclusive breastfeeding recommended?
Radiology
1 questionsA patient with a history of trauma presents with hearing loss. A High-Resolution Computed Tomography (HRCT) scan was performed. Which of the following structures is not typically visualized on HRCT?