Sensory Systems — MCQs

On this page
The inability to perceive texture and shape of an object occurs in a lesion of which pathway?
Small nerve fibers carry all except:
Pain is appreciated when the small bowel is
All are required for balancing EXCEPT:
Which of the following statements regarding color vision is true?
Proprioception sensation is carried by which of the following pathways?
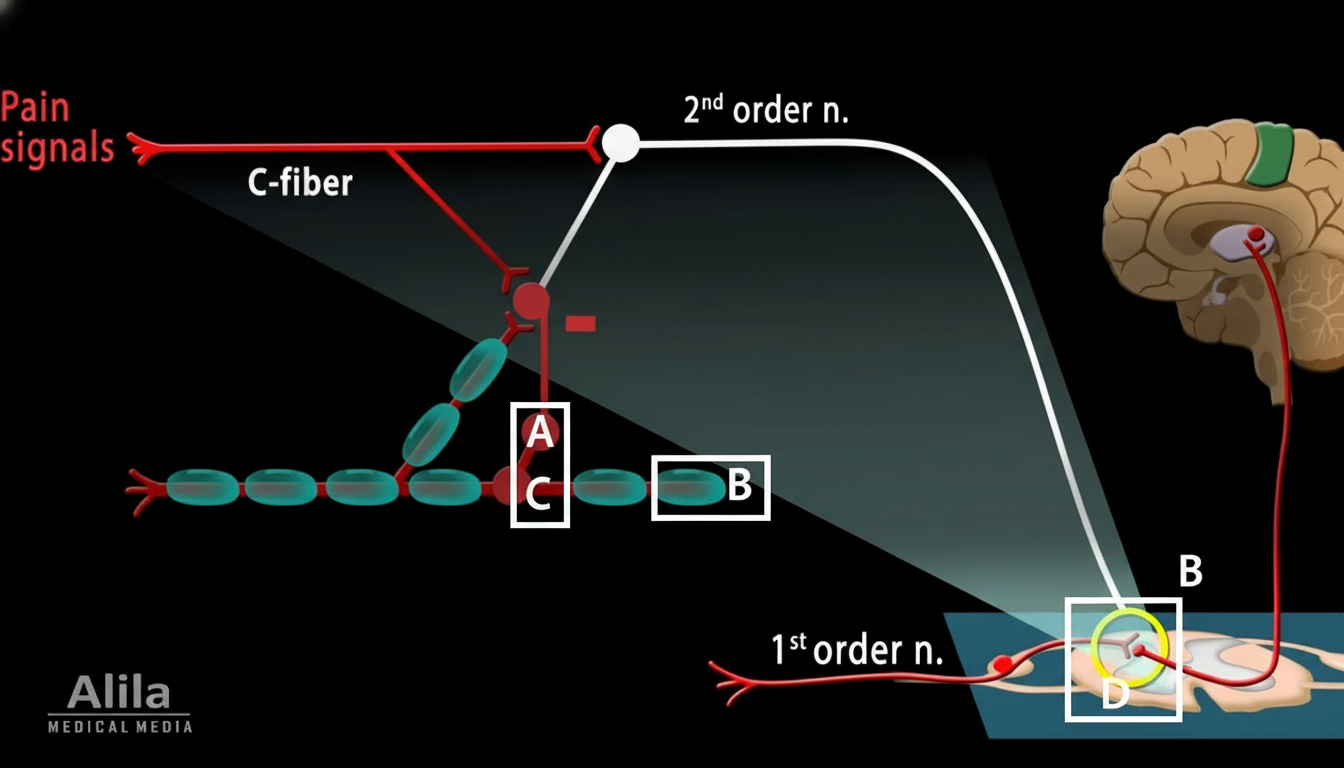
Which of the marked areas is involved in relieving pain when the painful site is massaged?
The decibel level above which auditory fatigue occurs is:
Color vision is mediated by which retinal cells?
Which cell type(s) exhibit action potentials in the human retina?
Practice by Chapter
General Sensory Physiology
Practice Questions
Somatosensation
Practice Questions
Pain Physiology
Practice Questions
Vision and Optics
Practice Questions
Retinal Physiology
Practice Questions
Visual Pathways and Processing
Practice Questions
Auditory System
Practice Questions
Vestibular System
Practice Questions
Taste and Smell
Practice Questions
Sensory Integration
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
