Respiratory System — MCQs

On this page
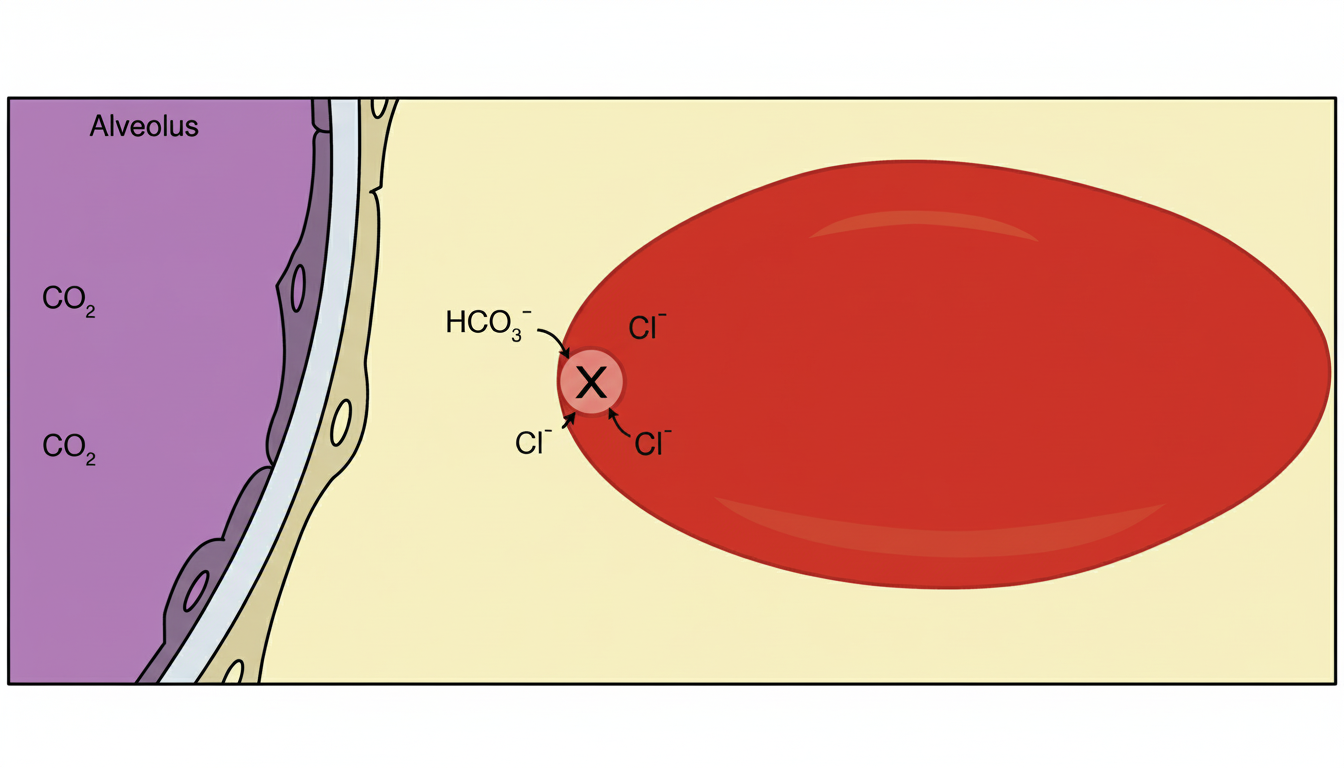
Which protein is responsible for the effect shown in RBC marked as $X$ ?
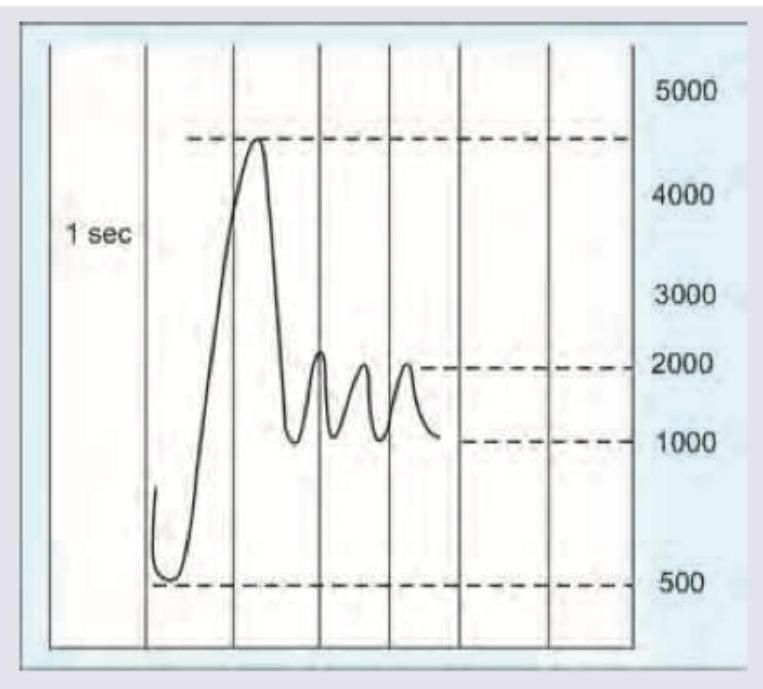
Calculate the FEV1/FVC ratio from the spirometry reading shown below.
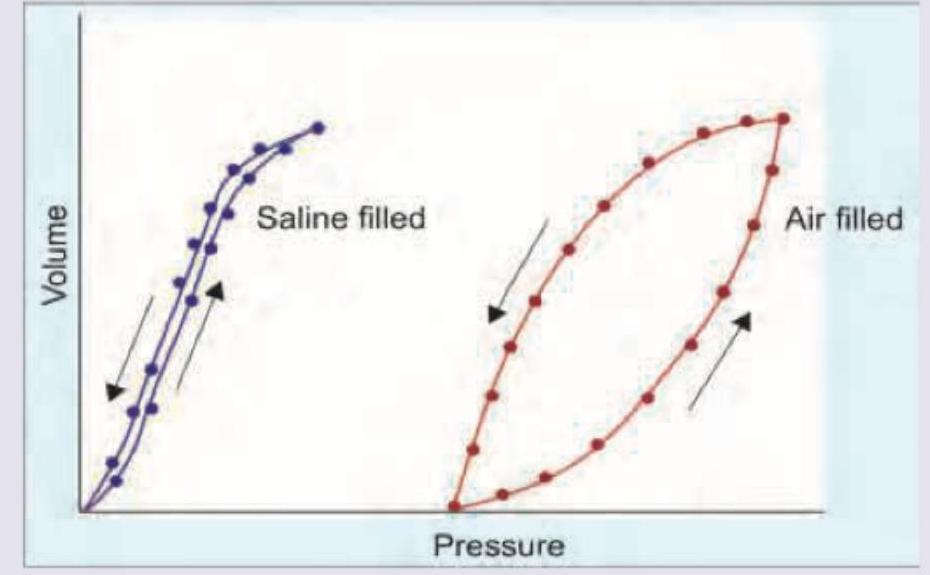
Hysteresis is observed between the deflation and inflation curves in an isolated lung compliance diagram. What is the best description for the same?
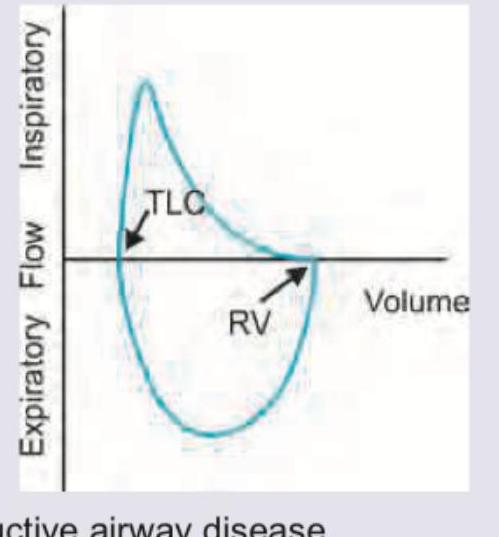
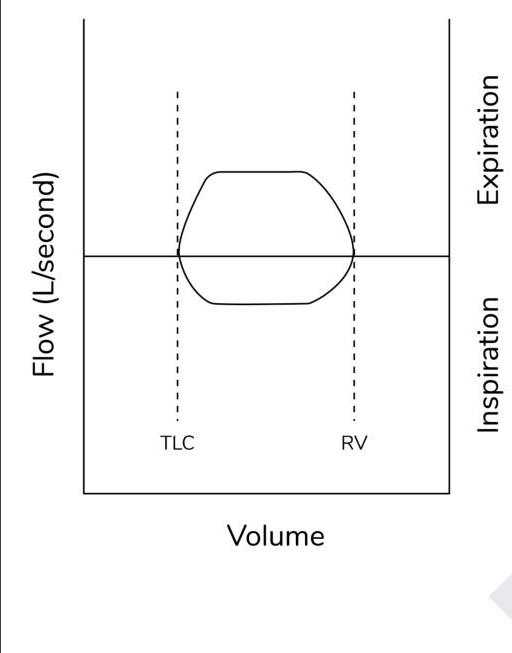
Which of the following pattern is reflected in the flow-volume curve?
Consider the following statements regarding respiratory function in old age: I. There is increasing ventilation-perfusion mismatch II. There is increased ventilatory response to hypoxia and hypercapnia III. There is a decline in maximum oxygen uptake leading to reduction in cardiorespiratory reserve IV. There is decline in the Forced Expiratory Volume to Forced Vital Capacity ratio (FEV1/FVC) by around 0.2% per year after the forties Which of the statements given above are correct?
Which of the following are the functions of larynx ? 1. Fixation of the chest 2. Aids in swallowing of food 3. Phonation 4. Respiration Select the correct answer using the code given below :
O2 (Oxygen) dissociation curve is shifted to right in the following except
What does zero pressure indicate in the pressure-volume curve?
Identify the pathology from the given flow-volume loop:
Which among the following has the highest airway resistance?
Practice by Chapter
Mechanics of Breathing
Practice Questions
Pulmonary Ventilation
Practice Questions
Pulmonary Circulation
Practice Questions
Gas Exchange in the Lungs
Practice Questions
Oxygen and Carbon Dioxide Transport
Practice Questions
Control of Breathing
Practice Questions
Respiratory Adjustments in Health and Disease
Practice Questions
High Altitude Physiology
Practice Questions
Diving Physiology
Practice Questions
Respiratory Function Tests
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
