Respiratory System — MCQs

On this page
Which time points on the Cheyne-Stokes breathing graph are associated with the highest pCO2 of lung blood and highest pCO2 of the neurons in the respiratory centre?
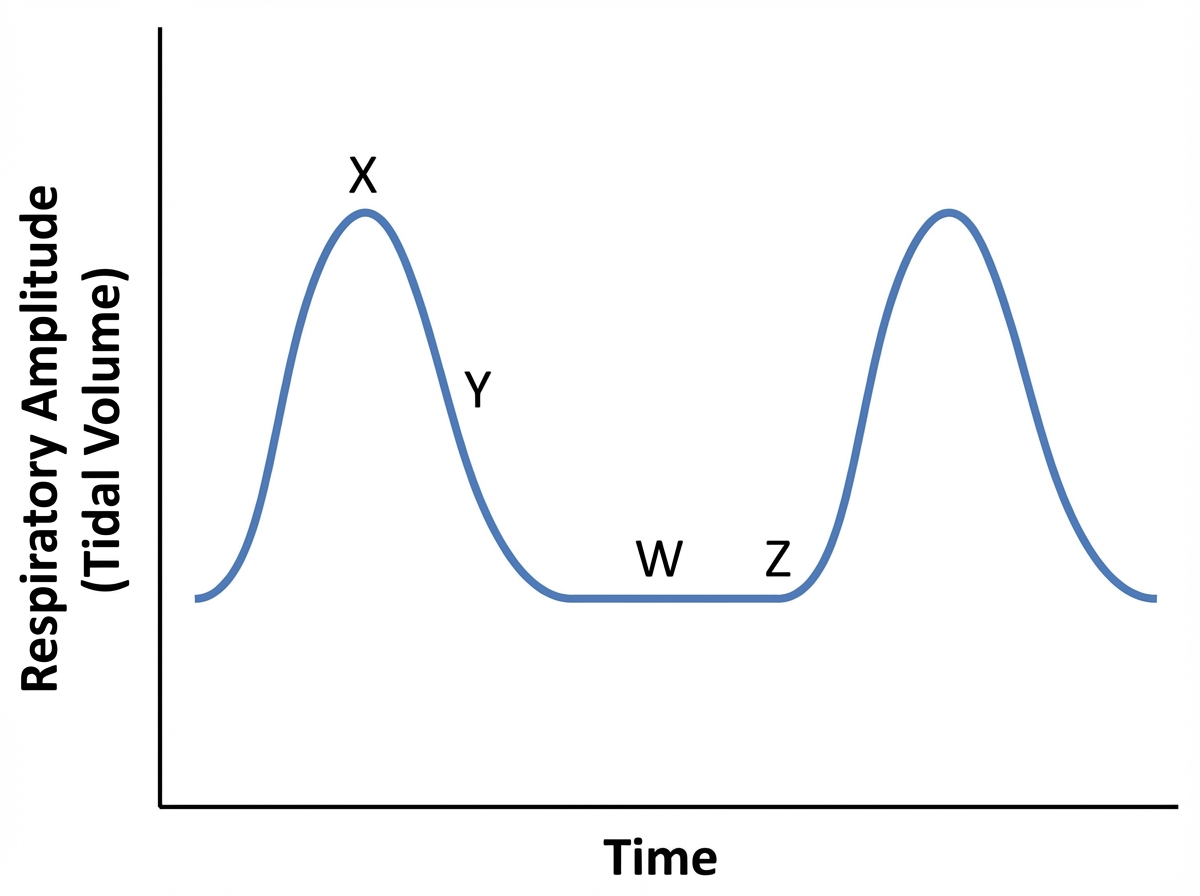
Caisson's disease is due to which of the following?
Oxygen therapy is least useful in which of the following conditions?
Most of the airway resistance is from which part of the respiratory system?
Carbon monoxide affinity to hemoglobin is how many times compared to oxygen?
What is the Haldane effect?
Decreased oxygen carrying capacity with normal partial pressure of oxygen (PO2) is a feature of which type of hypoxia?
What is the key factor in the transport of carbon dioxide as bicarbonate?
All of the following can be measured by a simple spirometer except?
Apneusis occurs when transection is at which level?
Practice by Chapter
Mechanics of Breathing
Practice Questions
Pulmonary Ventilation
Practice Questions
Pulmonary Circulation
Practice Questions
Gas Exchange in the Lungs
Practice Questions
Oxygen and Carbon Dioxide Transport
Practice Questions
Control of Breathing
Practice Questions
Respiratory Adjustments in Health and Disease
Practice Questions
High Altitude Physiology
Practice Questions
Diving Physiology
Practice Questions
Respiratory Function Tests
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
