Respiratory System — MCQs

On this page
In the ventilation-perfusion (V/Q) ratio curve for the normal lung, if the V/Q ratio is decreased, what will be the effect on pCO2 and pO2?
What causes the difference in the trajectory between the inspiratory loop and the expiratory loop in a flow-volume curve?
Pulmonary vasoconstriction is caused by:
Which of the following statements is FALSE regarding the oxygen dissociation curve?
Routine spirometry cannot estimate which of the following lung volumes or capacities?
Complex sectioning (transverse) at mid pons level along with vagi results in which of the following?
Which of the following conditions causes a leftward shift in the oxygen-hemoglobin dissociation curve?
What is the normal respiratory quotient?
Oxygen delivery to tissues in the body is cut in half by a 50% reduction in what?
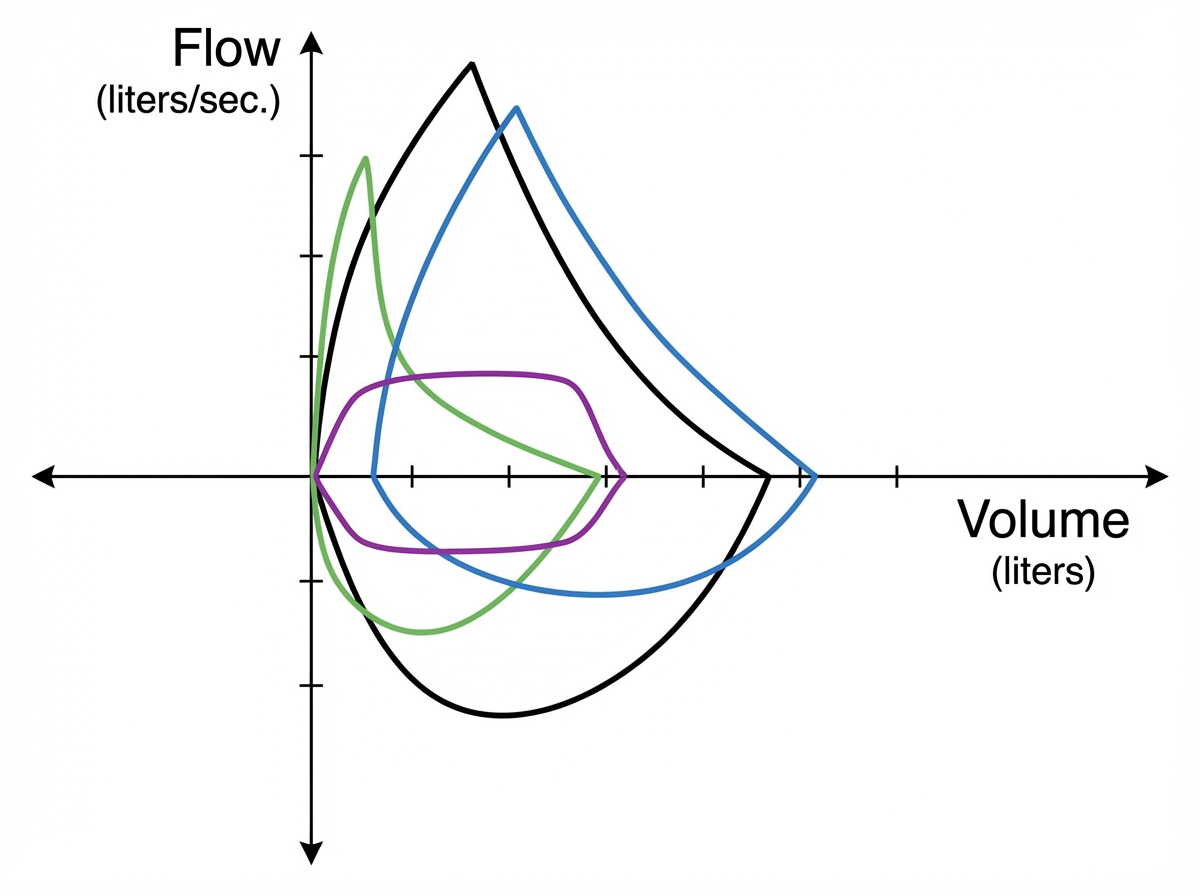
In the pulmonary function test shown in the colour palette, what does the green line represent?
Practice by Chapter
Mechanics of Breathing
Practice Questions
Pulmonary Ventilation
Practice Questions
Pulmonary Circulation
Practice Questions
Gas Exchange in the Lungs
Practice Questions
Oxygen and Carbon Dioxide Transport
Practice Questions
Control of Breathing
Practice Questions
Respiratory Adjustments in Health and Disease
Practice Questions
High Altitude Physiology
Practice Questions
Diving Physiology
Practice Questions
Respiratory Function Tests
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
