Respiratory System — MCQs

On this page
Which of the following is NOT true about COPD?
Tachycardia is caused by hypoxia due to which of the following mechanisms?
Which of the following is used to measure the resistance in small airways?
What is the normal pulmonary capillary pressure?
In an asthmatic patient, which of the following pulmonary functions would show the greater improvement on inhaling a bronchodilator?
Select the best statement regarding the respiratory centers.
What is the Haldane effect?
At which gestational age does surfactant production in the lungs begin?
What is the characteristic of type-II respiratory failure?
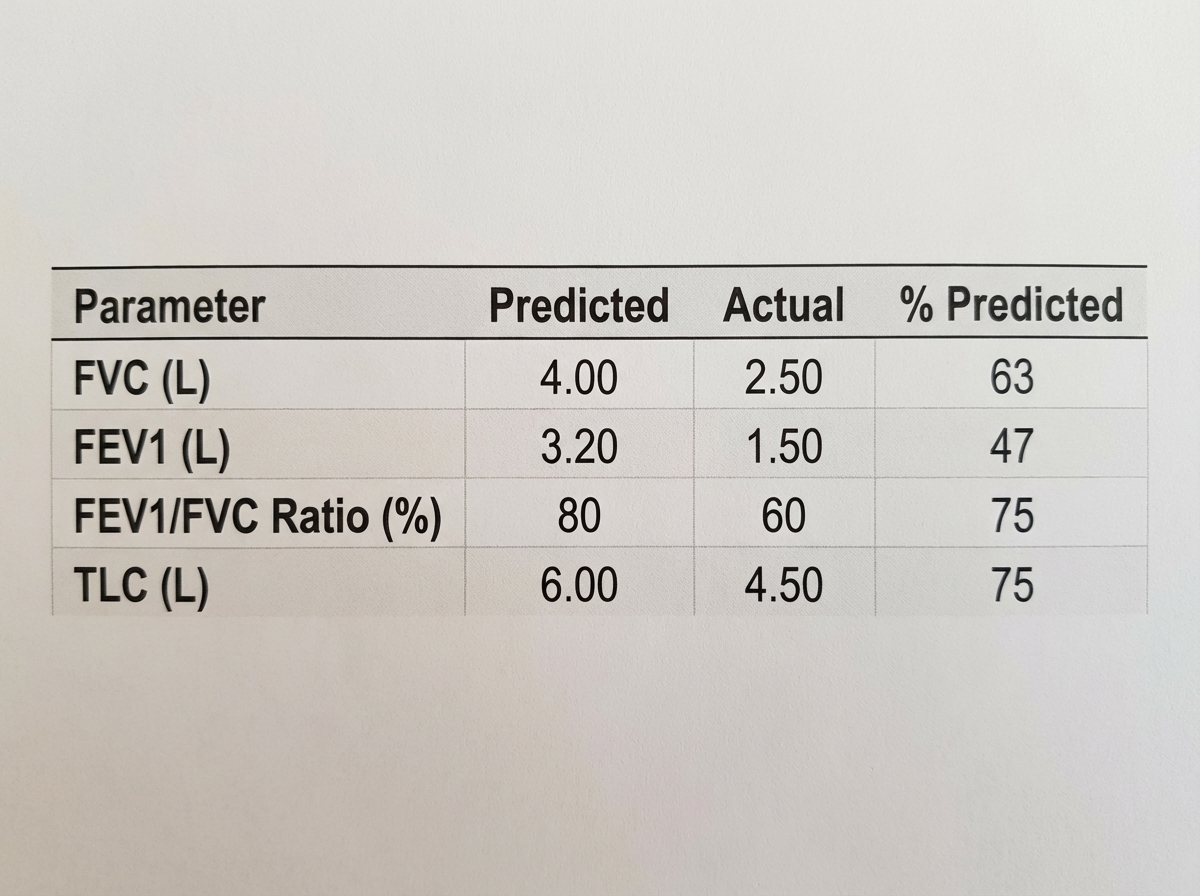
A 64-year-old woman presents with complaints of dyspnea and orthopnea. She is a lifelong non-smoker. Her pulmonary function testing is as follows. What is the most probable diagnosis?
Practice by Chapter
Mechanics of Breathing
Practice Questions
Pulmonary Ventilation
Practice Questions
Pulmonary Circulation
Practice Questions
Gas Exchange in the Lungs
Practice Questions
Oxygen and Carbon Dioxide Transport
Practice Questions
Control of Breathing
Practice Questions
Respiratory Adjustments in Health and Disease
Practice Questions
High Altitude Physiology
Practice Questions
Diving Physiology
Practice Questions
Respiratory Function Tests
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
