Reproductive Physiology — MCQs

On this page
Gonadotropin levels decline to prepubertal levels by age
Sperm acquires motility in:
At the time point indicated by the arrow, the hormone levels are:
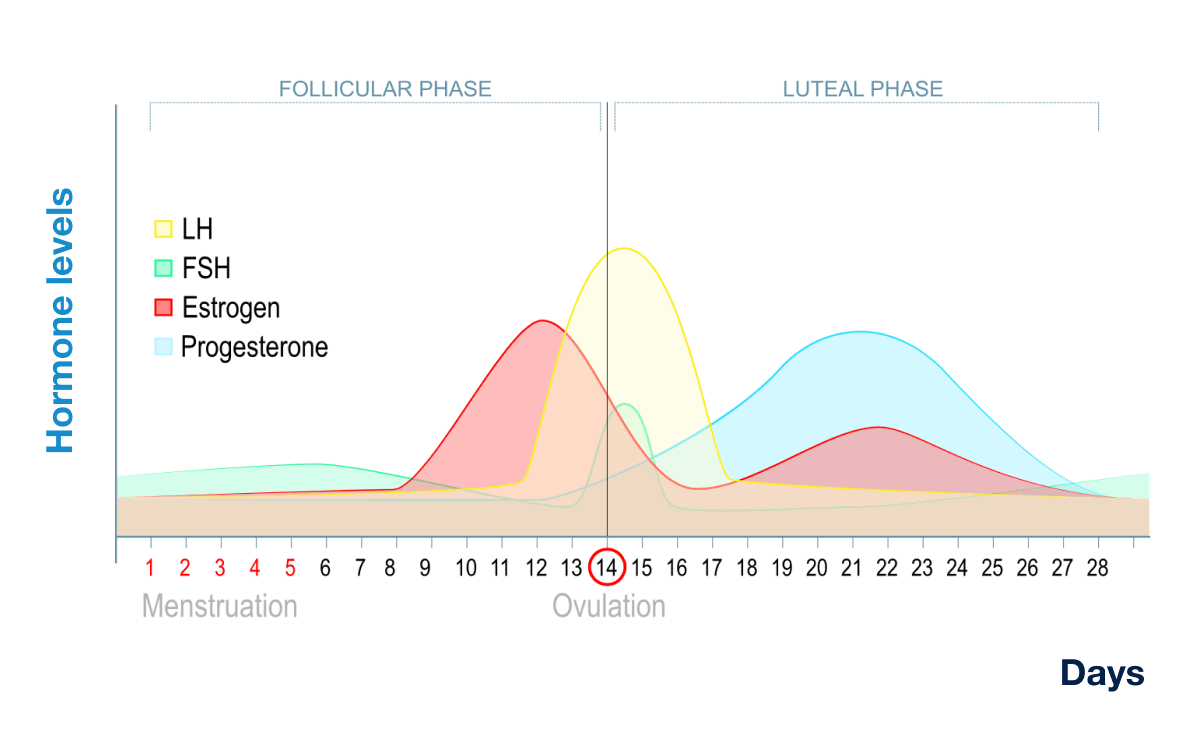
Sertoli cells secrete ?
A major function of the epididymis is:
Spermatogenesis occurs at which temperature condition?
First sign of pubertal development in a female is ?
Which of the following is not secreted by Sertoli cells?
Order of development of secondary sexual characteristic in male –
Sertoli cells play a key role in which of the following processes?
Practice by Chapter
Male Reproductive Physiology
Practice Questions
Spermatogenesis and Sperm Function
Practice Questions
Female Reproductive Physiology
Practice Questions
Menstrual Cycle
Practice Questions
Ovulation and Fertilization
Practice Questions
Physiology of Pregnancy
Practice Questions
Parturition
Practice Questions
Lactation
Practice Questions
Sexual Differentiation and Development
Practice Questions
Reproductive Aging
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
