Reproductive Physiology — MCQs

On this page
After ovulation, the oocyte is:
Absence or mutation of SRY gene results in ?
Milk production in pregnancy is inhibited by :
A 21-year-old primigravida woman visits the clinic in her 22nd week of gestation as part of her antenatal care. She has no complaints. Past medical history is unremarkable. Her only medication is a prenatal vitamin. Her temperature is 37.0°C (98.6°F), blood pressure is 110/70 mm Hg, pulse rate is 78/min, and respiration rate is 20/min. Physical examination is consistent with the gestational age of her pregnancy with no abnormalities noted. Urine dipstick is normal. Which of the following is the current primary location for fetal myelopoiesis at this stage of development?
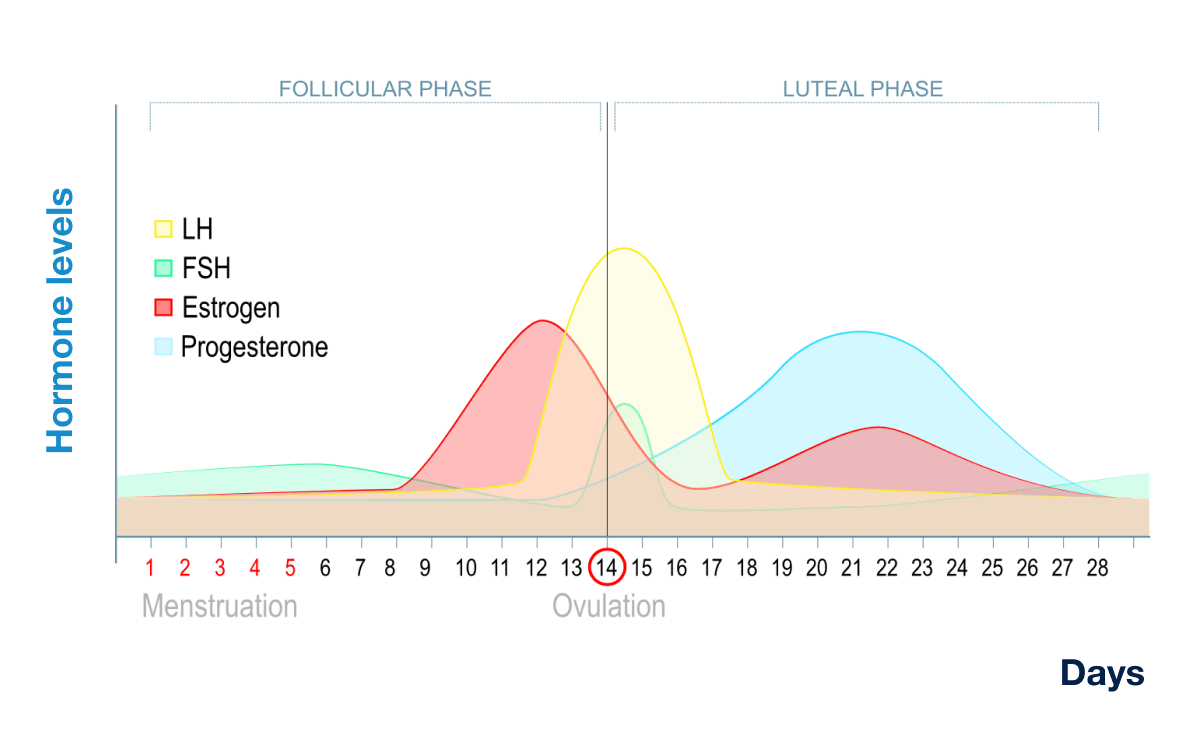
In this normal menstrual cycle graph, the mark 'X' represents levels of which hormone?
Inhibin is secreted by:
There is a mid-cycle shift in the basal body temperature (BBT) after ovulation in women. This is caused by :
Dihydrotestosterone acts on
Transplacental exchanges that take place are essential to the well being of the fetus. Which of those listed below is NOT a method?
Ovulation is primarily caused by preovulatory surge of:
Practice by Chapter
Male Reproductive Physiology
Practice Questions
Spermatogenesis and Sperm Function
Practice Questions
Female Reproductive Physiology
Practice Questions
Menstrual Cycle
Practice Questions
Ovulation and Fertilization
Practice Questions
Physiology of Pregnancy
Practice Questions
Parturition
Practice Questions
Lactation
Practice Questions
Sexual Differentiation and Development
Practice Questions
Reproductive Aging
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
