Reproductive Physiology — MCQs

On this page
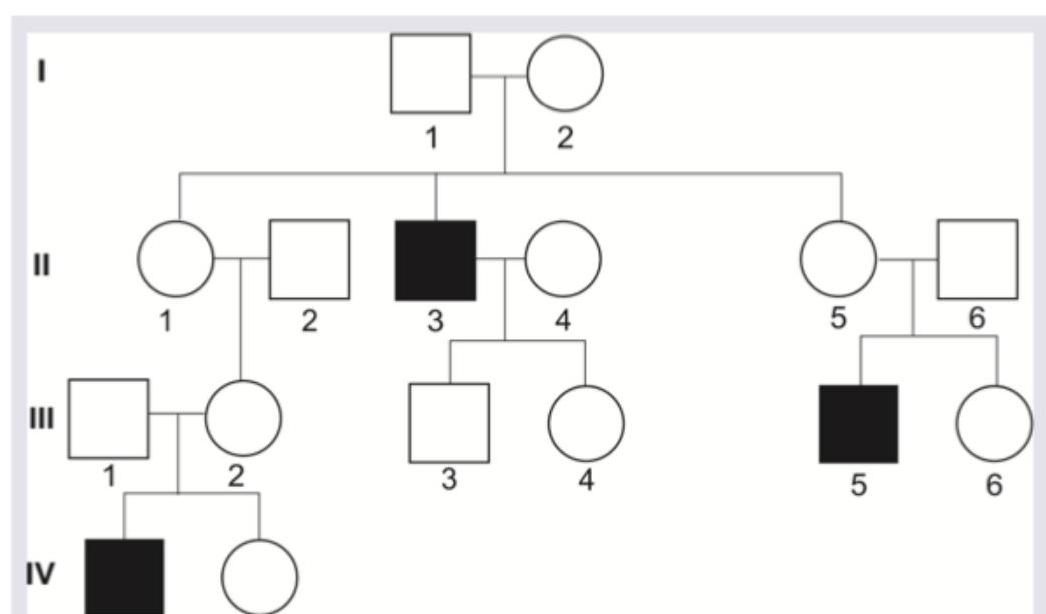
Identify the inheritance pattern shown below.
Carbohydrate metabolism in normal pregnancy shows :
Onset of labour is initiated by which of the following?
Which of the following are advantages of state of haemodilution during pregnancy? 1. Optimum gaseous exchange between maternal and foetal circulation due to decreased blood viscosity 2. Protection against adverse effect of blood loss during delivery 3. Increased oxygen carrying capacity of blood Select the correct answer using the code given below.
Which one of the following statements is correct regarding foetal physiology?
In hyperemesis gravidarum, Wernicke's encephalopathy is seen due to the deficiency of
After how many hours of LH surge does the ovulation occur?
Which one of the following statements is not correct about fetal circulation?
The ferning of cervical mucus is due to the high concentration of :
Pregnancy is characterized by the following physiological changes except :
Practice by Chapter
Male Reproductive Physiology
Practice Questions
Spermatogenesis and Sperm Function
Practice Questions
Female Reproductive Physiology
Practice Questions
Menstrual Cycle
Practice Questions
Ovulation and Fertilization
Practice Questions
Physiology of Pregnancy
Practice Questions
Parturition
Practice Questions
Lactation
Practice Questions
Sexual Differentiation and Development
Practice Questions
Reproductive Aging
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
