Renal Physiology — MCQs

On this page
Orexins are implicated in all except:
Which of the following can reduce the glomerular filtration rate (GFR)?
A 78-year-old man presents with nausea and vomiting. On examination, he appears dehydrated, his abdomen is soft, and the jugular venous pressure is not elevated. Laboratory tests reveal hypernatremia, and his calculated free water deficit is approximately 3 L. In which part of the normal kidney is most of the water reabsorbed?
Reabsorption of water is maximum in which part of the nephron?
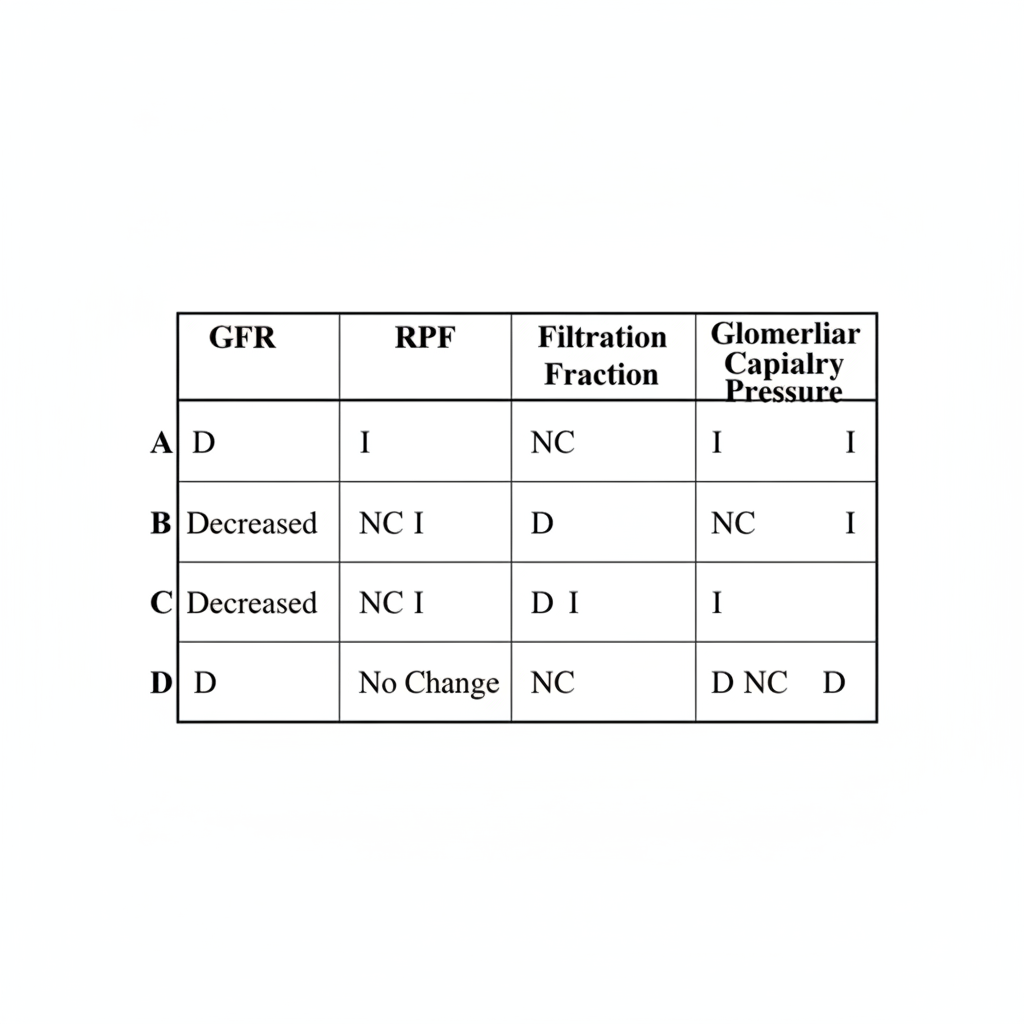
A patient is given a drug that dilates the afferent arteriole and contracts the efferent arteriole, leaving total renal vascular resistance unchanged. Which set of changes is likely to occur in the following table? (I = increased, D = decreased, NC = no change)
Which of the following does not cause relaxation of the urinary bladder?
What is the reason for the high sodium content in the renal medulla?
K+ secretion from the loop of Henle is decreased by which of the following medications?
If Renal Blood Flow is 1250 ml/min, calculate Renal Plasma Flow.
What percentage of cardiac output is supplied to the kidneys?
Practice by Chapter
Renal Blood Flow and Glomerular Filtration
Practice Questions
Tubular Reabsorption and Secretion
Practice Questions
Concentration and Dilution of Urine
Practice Questions
Acid-Base Regulation by the Kidneys
Practice Questions
Sodium and Water Balance
Practice Questions
Potassium Regulation
Practice Questions
Calcium and Phosphate Handling
Practice Questions
Micturition Physiology
Practice Questions
Renal Function Tests
Practice Questions
Integrative Responses to Fluid Challenges
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
