Renal Physiology — MCQs

On this page
What is the correct formula for calculating the Glomerular Filtration Rate (GFR)?
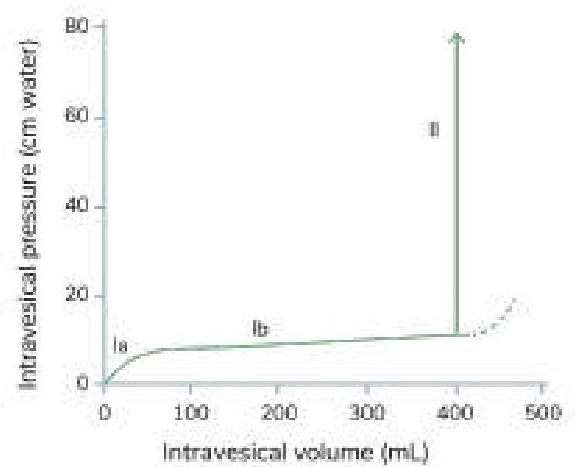
Which of the following statements is true regarding the given cystometrogram?
Impaired function of Aquaporin results in
Tubuloglomerular feedback control is useful for which one of the following?
Vasopressin acts through which aquaporin channels in the collecting duct?
Which of the following is NOT a component responsible for the counter current mechanism in the kidney?
What is the physiological response of the kidney during shock?
Tubuloglomerular feedback is for regulation of?
What is the primary function of tubuloglomerular feedback?
Which of the following is the MOST important factor determining whether a substance can be filtered at the glomerulus?
Practice by Chapter
Renal Blood Flow and Glomerular Filtration
Practice Questions
Tubular Reabsorption and Secretion
Practice Questions
Concentration and Dilution of Urine
Practice Questions
Acid-Base Regulation by the Kidneys
Practice Questions
Sodium and Water Balance
Practice Questions
Potassium Regulation
Practice Questions
Calcium and Phosphate Handling
Practice Questions
Micturition Physiology
Practice Questions
Renal Function Tests
Practice Questions
Integrative Responses to Fluid Challenges
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
