Neurophysiology — MCQs

On this page
Depolarization in myelinated axons jumps from one node of Ranvier to the next. This process is known as:
A patient diagnosed with depression responds well to MAO inhibitors. Which neurotransmitter is deficient in this patient, and from which structure is it primarily produced?
Pathology of which system can lead to disorders of the autonomic nervous system?
What structures form the blood-brain barrier?
Sympathetic stimulation causes all except?
Which of the following is not a feature of spinal cord reflex?
Under normal physiological conditions, CSF pressure is proportional to which of the following factors?
Delta waves on EEG are recorded in which stage of sleep?
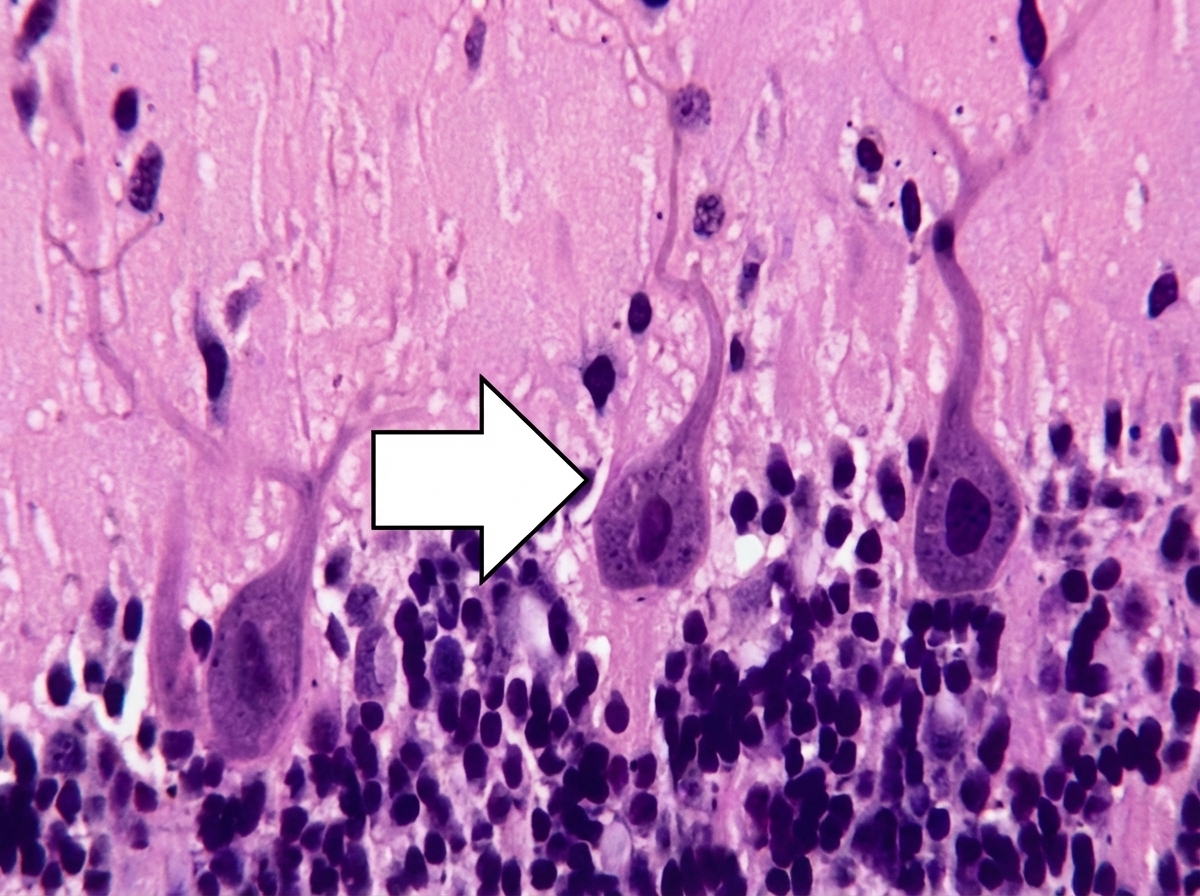
The marked cell inhibits which of the following structure?
What is the effect of axon thickening on nerve impulse conduction speed?
Practice by Chapter
Neurons and Glial Cells
Practice Questions
Synaptic Transmission
Practice Questions
Sensory Processing
Practice Questions
Motor Control Systems
Practice Questions
Autonomic Nervous System
Practice Questions
Hypothalamus and Limbic System
Practice Questions
Cerebral Cortex Functions
Practice Questions
Electroencephalography
Practice Questions
Neuroplasticity
Practice Questions
Sleep and Wakefulness
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
