Nerve and Muscle Physiology — MCQs

On this page
A 35-year-old man wakes up after sleeping with his arm draped over a chair and complains of pain. Which of the following accurately describes the order of susceptibility of nerve fibers in the given condition?
Which of the following ion movements is primarily responsible for the repolarization phase (Phase 3) of an action potential, as depicted in the image?
What best describes step 3 in the given diagram?
Which of the following changes occurs during muscle contraction while exercising, as shown in the image?
A single muscle twitch lasts 40 milliseconds. What is the minimum tetanization frequency required to produce a sustained (fused) contraction in this muscle?
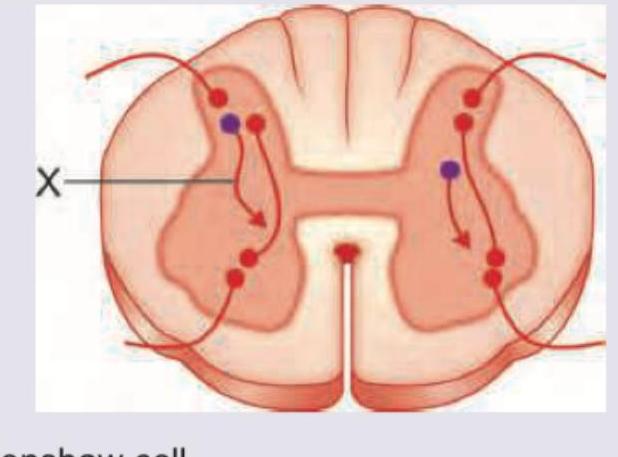
Name the interneuron marked X in colour purple involved in tetanus. (Recent NEET Pattern 2016-17)
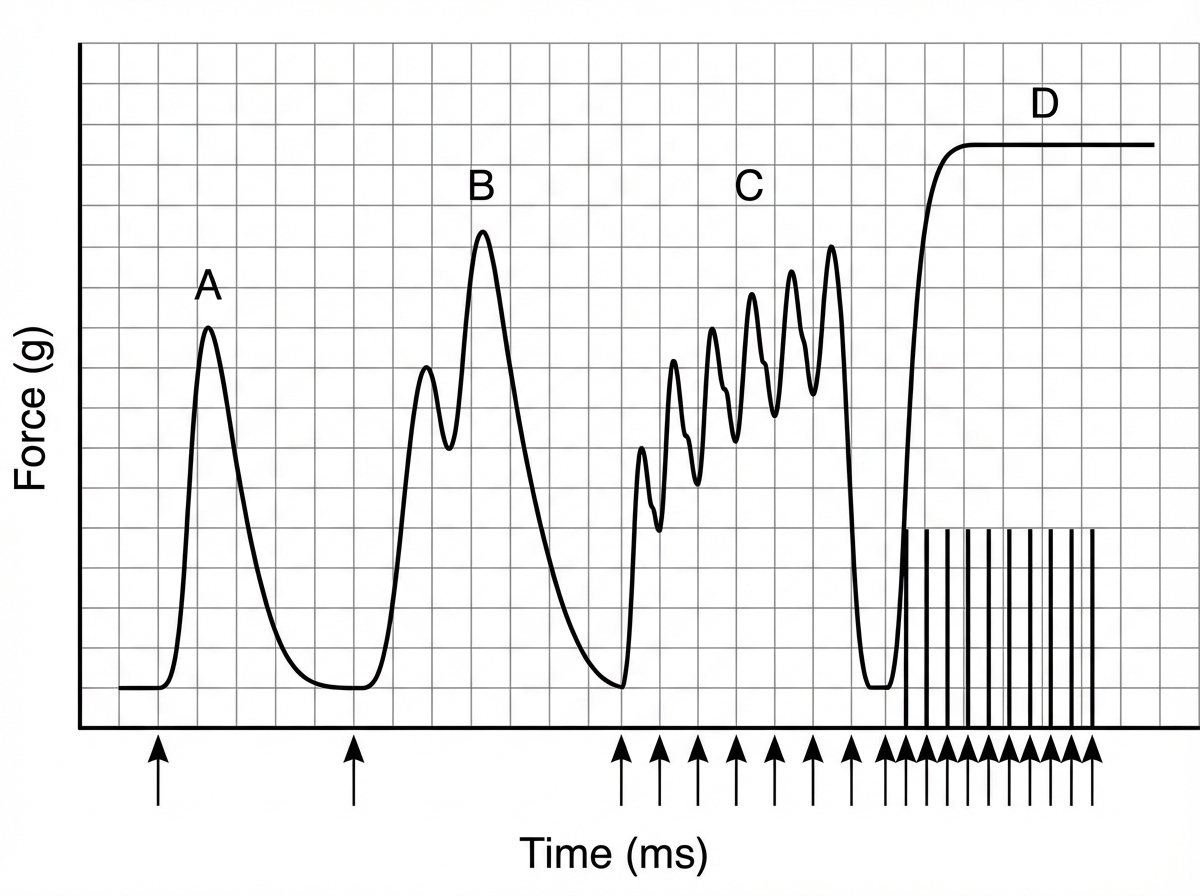
The following skeletal muscle recording shows presence of: (Recent NEET Pattern 2016-17)
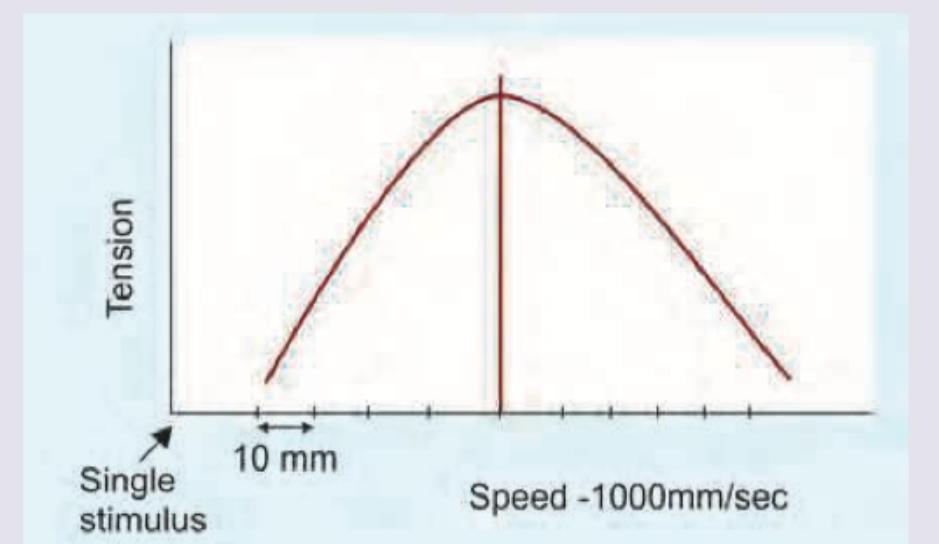
The fiber marked as X is:

Calculate the tetanizing frequency based on the contraction dynamics of gastrocnemius muscle of frog shown in the image?
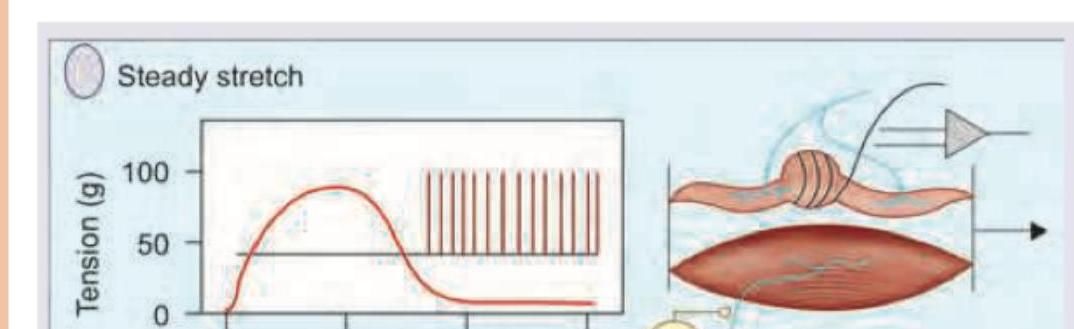
In the process shown below stretch stimulus is mediated by which of the following receptors?
Practice by Chapter
Resting Membrane Potential
Practice Questions
Action Potential Generation and Propagation
Practice Questions
Neuromuscular Junction
Practice Questions
Skeletal Muscle Contraction
Practice Questions
Smooth Muscle Physiology
Practice Questions
Cardiac Muscle Properties
Practice Questions
Muscle Metabolism and Fatigue
Practice Questions
Motor Unit Function
Practice Questions
Neurotransmitters and Receptors
Practice Questions
Electrophysiological Measurements
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
