Gastrointestinal System — MCQs

On this page
Which of the cells labelled below secrete hydrochloric acid?
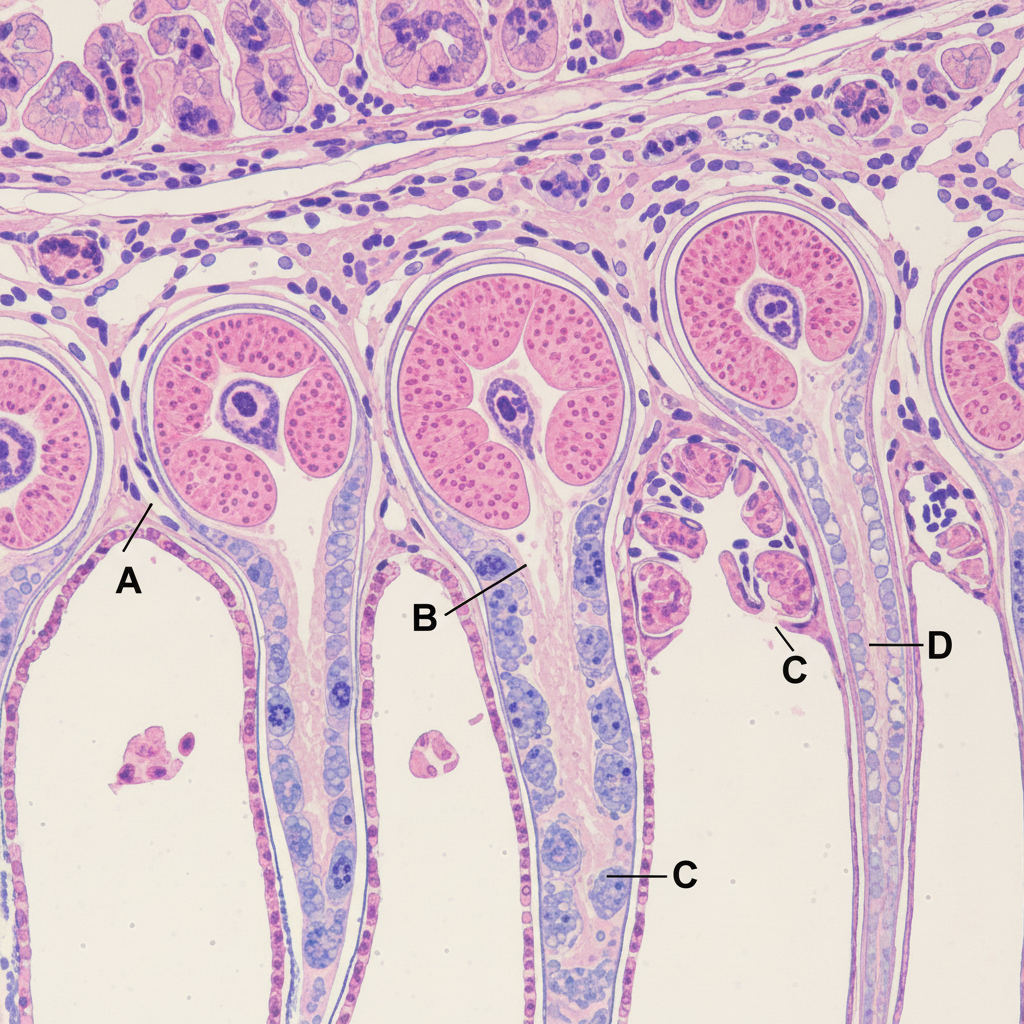
Which of the following are functions of the gall bladder? I. Reservoir for bile II. Production of bile III. Secretion of mucus IV. Concentration of bile Select the correct answer using the code given below :
Iron is absorbed predominantly in the
With reference to the role of fibre in diet, consider the following statements: 1. It inhibits faecal mutagen synthesis. 2. It reduces post-prandial glucose. 3. It decreases the transit time of food in the bowel. Which of the above represent(s) the role of fibre in our diet?
Which transporter is responsible for the absorption of glucose in the intestine when a person is given Oral Rehydration Solution (ORS)?
A child presented with dehydration and was supplemented with ORS solution for management. Which of the following transporters help in the absorption of glucose from GIT?
A woman must vomit whenever she eats spicy food. Arrange the sequence of events during vomiting. 1. LES is open and UES is closed 2. Strong contractions in the stomach 3. Inspiration against a closed glottis 4. Relaxation of the pyloric sphincter 5. LES opens and UES opens 6. Reverse peristalsis in the small intestine LES: Lower esophageal sphincter UES: Upper esophageal sphincter
All of the following increases gastric acid secretion except?
The relaxation of the intestinal segment distal to the segment with the bolus of food during peristalsis is because of?
Which neurotransmitter primarily mediates slow synaptic transmission in the enteric nervous system?
Practice by Chapter
Gastrointestinal Motility
Practice Questions
Gastrointestinal Secretions
Practice Questions
Digestion and Absorption
Practice Questions
Gastrointestinal Hormones
Practice Questions
Hepatobiliary Physiology
Practice Questions
Pancreatic Exocrine Function
Practice Questions
Gastrointestinal Circulation
Practice Questions
Intestinal Immune System
Practice Questions
Gut Microbiome
Practice Questions
Regulation of Food Intake
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
