Endocrinology — MCQs

On this page
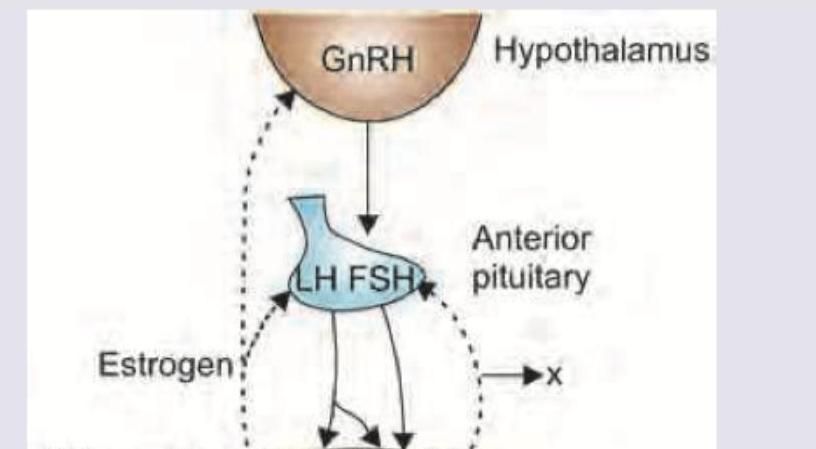
Which of the following mechanisms is used by the marked structure to influence neighboring cells?
Which of the following tissues will not be able to take up glucose in insulin resistance/insulin absence/diabetes mellitus?
Which of the following is correct about the feedback hormone marked as $X$ ?
Which of the following represents a normal response to an OGTT?
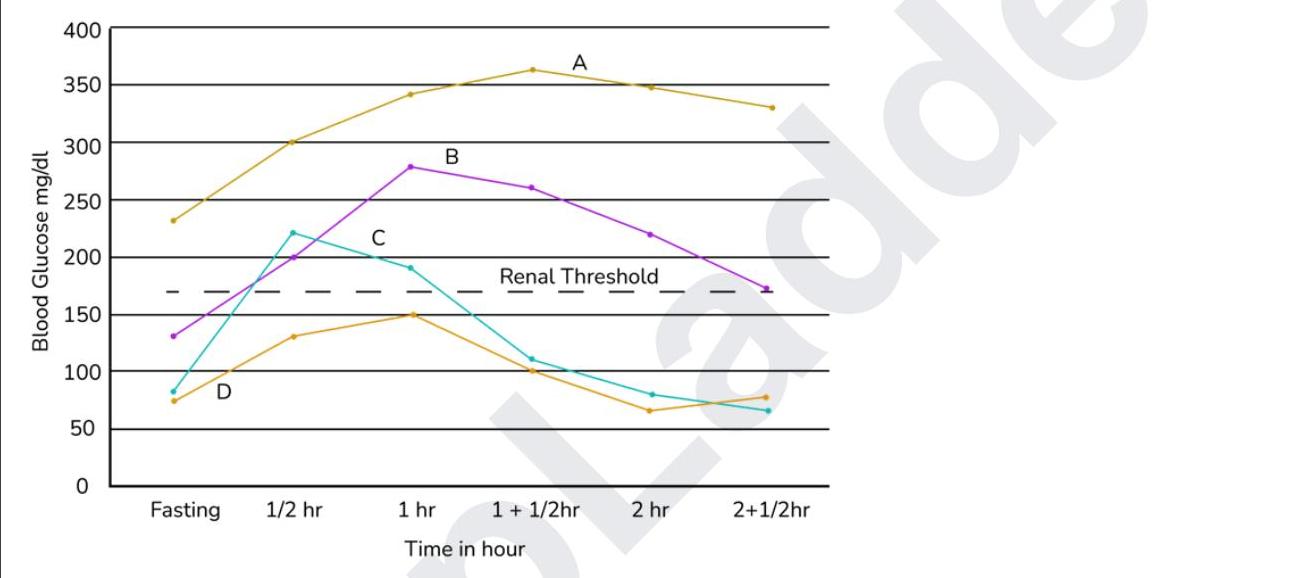
Which of the following is the primary tissue dependent on insulin for glucose uptake?
Which hormone most strongly stimulates gluconeogenesis during prolonged fasting?
Which hormone is primarily responsible for initiating milk production postpartum?
A 20-year-old college student has elevated stress levels due to her rigorous academic schedule, social commitments, and family pressures. She complains of never having enough time for all her responsibilities. Which of the following hormones acts by intracellular receptors to exert the physiologic effects of her stress?
Which of the following hormones regulates blood levels of 1,25-OH-cholecalciferol positively?
Testosterone is secreted by:
Practice by Chapter
Principles of Endocrine Regulation
Practice Questions
Hypothalamus and Pituitary Gland
Practice Questions
Thyroid Physiology
Practice Questions
Adrenal Cortex and Medulla
Practice Questions
Pancreatic Hormones and Glucose Metabolism
Practice Questions
Calcium and Phosphate Homeostasis
Practice Questions
Growth Hormone and Growth Factors
Practice Questions
Endocrine Regulation of Metabolism
Practice Questions
Hormone Receptors and Signaling
Practice Questions
Assessment of Endocrine Function
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
