Endocrinology — MCQs

On this page
Which hormone inhibits both FSH and LH?
Which of the following is associated with a reduction of cAMP in the serum?
The provided diagram shows the adrenal gland. Identify the hormone produced from the area labeled 'A'.
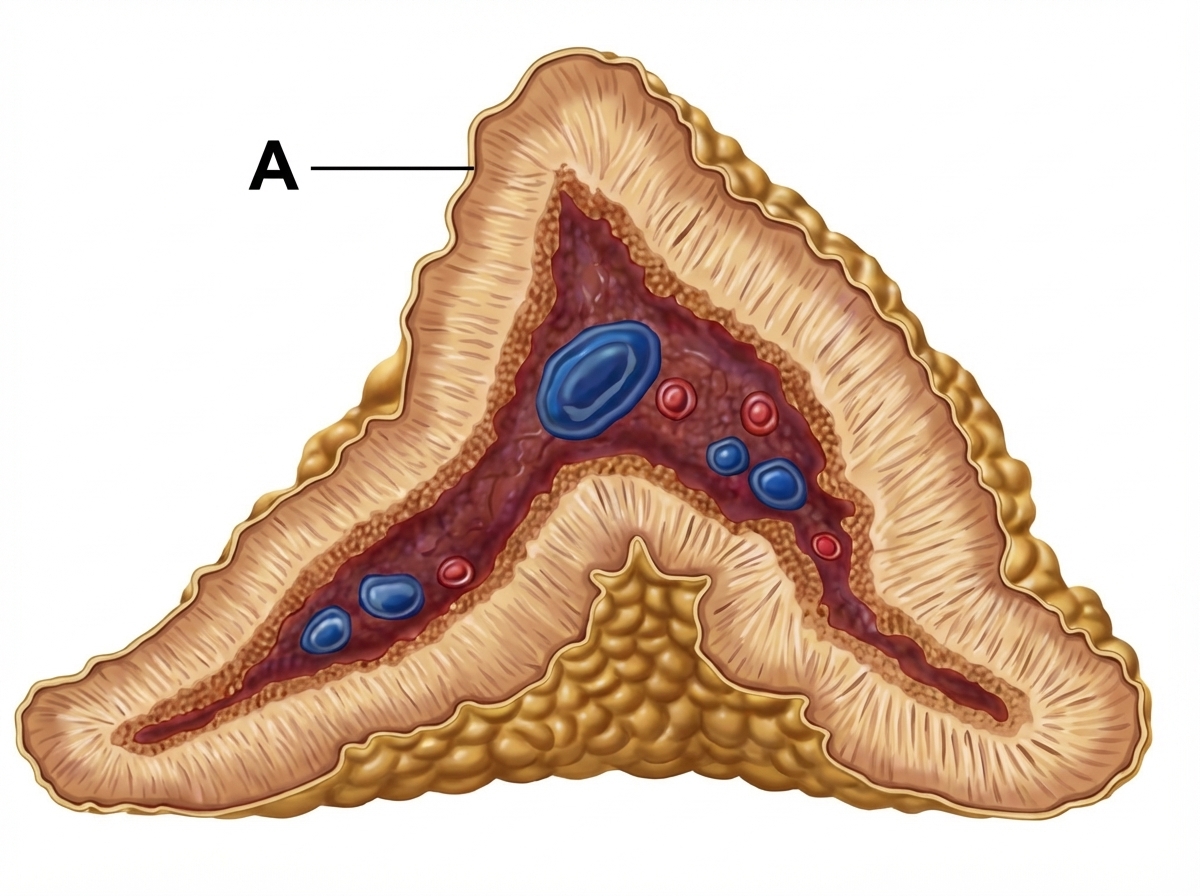
Which of the following is both synthesized and stored in the hypothalamus?
Which finding would be present following selective destruction of Sertoli cells?
Vasopressin is secreted by which nucleus of the hypothalamus?
Obesity is ordinarily associated with low ghrelin levels. Which of the following conditions is an exception where obesity is associated with high ghrelin levels?
Cholecystokinin is mainly secreted by which part of the gastrointestinal tract?
Hypercalcemia is caused by all of the following except?
Lesion of which hypothalamic nuclei leads to loss of circadian rhythm?
Practice by Chapter
Principles of Endocrine Regulation
Practice Questions
Hypothalamus and Pituitary Gland
Practice Questions
Thyroid Physiology
Practice Questions
Adrenal Cortex and Medulla
Practice Questions
Pancreatic Hormones and Glucose Metabolism
Practice Questions
Calcium and Phosphate Homeostasis
Practice Questions
Growth Hormone and Growth Factors
Practice Questions
Endocrine Regulation of Metabolism
Practice Questions
Hormone Receptors and Signaling
Practice Questions
Assessment of Endocrine Function
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
