Electrolytes and Body Fluids — MCQs

On this page
Body water content as a percentage of body weight is lowest in which of the following groups?
ECF volume assessment can be most accurately done by which substance?
Edema is due to which of the following factors?
Which of the following is an intracellular constituent of the neuromuscular system?
What does 0.9% NaCl solution contain?
Muscular weakness due to magnesium deficiency is enhanced by the presence of which condition?
Arrange the following according to increasing order of their total body water as a percentage of body weight: 1. 6-month-old baby 2. Neonate 3. Young female 4. Young male
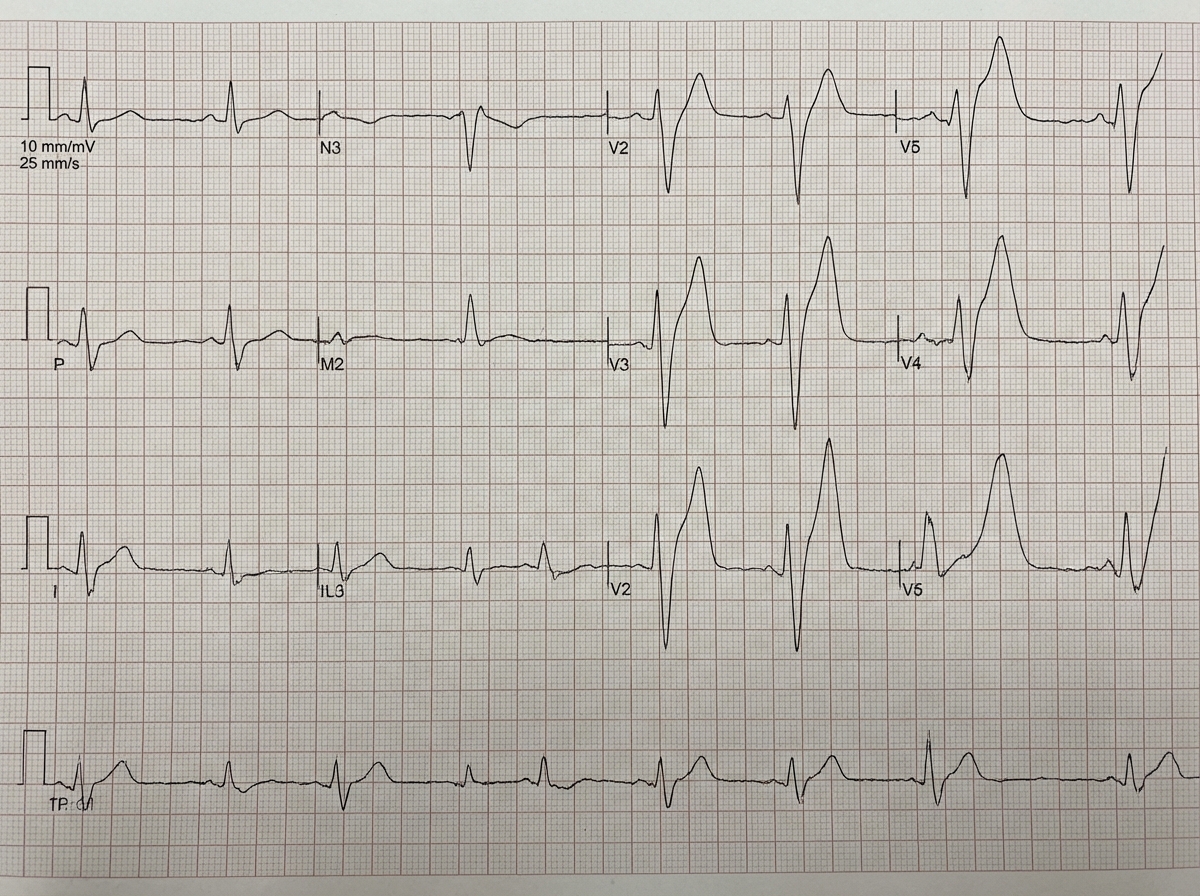
Which of the following conditions is characterized by these ECG changes?
Edema may be caused by any of the following, EXCEPT:
Plasma constitutes what percentage of body weight?
Practice by Chapter
Body Fluid Compartments and Composition
Practice Questions
Osmolality and Tonicity
Practice Questions
Sodium and Water Balance
Practice Questions
Potassium Homeostasis
Practice Questions
Calcium and Phosphate Regulation
Practice Questions
Magnesium Metabolism
Practice Questions
Fluid Shifts Between Compartments
Practice Questions
Edema Formation Mechanisms
Practice Questions
Dehydration Physiology
Practice Questions
Disorders of Electrolyte Balance
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
