Electrolytes and Body Fluids — MCQs

On this page
Extracellular fluid includes all except?
What are the major symptoms of hypernatremia?
What is true about hyperkalemia?
Edema occurs when plasma protein level falls below which value?
Hyperkalemia can occur in all of the following conditions, except?
What percentage of body weight does total body water constitute?
Osmolality of plasma is mainly contributed by?
Dehydration is more severe in infants compared to adults. What is the PRIMARY reason for this increased susceptibility?
Which of the following is the principal constituent of serum osmolality?
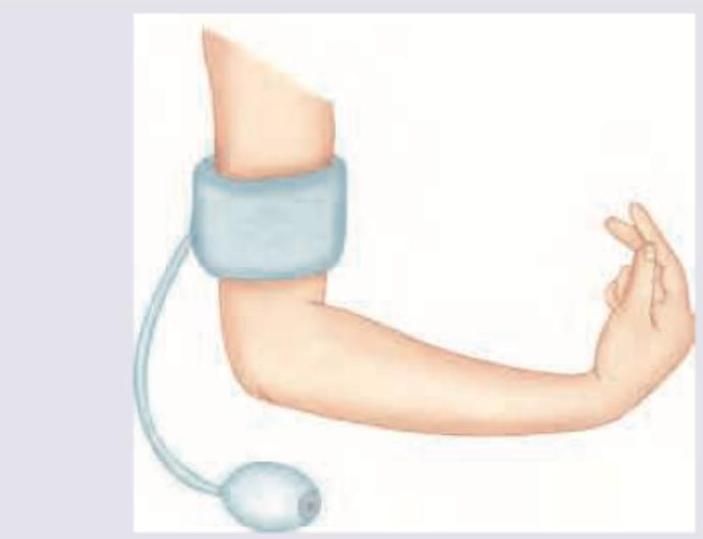
In a child with suspected tetany, the following test is performed. Identify the sign?
Practice by Chapter
Body Fluid Compartments and Composition
Practice Questions
Osmolality and Tonicity
Practice Questions
Sodium and Water Balance
Practice Questions
Potassium Homeostasis
Practice Questions
Calcium and Phosphate Regulation
Practice Questions
Magnesium Metabolism
Practice Questions
Fluid Shifts Between Compartments
Practice Questions
Edema Formation Mechanisms
Practice Questions
Dehydration Physiology
Practice Questions
Disorders of Electrolyte Balance
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
