Emergency Pharmacology — MCQs

On this page
Which of the following conditions can the shown injection be used for emergency management?
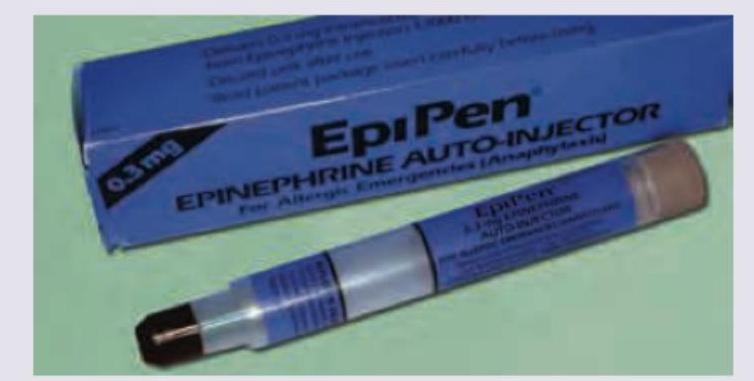
A 3-year-old child presents with febrile seizures. All are correct about the route of drug administered except:
A child with acute lymphoblastic leukemia was given Vincristine in V.A.L.P regimen. However there was an extravasation of the drug. All should be done for management of the same except?
Which of the following statements are correct regarding the use of benzodiazepines in the initial management of status epilepticus? I. Upto two doses may be used 5 minutes apart, if seizures are not controlled II. For Lorazepam, only a single dose should be used, even if seizures are not controlled III. Dose of midazolam at this stage is 1-15 mcg / kg / min infusion IV. Dose of both lorazepam and midazolam is 0.1 mg / kg Select the answer using the code given below :
What is the antidote for belladonna poisoning?
What is the drug of choice for emergency contraception ?
Which of the following drugs is not used for the emergency (immediate) management of hyperkalaemia?
A patient presented with dizziness, cool clammy skin, pinpoint pupil with blue lips and fingernails suffering from respiratory depression. The patient was producing a pink frothy sputum on coughing. The drug used to reverse the effects is?
A female was given morphine sulphate during labour for pain but she developed respiratory distress. Which of the following will be the correct antidote?
A 55-year-old man presents to the emergency department with acute confusion, visual disturbances, and difficulty breathing. His wife reports he was working with industrial cleaning supplies in an unventilated space. Laboratory analysis reveals severe metabolic acidosis and elevated anion gap. Which of the following antidotes should be administered immediately?
Practice by Chapter
Management of Anaphylaxis
Practice Questions
Drugs in Cardiac Arrest
Practice Questions
Status Epilepticus Management
Practice Questions
Acute Stroke Therapeutics
Practice Questions
Toxicological Emergencies
Practice Questions
Antidotes in Emergency Medicine
Practice Questions
Pain Management in Emergency
Practice Questions
Sedation and Paralysis in Emergency
Practice Questions
Drugs in Traumatic Emergencies
Practice Questions
Thrombolysis in Emergency Settings
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
