Emergency Pharmacology — MCQs

On this page
A young man is prescribed parenteral antibiotics for a respiratory tract infection. He collapses immediately after receiving the first dose, presenting with tachycardia, wheezing, and a drop in blood pressure. What are the most appropriate immediate interventions for this situation?
Calcium gluconate is not indicated in the management of which of the following conditions during CPR?
What is the drug of choice in the management of a life-threatening allergic reaction?
Oxygen as an emergency drug is contraindicated in which of the following conditions?
A patient who has undergone limb amputation is advised a stress test. What is the drug commonly used for this test?
Which drug should NOT be used in a patient with hyperkalemia and no ECG findings?
What is the drug of choice for anaphylactic shock?
A patient is brought to the emergency department with signs suggesting opioid poisoning. What is the antidote of choice?
What is the concentration of adrenaline used in the following route of administration?
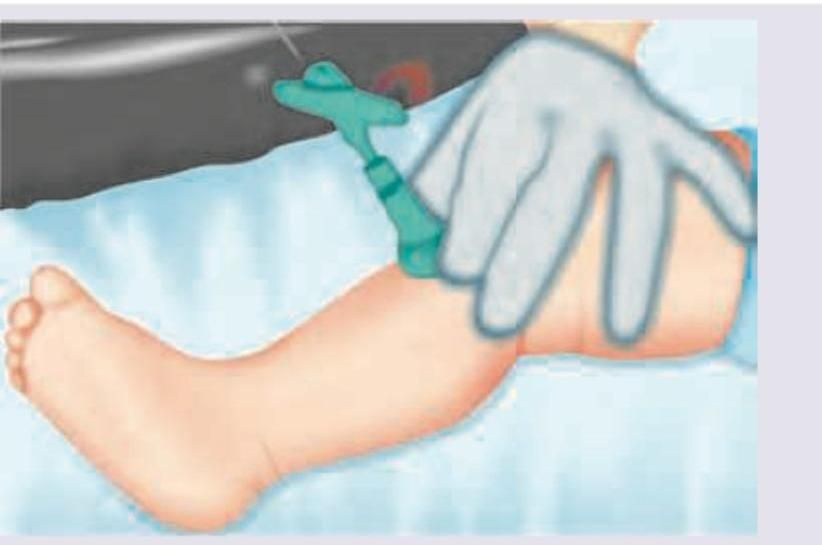
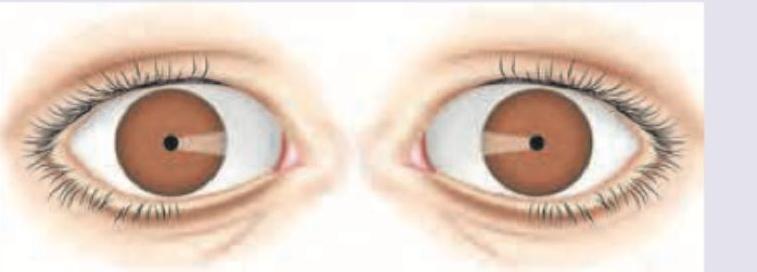
A comatose person is brought to the hospital. On examination his respiratory rate is 8 / min with pulse rate of 75 bpm with BP of 110 / 70 mm Hg. His Pupils are shown below. Body temperature is 96°F. What is the probable diagnosis?
Practice by Chapter
Management of Anaphylaxis
Practice Questions
Drugs in Cardiac Arrest
Practice Questions
Status Epilepticus Management
Practice Questions
Acute Stroke Therapeutics
Practice Questions
Toxicological Emergencies
Practice Questions
Antidotes in Emergency Medicine
Practice Questions
Pain Management in Emergency
Practice Questions
Sedation and Paralysis in Emergency
Practice Questions
Drugs in Traumatic Emergencies
Practice Questions
Thrombolysis in Emergency Settings
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
