Drugs in Psychiatric Disorders — MCQs

On this page
What class of medication is used to treat schizophrenia?
Regarding the use of Lithium in maniac-depressive psychosis, what is the true statement?
Which of the following is an atypical antipsychotic with the least metabolic side effects?
A patient was given an antipsychotic drug, haloperidol, and the patient developed acute dystonia. Which is the next best step?
A 12-year-old child presents with palpitations, tremors, dry mouth, heart rate 130 bpm, respiratory rate 34/min. Which of the following substances is most likely responsible?
A patient with schizophrenia, developed muscular dystonia and was treated for it. The patient now presents with complaints of dry mouth, dizziness, and hypotension. What is the most likely drug causing these side effects?
A 38-year-old professor with depression requests you to prescribe an antidepressant that would be least likely to cause sexual dysfunction. Which of the following drugs would you prescribe?
A psychiatrist prescribes lithium for a patient who is diagnosed with bipolar disorder. Which of the following statements is incorrect regarding lithium?
Which of the following psychoactive substances is a new, rapidly acting antidepressant?
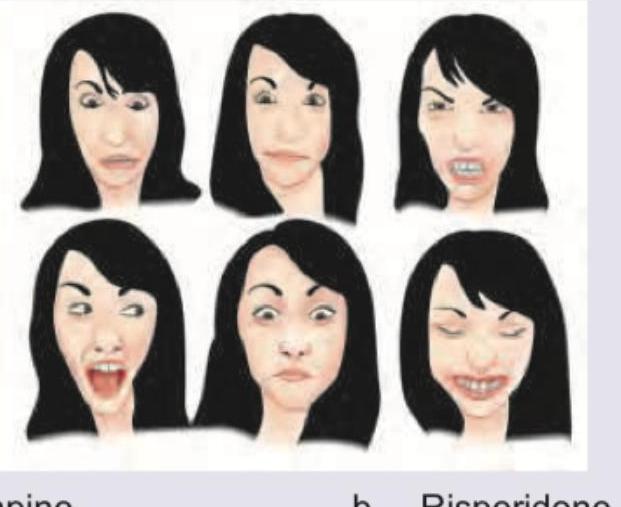
Which drug has propensity to cause such involuntary movements?
Practice by Chapter
Antipsychotics: Typical and Atypical
Practice Questions
Antidepressants: SSRIs and SNRIs
Practice Questions
Tricyclic Antidepressants
Practice Questions
MAO Inhibitors
Practice Questions
Mood Stabilizers
Practice Questions
Anxiolytics
Practice Questions
Drugs for ADHD
Practice Questions
Drugs for Sleep Disorders
Practice Questions
Drugs for Dementia
Practice Questions
Drug-Induced Psychiatric Symptoms
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
