Drugs for Gastrointestinal Diseases — MCQs

On this page
What is the drug of choice for the medical management of bleeding esophageal varices?
Which drug is NOT used in the treatment of H. pylori infection?
What is true regarding sulfasalazine?
What is the drug of choice for antibiotic-associated pseudomembranous colitis?
Levosulpiride acts as an antagonist of which central dopamine receptor?
Teduglutide is used in small bowel syndrome because its action is similar to which of the following?
Which of the following is a 5-HT3 antagonist?
Which of the following is a prokinetic drug?
What is the preferred drug for controlling an acute exacerbation of ulcerative colitis?
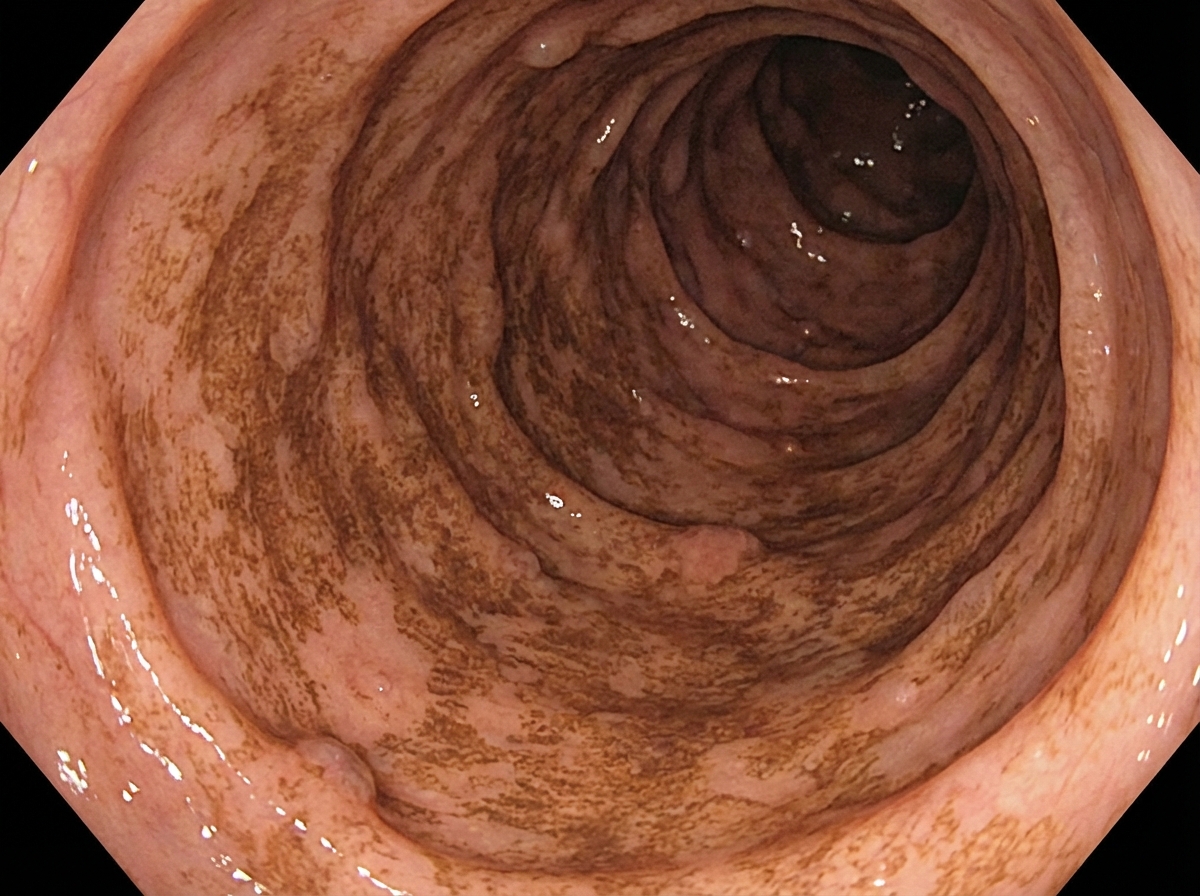
The following adverse drug reaction seen in colonoscopy view is due to which of the following agents?
Practice by Chapter
Acid-Peptic Disease Therapeutics
Practice Questions
Proton Pump Inhibitors
Practice Questions
H2 Receptor Antagonists
Practice Questions
Antacids and Mucosal Protectants
Practice Questions
Antiemetics
Practice Questions
Prokinetic Agents
Practice Questions
Laxatives and Purging Agents
Practice Questions
Antidiarrheal Drugs
Practice Questions
Drugs for Inflammatory Bowel Disease
Practice Questions
Pancreatic Enzyme Supplements
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
