Drugs for Gastrointestinal Diseases — MCQs

On this page
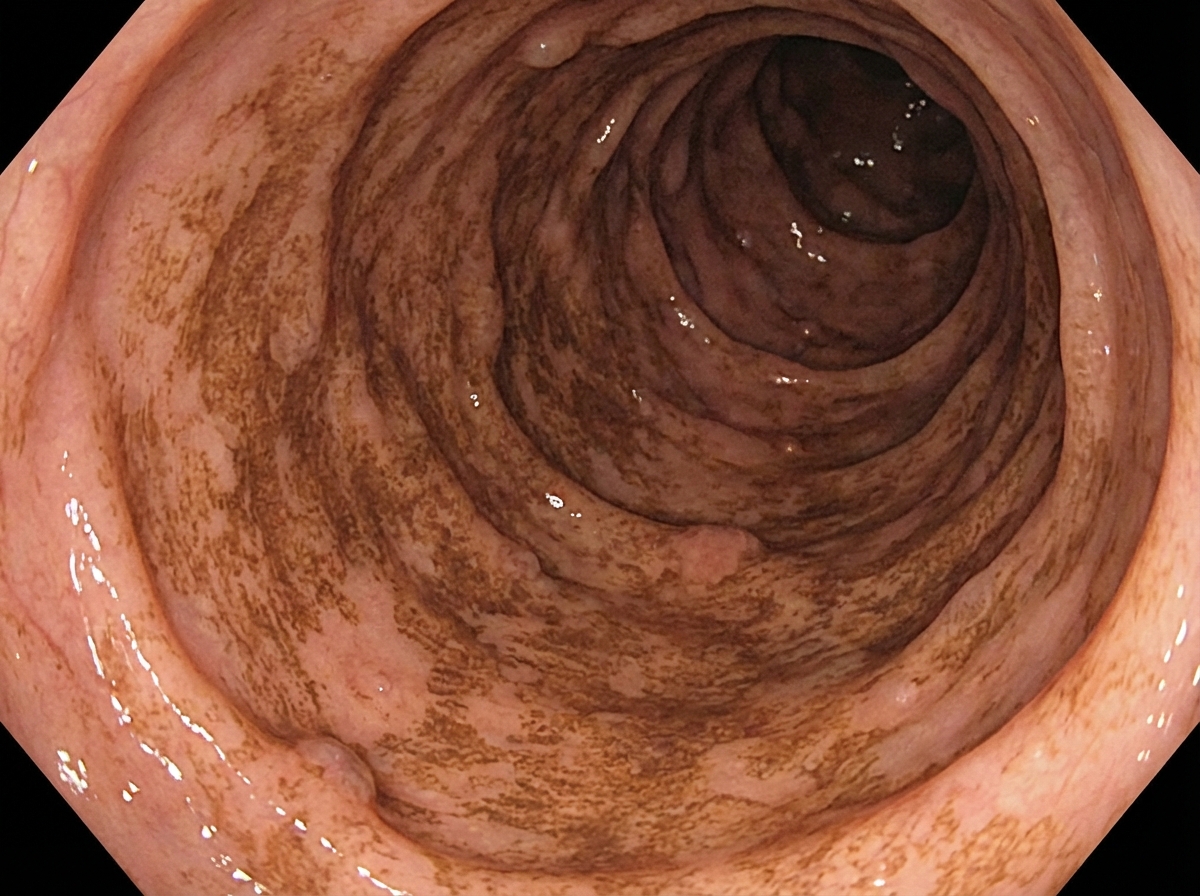
Which one of the following causes Melanosis coli?
Which of the following drugs causes the observed effect on colonoscopic view?
Which of the following is the most likely indication for the use of pirenzepine?
Which of the following is a Protein Pump Inhibitor?
Which prokinetic drug lacks D2 receptor antagonism?
Why is atropine added to commercial preparations containing diphenoxylate?
Which of the following is NOT a gastrointestinal effect of metoclopramide?
All of the following are false about Tenapanor except?
What is the drug of choice for an acute exacerbation of ulcerative colitis?
Which antibiotic improves gastroparesis?
Practice by Chapter
Acid-Peptic Disease Therapeutics
Practice Questions
Proton Pump Inhibitors
Practice Questions
H2 Receptor Antagonists
Practice Questions
Antacids and Mucosal Protectants
Practice Questions
Antiemetics
Practice Questions
Prokinetic Agents
Practice Questions
Laxatives and Purging Agents
Practice Questions
Antidiarrheal Drugs
Practice Questions
Drugs for Inflammatory Bowel Disease
Practice Questions
Pancreatic Enzyme Supplements
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
