Diuretics — MCQs

On this page
Which of the following drugs will act on X to inhibit sugar absorption from the PCT of kidney?
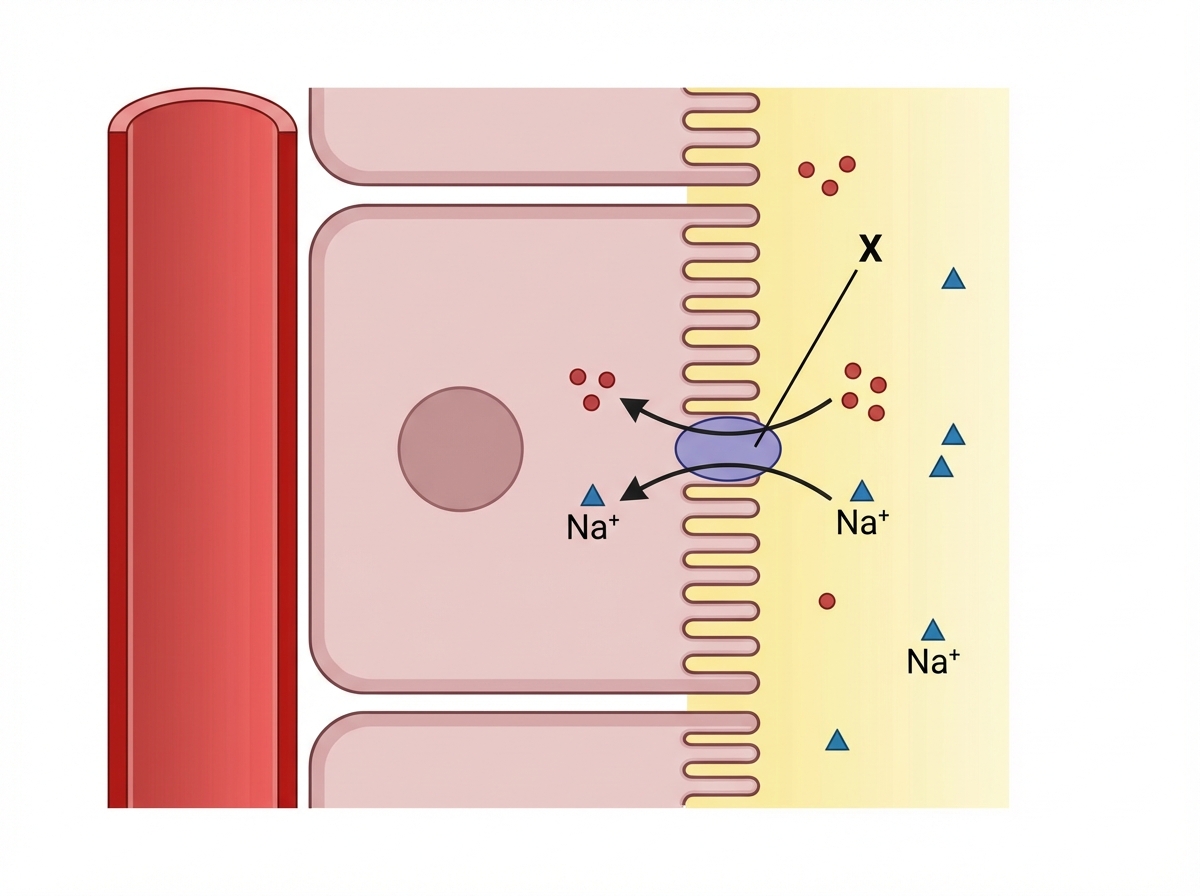
A 42-year old man with history of alcohol dependency presents with progressive abdominal distension. Abdominal examination reveals a shifting dullness. Which one of the following is the most appropriate drug to relieve this abdominal distension?
A 66-year-old male presents to the outpatient cardiology clinic for evaluation of suspected primary hypertension. His blood pressure is elevated to 169/96 mm Hg, and his heart rate is 85/min. Physical examination reveals an overweight male with regular heart and lung sounds. Following repeated elevated blood pressure measurements, the diagnosis is made and the patient is started on hydrochlorothiazide. Of the following options, which is a side effect that one could experience from thiazide-like diuretics?
Which of the following is a carbonic anhydrase inhibitor?
Hydrochlorothiazide works by inhibiting
Which one of the following is not a clinical use of spironolactone?
Which of the following diuretics is contraindicated in Hepatic coma?
What is the effect of thiazide diuretics on urinary calcium excretion?
Side effects of oral carbonic anhydrase inhibitors include?
Loop and thiazide diuretics commonly cause clinically significant loss of:
Practice by Chapter
Carbonic Anhydrase Inhibitors
Practice Questions
Loop Diuretics
Practice Questions
Thiazide and Thiazide-Like Diuretics
Practice Questions
Potassium-Sparing Diuretics
Practice Questions
Carbonic Anhydrase Inhibitors
Practice Questions
Osmotic Diuretics
Practice Questions
Combination Diuretic Therapy
Practice Questions
Diuretics in Heart Failure
Practice Questions
Diuretics in Hypertension
Practice Questions
Diuretics in Renal Disorders
Practice Questions
Adverse Effects and Drug Interactions
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
