Clinical Pharmacology and Drug Toxicity — MCQs

On this page
A 35-year-old male presents to the emergency department with complaints of blurred vision, dizziness, and severe headache after ingesting an unknown quantity of homemade alcohol earlier in the day. On examination, he is disoriented. Laboratory tests reveal severe metabolic acidosis with a high anion gap. Which metabolite is primarily responsible for the toxicity in this case?
A 25-year-old woman presents to the emergency department 6 hours after ingesting a large quantity of paracetamol tablets. What is the most likely progression of paracetamol poisoning in this case?
A male patient complained of imbalance, numbness of the foot, and muscle weakness. On history taking, he revealed that he has been taking multivitamin tablets more than the prescribed dose for 1 year. Which of the following is the most likely cause of the associated symptoms seen in this patient?
A 50-year-old factory worker was brought to the emergency room with complaints of headache, vomiting, and blurring of vision after he consumed local spirit. Which of the following is used for the treatment of his condition?
A 55-year-old diabetic patient on metformin develops lactic acidosis after a contrast-enhanced CT scan. What is the mechanism by which metformin contributed to this complication?
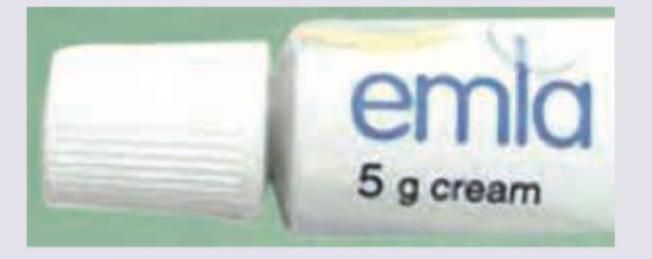
The application of the following product can lead to development of: (Recent NEET Pattern 2016-17)
Which of the following is a non-narcotic active principle of the opium poppy shown in the image below?

The toxin shown below will cause:

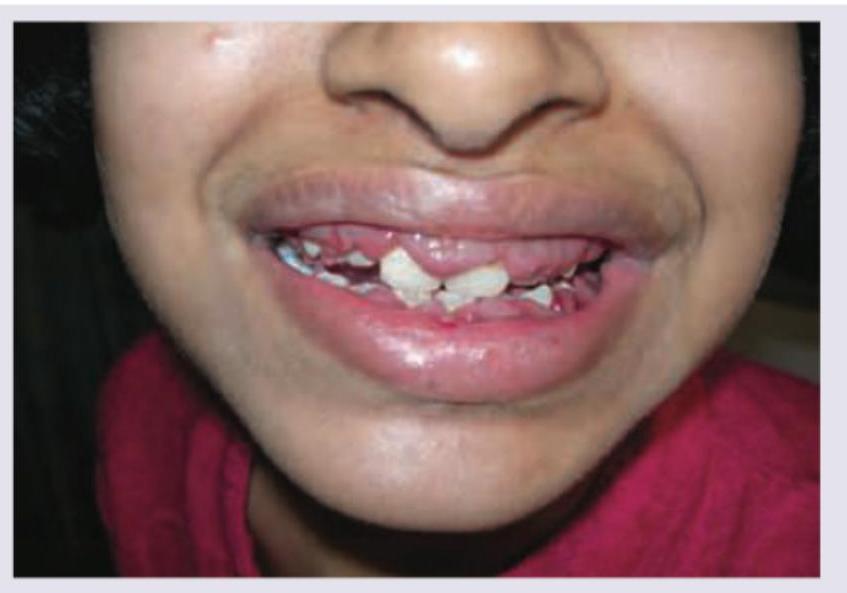
The condition shown in the image can be seen with all of the following EXCEPT:
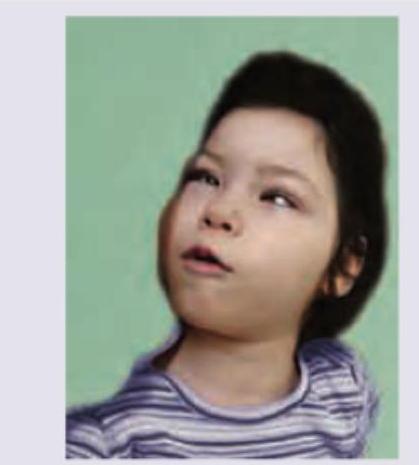
A 6-year-old child was having multiple vomiting episodes after eating at mid-day meal scheme in school. The Doctor at PHC gave injectable anti-emetics after which the child developed following posturing. What is the clinical diagnosis and what drug should be given to counteract this posturing?
Practice by Chapter
Principles of Clinical Pharmacology
Practice Questions
Therapeutic Drug Monitoring
Practice Questions
Drug Toxicity and Overdose
Practice Questions
Antidotes and Their Applications
Practice Questions
Management of Drug Poisoning
Practice Questions
Drug-Induced Liver Injury
Practice Questions
Drug-Induced Kidney Injury
Practice Questions
Drug-Induced Blood Dyscrasias
Practice Questions
Drug-Induced QT Prolongation
Practice Questions
Pharmacovigilance
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
