Clinical Pharmacology and Drug Toxicity — MCQs

On this page
Which of the following is NOT an immunosuppressant?
Which of the following is a category X drug?
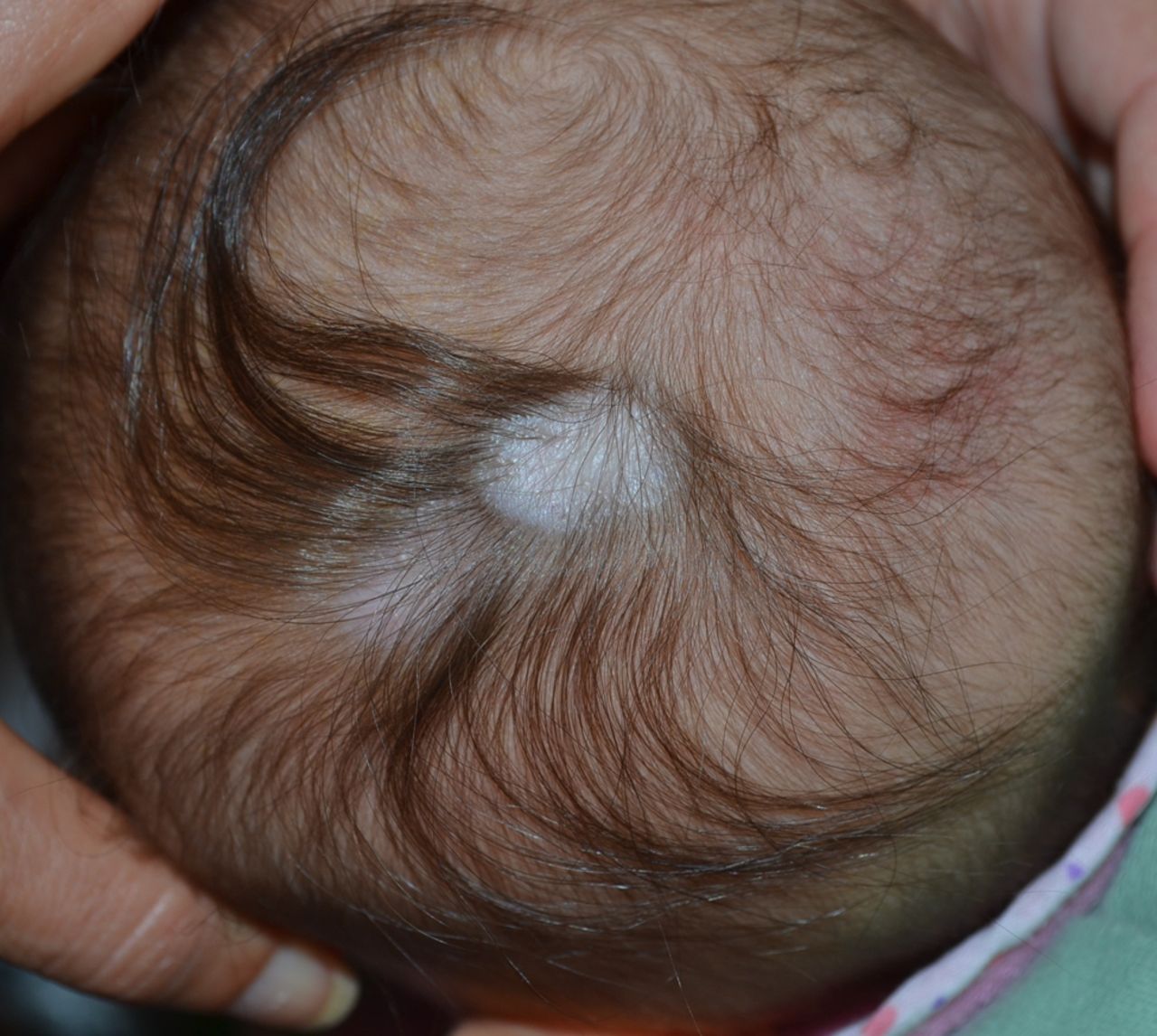
Which of the following drugs is responsible for the teratogenic effect shown in the image?
A 14-year-old boy presents with weakness, muscle twitching, drooling, and a generalized tonic-clonic seizure after helping his father in the yard. On arrival of emergency medical services, his heart rate is 40 beats per minute and his pupils are pinpoint. What is the most appropriate treatment for the likely toxic substance involved?
Which secretion is not decreased in organophosphate poisoning?
Which of the following immunosuppressant drugs is nephrotoxic?
Cyclosporine acts by decreasing the production of:
Naltrexone is used for which of the following poisonings?
What is the active metabolite of azathioprine?
Which of the following statements about fexofenadine is true?
Practice by Chapter
Principles of Clinical Pharmacology
Practice Questions
Therapeutic Drug Monitoring
Practice Questions
Drug Toxicity and Overdose
Practice Questions
Antidotes and Their Applications
Practice Questions
Management of Drug Poisoning
Practice Questions
Drug-Induced Liver Injury
Practice Questions
Drug-Induced Kidney Injury
Practice Questions
Drug-Induced Blood Dyscrasias
Practice Questions
Drug-Induced QT Prolongation
Practice Questions
Pharmacovigilance
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
