Clinical Pharmacology and Drug Toxicity — MCQs

On this page
Which one of the following medications is most likely to be responsible for this appearance?
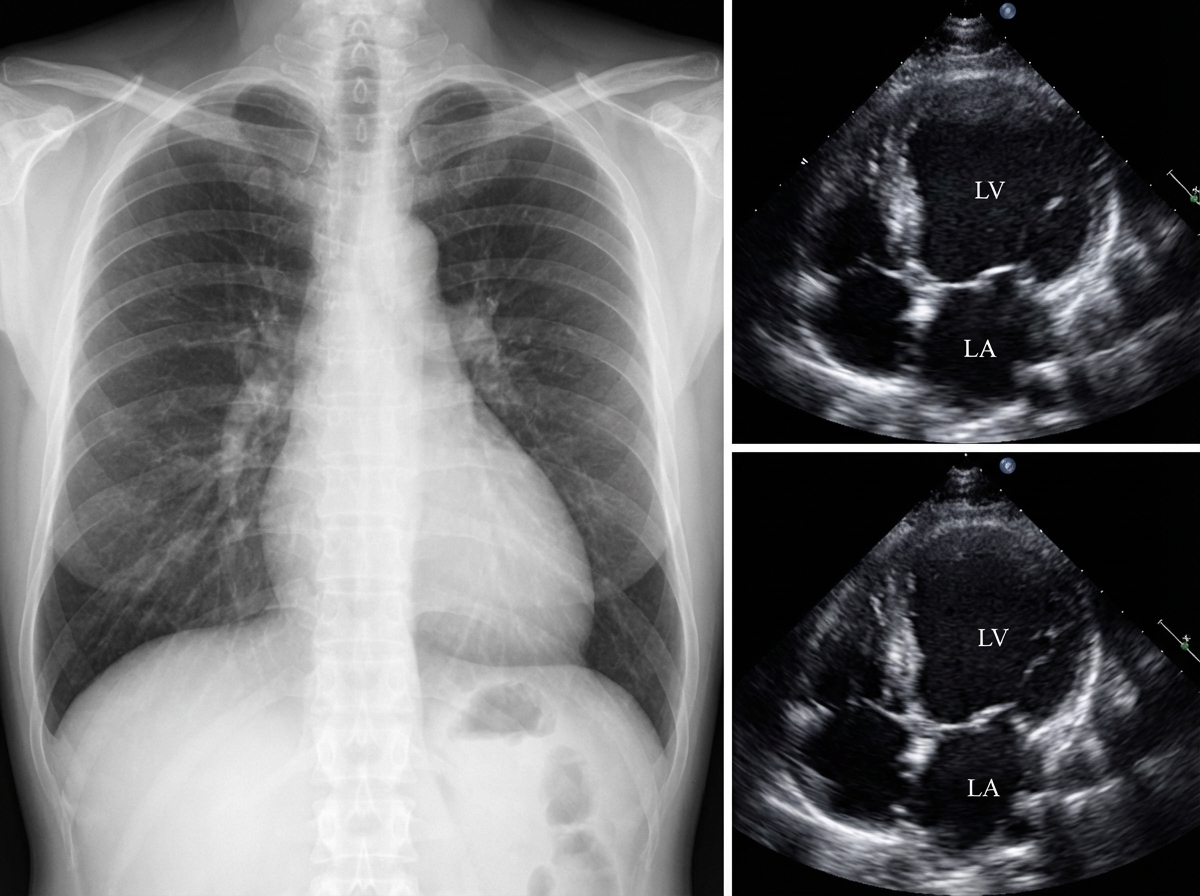
Forced alkaline diuresis is indicated in which of the following conditions?
Which of the following antimicrobials requires dose reduction even in mild renal failure?
Which of the following is an example of an idiosyncratic drug reaction?
All are adverse effects of cyclosporin, EXCEPT:
Cyclosporine acts on which of the following lymphocyte subsets?
Cyclosporine acts on which of the following lymphocyte subsets?
What is the recommended treatment for acute barbiturate poisoning?
Which drug can cause osteoporosis?
BAL is useful in treating poisoning due to all, except:
Practice by Chapter
Principles of Clinical Pharmacology
Practice Questions
Therapeutic Drug Monitoring
Practice Questions
Drug Toxicity and Overdose
Practice Questions
Antidotes and Their Applications
Practice Questions
Management of Drug Poisoning
Practice Questions
Drug-Induced Liver Injury
Practice Questions
Drug-Induced Kidney Injury
Practice Questions
Drug-Induced Blood Dyscrasias
Practice Questions
Drug-Induced QT Prolongation
Practice Questions
Pharmacovigilance
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
