Central Nervous System Pharmacology — MCQs

On this page
Which of the following drugs is NOT used in the condition shown?
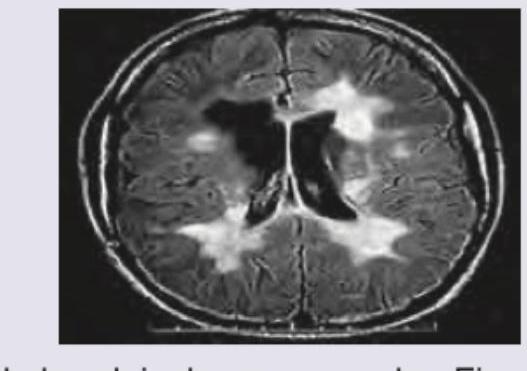
Which one of the following oral drugs may be used as adjunctive therapy in the management of super-refractory status epilepticus?
The anticonvulsant of choice in the treatment of generalized tonic-clonic seizures is
The first drug approved for Rett syndrome is?
Which of the following is the most effective oral drug for smoking cessation?
Which of the following is a new drug approved for Rett syndrome?
Which of the following is the most effective drug in smoking cessation?
Which of the following is true regarding nicotine substitution therapy?
All of the following are actions produced by mu receptors of morphine except:-
Shortest-acting muscle relaxant is:
Practice by Chapter
General Anesthetics
Practice Questions
Local Anesthetics
Practice Questions
Sedative-Hypnotics
Practice Questions
Antiepileptic Drugs
Practice Questions
Antiparkinsonian Drugs
Practice Questions
Opioid Analgesics
Practice Questions
Drugs of Abuse and Addiction
Practice Questions
Psychostimulants
Practice Questions
Hallucinogens
Practice Questions
CNS Stimulants and Cognitive Enhancers
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
