Central Nervous System Pharmacology — MCQs

On this page
On which receptor do barbiturates act?
Vigabatrin acts by:
Morphine can be used in all the following conditions except?
Which of the following is a potassium channel opener?
Which drug is not currently used in the management of Alzheimer's disease?
Which of the following is the least narcotic opioid?
Respiratory center depression can be caused by all of the following except?
Which drug, with chronic use in seizure states, has adverse effects including coarsening of facial features, hirsutism, gingival hyperplasia, and osteomalacia?
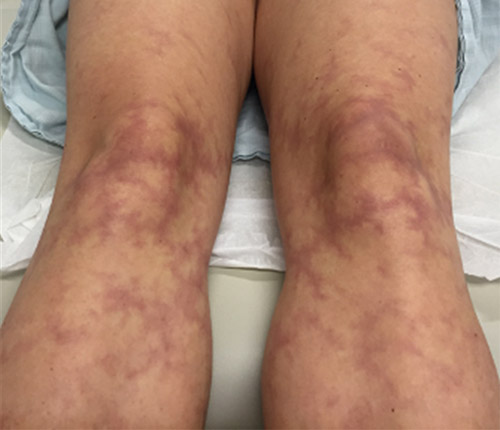
A patient with Parkinsonism being treated with one of the following drugs developed the skin condition shown in the image. Which drug is most likely responsible for this adverse effect?
Rivastigmine is used in the management of which condition?
Practice by Chapter
General Anesthetics
Practice Questions
Local Anesthetics
Practice Questions
Sedative-Hypnotics
Practice Questions
Antiepileptic Drugs
Practice Questions
Antiparkinsonian Drugs
Practice Questions
Opioid Analgesics
Practice Questions
Drugs of Abuse and Addiction
Practice Questions
Psychostimulants
Practice Questions
Hallucinogens
Practice Questions
CNS Stimulants and Cognitive Enhancers
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
