Cardiovascular Drugs — MCQs

On this page
Which drug possesses beta-adrenergic blocking, antioxidant, calcium channel blocking, and alpha-1 antagonist activities?
Which one of the following is the most characteristic arrhythmia associated with digitalis toxicity?
Vorapaxar acts by inhibiting which receptor?
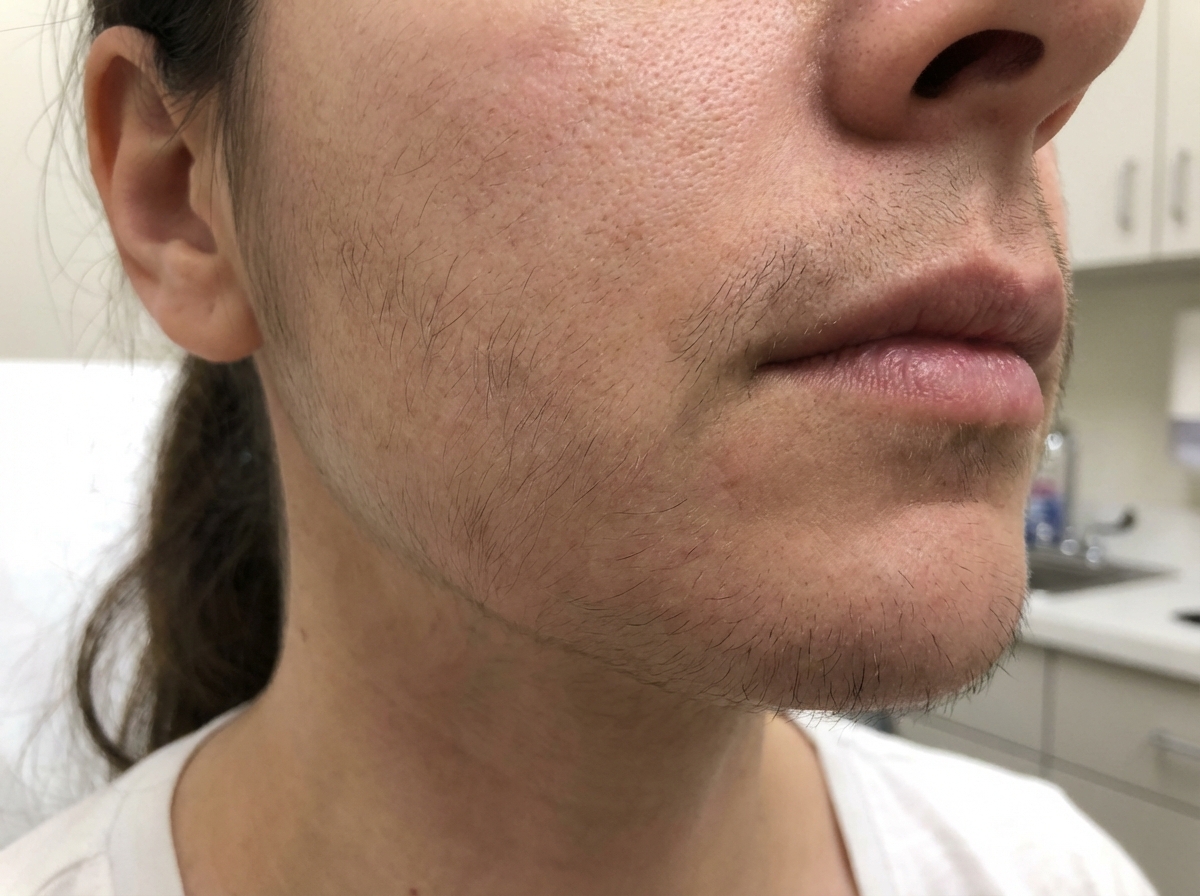
A 34-year-old lady on antihypertensives presented with certain features. Which of the following drugs is likely responsible for this condition?
In low doses, aspirin primarily acts on which enzyme?
What is the primary adverse effect of the combination use of beta-blockers and calcium channel blockers?
All of the following beta blockers have intrinsic sympathomimetic activity EXCEPT:
What is the mechanism of action of nifedipine?
Propranolol is contraindicated in diabetes mellitus due to which of the following reasons?
Which of the following drugs does NOT increase nitric oxide levels?
Practice by Chapter
Antihypertensive Agents
Practice Questions
Drugs for Heart Failure
Practice Questions
Antiarrhythmic Drugs
Practice Questions
Antianginal Agents
Practice Questions
Lipid-Lowering Drugs
Practice Questions
Anticoagulants and Antiplatelet Drugs
Practice Questions
Thrombolytic Agents
Practice Questions
Drugs Used in Pulmonary Hypertension
Practice Questions
Drugs Used in Shock
Practice Questions
Cardiovascular Effects of Non-Cardiovascular Drugs
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
