Cardiovascular Drugs — MCQs

On this page
All the following agents may be used for the management of hypertensive crisis EXCEPT?
All are true about ranolazine except?
The side effect of corneal microdeposits is seen most commonly with which of the following drugs?
Ticagrelor is used for what purpose?
What is the dose of Reteplase for the management of acute myocardial infarction?
What is the drug of choice for pregnancy-induced hypertension?
Which drug prescribed by the physician would most probably be responsible for this condition?
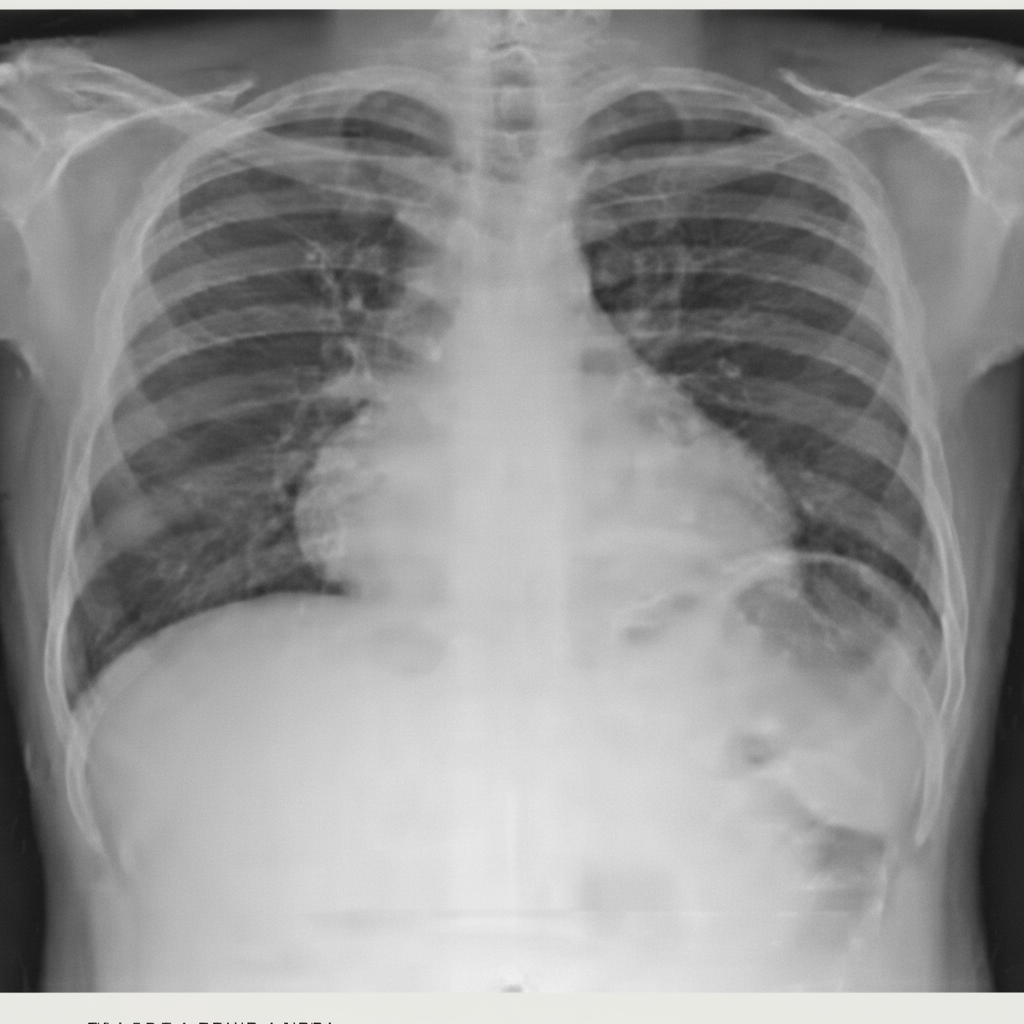
Which of the following agents is a thrombin receptor antagonist?
Enhancement of the effects of bradykinin is most likely to occur with which of the following drugs?
What is the most significant adverse effect of ACE inhibition?
Practice by Chapter
Antihypertensive Agents
Practice Questions
Drugs for Heart Failure
Practice Questions
Antiarrhythmic Drugs
Practice Questions
Antianginal Agents
Practice Questions
Lipid-Lowering Drugs
Practice Questions
Anticoagulants and Antiplatelet Drugs
Practice Questions
Thrombolytic Agents
Practice Questions
Drugs Used in Pulmonary Hypertension
Practice Questions
Drugs Used in Shock
Practice Questions
Cardiovascular Effects of Non-Cardiovascular Drugs
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
