Cardiovascular Drugs — MCQs

On this page
Morphine is used in:
Which antiplatelet drug acts via purinergic receptors and is not largely impacted by CYP2C19 polymorphism?
Methyl dopa acts on which of the following receptors?
What is the best drug for the rhythm disorder shown below?
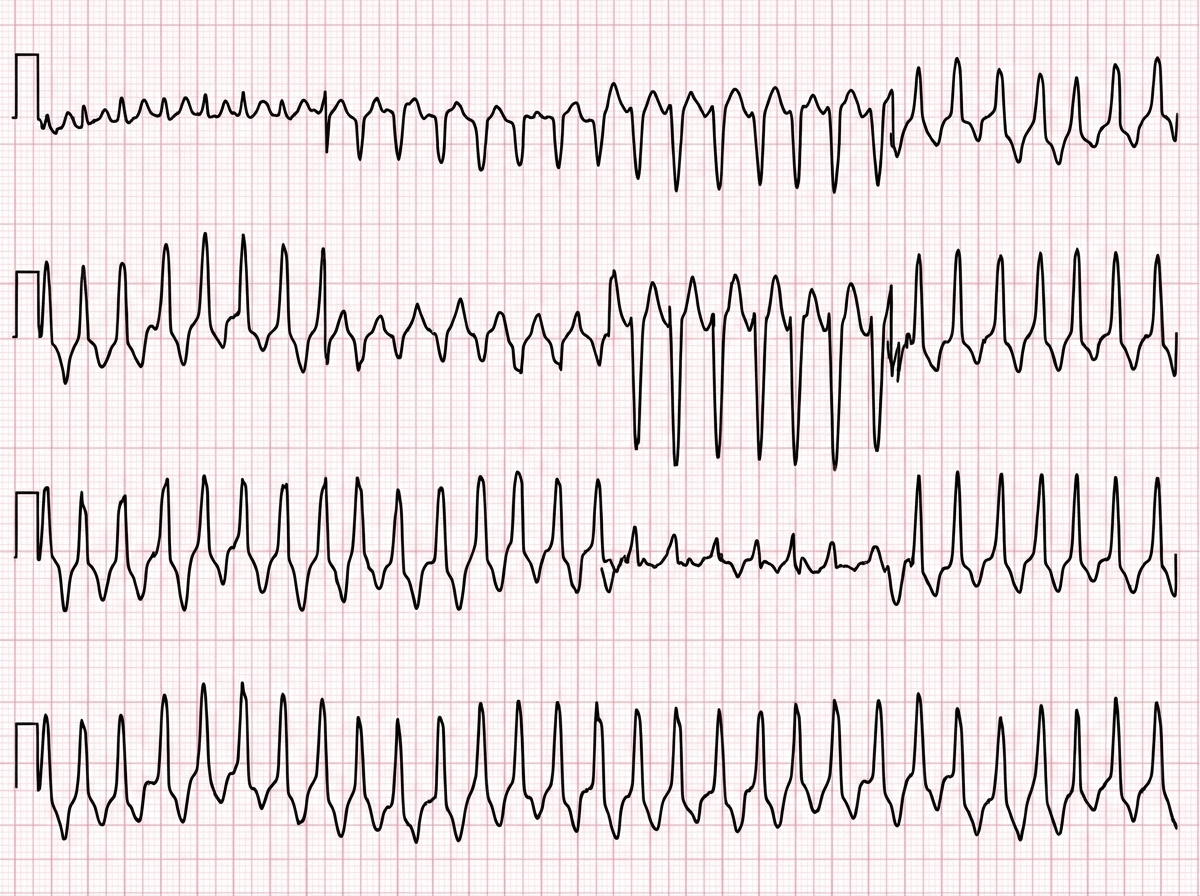
Which of the following drugs should be avoided in a pregnant female with dilated cardiomyopathy?
Clevidipine is a type of which drug class?
Which drug is used to treat ventricular arrhythmias caused by digoxin toxicity?
All of the following drugs can worsen angina, except:
Septicemic shock with multi-organ failure is treated by which of the following medications?
Quinidine exerts its action on the heart by which mechanism?
Practice by Chapter
Antihypertensive Agents
Practice Questions
Drugs for Heart Failure
Practice Questions
Antiarrhythmic Drugs
Practice Questions
Antianginal Agents
Practice Questions
Lipid-Lowering Drugs
Practice Questions
Anticoagulants and Antiplatelet Drugs
Practice Questions
Thrombolytic Agents
Practice Questions
Drugs Used in Pulmonary Hypertension
Practice Questions
Drugs Used in Shock
Practice Questions
Cardiovascular Effects of Non-Cardiovascular Drugs
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
