Antimicrobial Agents — MCQs

On this page
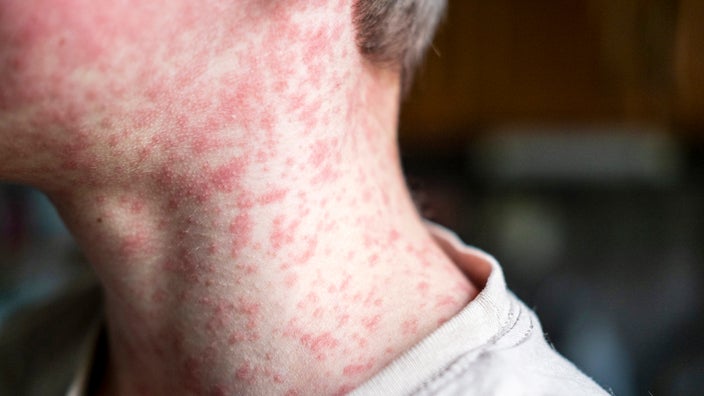
The condition shown in the image is due to excessive/rapid usage of?
Tafenoquine, approved in July 2018, is used for which of the following?
Which among the following fluoroquinolones has the longest half-life?
Which of the following classes of drugs is lumefantrine best associated with?
What is the recommended daily dose of amphotericin B for a patient with suspected severe fungal infection?
What is the drug of choice for the treatment of pertussis?
Which of the following antifungal drugs has a broad antifungal spectrum?
Which of the following is recommended as a dual-active drug targeting both HBV and HIV?
Prolonged treatment with isoniazid (INH) leads to deficiency of:
Which of the following anti-influenza drugs can cause Livedo reticularis?
Practice by Chapter
Beta-Lactam Antibiotics
Practice Questions
Aminoglycosides
Practice Questions
Macrolides and Ketolides
Practice Questions
Tetracyclines
Practice Questions
Quinolones
Practice Questions
Sulfonamides and Trimethoprim
Practice Questions
Antimycobacterial Drugs
Practice Questions
Antifungal Agents
Practice Questions
Antiviral Drugs
Practice Questions
Antiparasitic Agents
Practice Questions
Principles of Antimicrobial Selection
Practice Questions
Antimicrobial Resistance
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
