Antimicrobial Agents — MCQs

On this page
Single-dose mebendazole is effective in the treatment of which of the following helminthic infections?
Which of the following statements about Bedaquiline is TRUE?
Which antibacterial agent can be used intranasally for prophylaxis against recurrent Staphylococcus aureus infection?
All of the following are true regarding cephalosporins, except:
Which of the following is NOT a protease inhibitor?
Which one of the following is best associated with Lumefantrine?
What is the drug of choice for Chagas disease?
Which of the following antibiotics, known for its narrow spectrum of activity and use in managing abdominal abscesses caused by Bacteroides fragilis, can also lead to antibiotic-associated colitis?
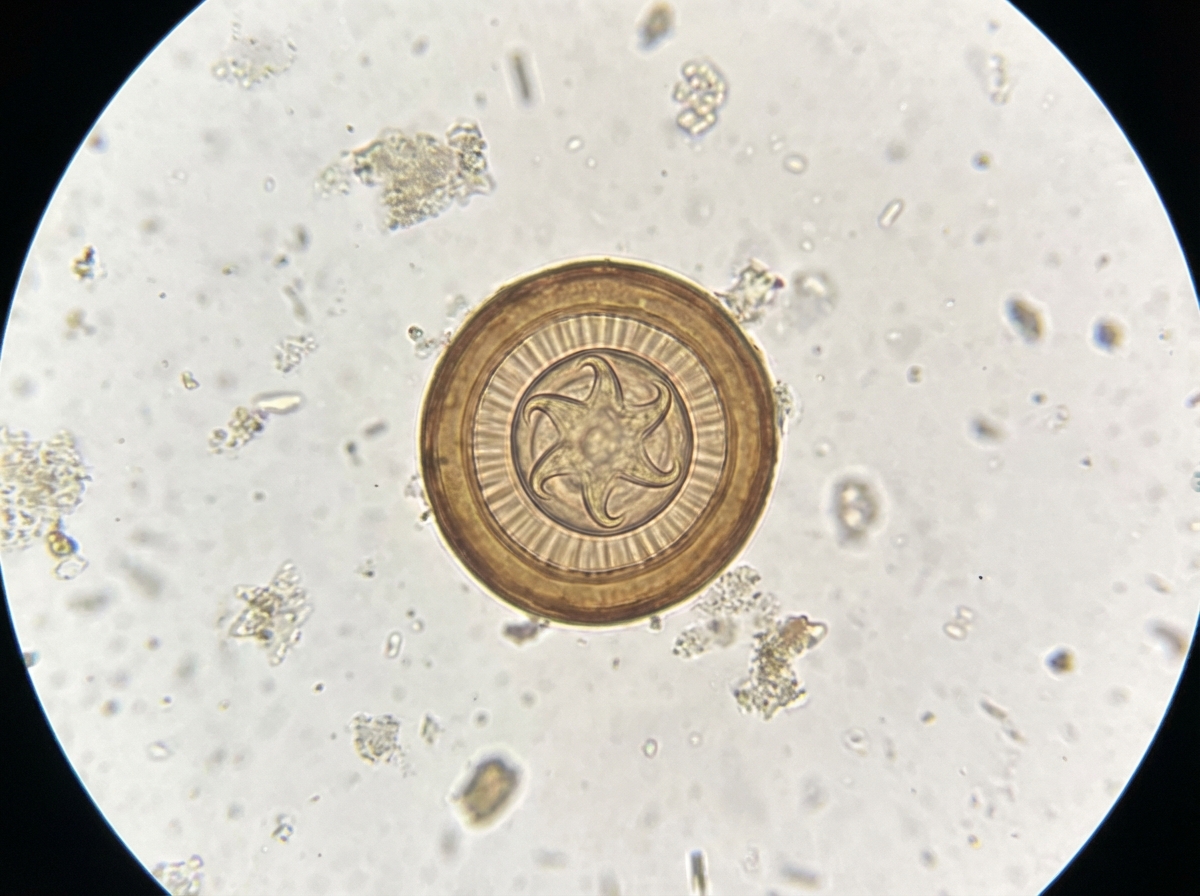
A 10-year-old child presents with diarrhea and abdominal pain for 4 days. Stool microscopy reveals findings suggestive of a parasitic infection. Which of the following medications is indicated for treatment?
Which of the following inhibitors of protein synthesis is primarily bactericidal?
Practice by Chapter
Beta-Lactam Antibiotics
Practice Questions
Aminoglycosides
Practice Questions
Macrolides and Ketolides
Practice Questions
Tetracyclines
Practice Questions
Quinolones
Practice Questions
Sulfonamides and Trimethoprim
Practice Questions
Antimycobacterial Drugs
Practice Questions
Antifungal Agents
Practice Questions
Antiviral Drugs
Practice Questions
Antiparasitic Agents
Practice Questions
Principles of Antimicrobial Selection
Practice Questions
Antimicrobial Resistance
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
