Analgesics and Anti-inflammatory Drugs — MCQs

On this page
A female patient complains of swelling and pain in her great toe. Her uric acid level is found to be high. A drug that reduces uric acid levels is prescribed. Which of the following enzymes should the drug inhibit?
A 60 -year-old patient of carcinoma prostate is having skeletal metastasis. He was put on 8 mg of hydromorphone daily but is still having severe bone pain. He was then put on the transdermal system shown below. All are correct about this transdermal system except:
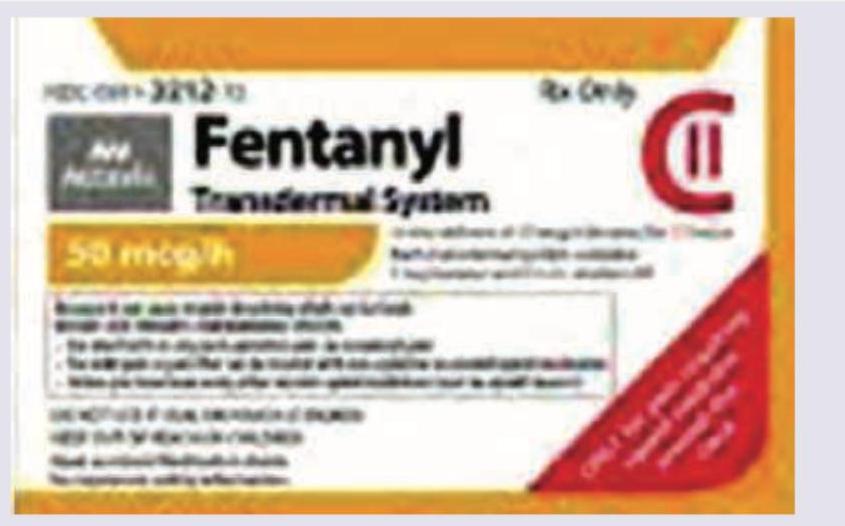
Treatment of first choice in acute Gout is
A patient presents with swelling in MCP joints, and his serum uric acid levels were found to be elevated. His physician prescribed a drug which is considered as the first line agent in the management of this condition. What is the mechanism of this drug?
What is the mechanism of action of cyclosporine?
What is the mechanism of action of local anesthetics?
An otherwise healthy 15-month-old boy is brought to the emergency department by his mother 1 hour after having a single episode of generalized tonic-clonic seizure, which stopped spontaneously after 1 minute. He was sleepy initially but is now awake and alert. His mother reports that he has had a fever and runny nose for the past 3 days. His temperature is 40.1°C (104.2°F). Physical examination shows no abnormalities. Analysis of his cerebrospinal fluid shows 3 cells/mm3, a glucose concentration of 68 mg/dL, and a protein concentration of 35 mg/dL. Administration of a drug that acts through which of the following mechanisms of action is most appropriate in this patient?
Shortest acting local anaesthetic
Drug used in osteoarthritis
NSAID used commonly for topical ocular use is
Practice by Chapter
NSAIDs: Classification and Mechanism
Practice Questions
COX-2 Selective Inhibitors
Practice Questions
Acetaminophen (Paracetamol)
Practice Questions
Opioid Analgesics and Antagonists
Practice Questions
Drugs Used in Gout and Hyperuricemia
Practice Questions
Drugs Used in Rheumatoid Arthritis
Practice Questions
Disease-Modifying Antirheumatic Drugs
Practice Questions
Glucocorticoids as Anti-inflammatory Agents
Practice Questions
Migraine Therapeutics
Practice Questions
Neuropathic Pain Management
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
