Upper Respiratory Tract Infections — MCQs

4 year old male, recurrent URTI, has difficulty breathing, High arched palate, Failure to grow and impaired hearing, management is
A child presents with recurrent ear infections and conductive hearing loss. What is the most likely diagnosis?
A 4-year-old boy presents with low-grade fever, inspiratory stridor, and barking cough for the past 5 days. Examination reveals a hoarse voice, a moderately inflamed pharynx, and a slightly increased respiratory rate. His chest x-ray showed subglottic narrowing appearing like a steeple. Which among the following is not indicated in the treatment of this condition?
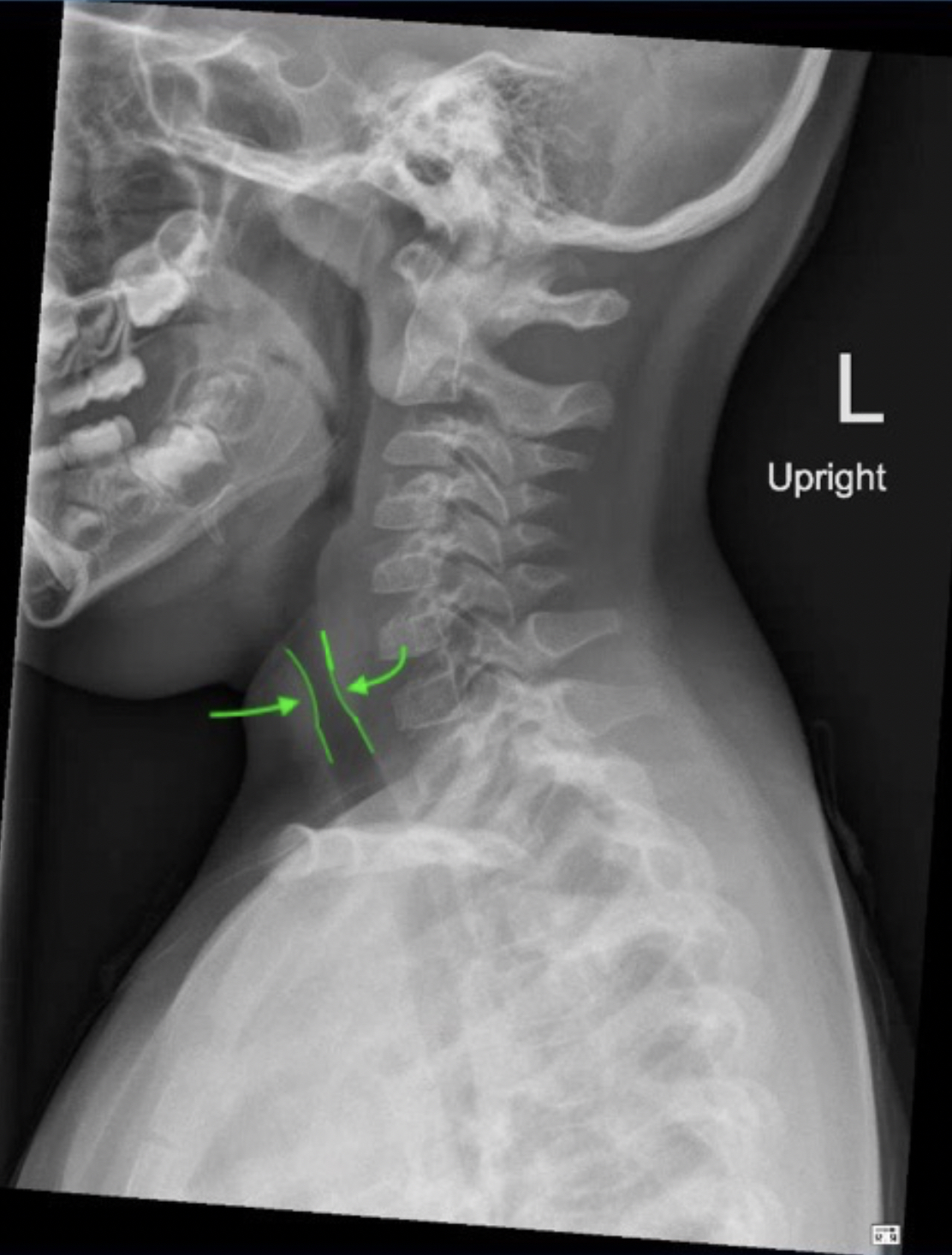
A patient presents with hoarseness of voice and a clinical condition as shown in the image. Identify the lesion:
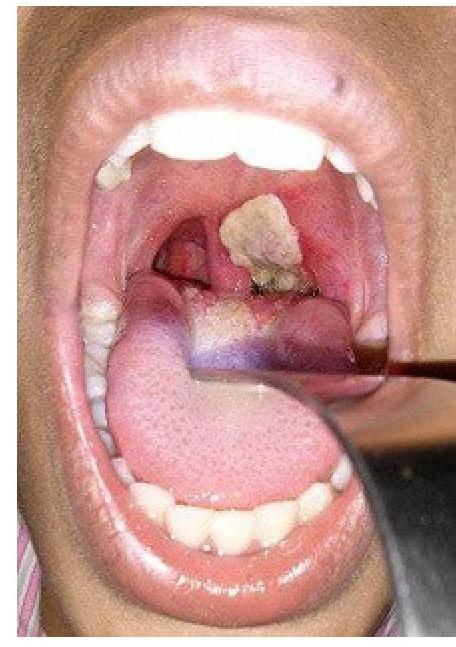
Most dangerous sign in lower respiratory tract infection (LRTI) in children is:
Which of the following is not associated with primary ciliary dyskinesia?
A 2-month-old child with a birth weight of 2 kg presents with poor feeding, excessive sleepiness, and wheezing. What is the most likely diagnosis?
Which of the following conditions is most associated with digital clubbing in children?
A 24 month child, with a weight of 11 kg, has RR of 38 / min, chest indrawing, cough and fever. Management according to IMNCI?
A 10-year-old male child presenting with complaints of poor growth, poor appetite, short stature, clubbing, and recurrent chest infections, along with steatorrhea, is most likely diagnosed with what?
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
