Respiratory Diseases — MCQs

On this page
An 11-month-old child presents with complaints of respiratory distress. On examination, there are bilateral crepitations and wheezing. Which of the following is the most likely cause?
A 2-year-old female child presented to a Primary Health Centre with a 4-day history of cough and fever, and inability to drink for the last 12 hours. On examination, the child weighed 5 kg and had a respiratory rate of 45/minute with fever. According to the WHO Integrated Management of Childhood Illness (IMCHI) classification, how would this child be classified?
Which of the following is a sign of severe pneumonia in an 18-month-old child?
What is the earliest presenting feature of cystic fibrosis in a neonate?
In cystic fibrosis, which organism most commonly causes infection?
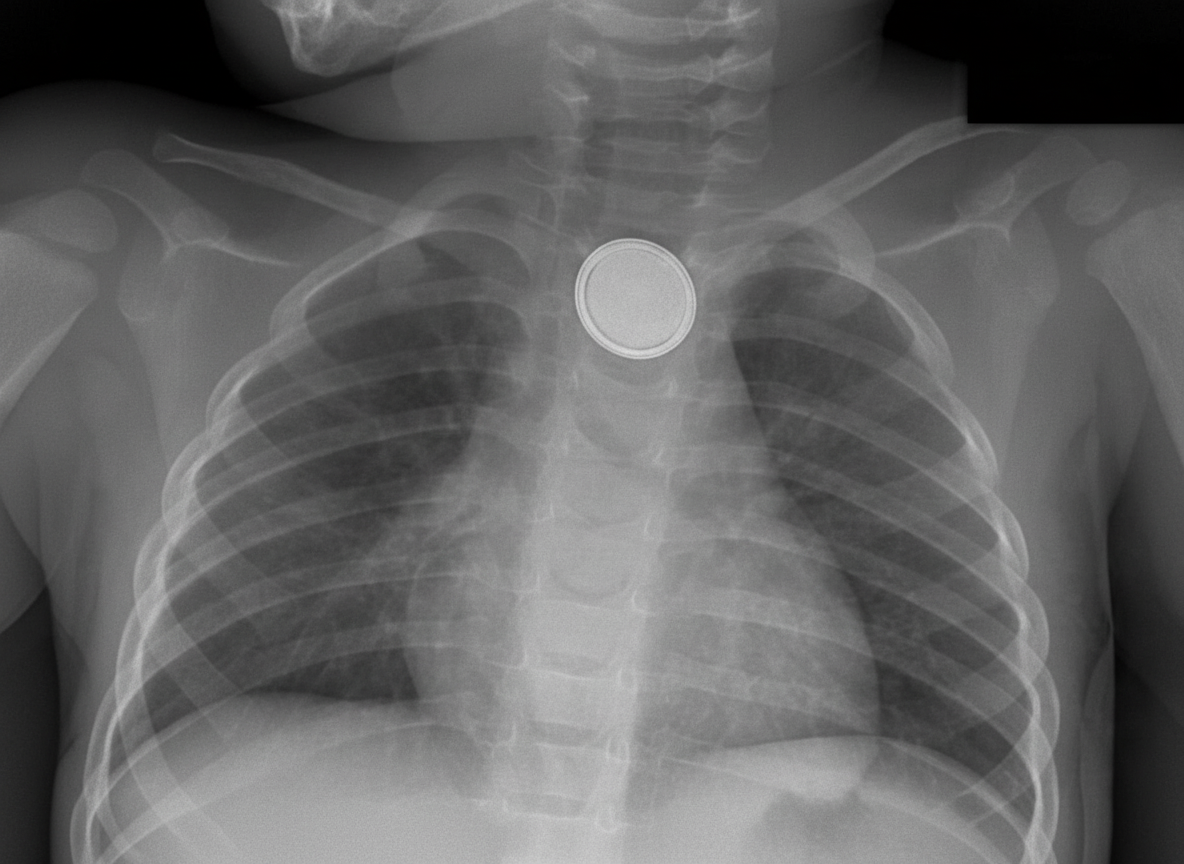
A 4-year-old child presents with findings on a chest X-ray. What is the probable location of the foreign body visible on the skiagram?
What is the cutoff value of sweat chloride above which consistently higher readings are diagnostic for Cystic fibrosis?
A child presents with fever and a barky cough. On examination, the respiratory rate is 36/min, stridor is present only on crying, and the temperature is 39 degrees Celsius. There are no other abnormal findings. What is the next logical step in management?
Croup syndrome is usually caused by which of the following viruses?
Pneumatocele is most commonly caused by which organism?
Practice by Chapter
Upper Respiratory Tract Infections
Practice Questions
Lower Respiratory Tract Infections
Practice Questions
Asthma Management
Practice Questions
Cystic Fibrosis
Practice Questions
Bronchiolitis
Practice Questions
Foreign Body Aspiration
Practice Questions
Sleep-Disordered Breathing
Practice Questions
Congenital Lung Malformations
Practice Questions
Pleural Diseases
Practice Questions
Tuberculosis in Children
Practice Questions
Chronic Lung Disease in Premature Infants
Practice Questions
Pulmonary Function Testing
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
