Respiratory Diseases — MCQs

On this page
Loeffler's syndrome is characterized by:
What are the WHO criteria for hospital admission in pneumonia?
All of the following are used in the acute attack of asthma in a 4-year-old child, except:
A 4-month-old infant presents with cough and a respiratory rate greater than 60/min, with no chest retractions. What is the appropriate management according to the Integrated Management of Childhood Illness (IMNCI) protocol?
A 3-year-old, well-immunized male child presents with sore throat, fever, noisy breathing, and inability to swallow for the past four hours. Examination reveals a toxic, tachypneic child with inspiratory stridor, suprasternal, supraclavicular, and intercostal retractions during inspiration. What is the most likely diagnosis?
A 14-year-old boy presented with chronic diarrhea and weight loss. History reveals that he has repeated attacks of respiratory tract infections with Pseudomonas aeruginosa. His younger brother died from a severe respiratory infection at the age of 7. Which of the following agents is most likely to improve this patient's condition?
Bronchiolitis obliterans is suggested by all findings except:
What is the MOST suitable management for a 2-year-old child presenting with cough for 5 days? On examination, the respiratory rate is 40/minute. The child is well-nourished, active, and feeding well.
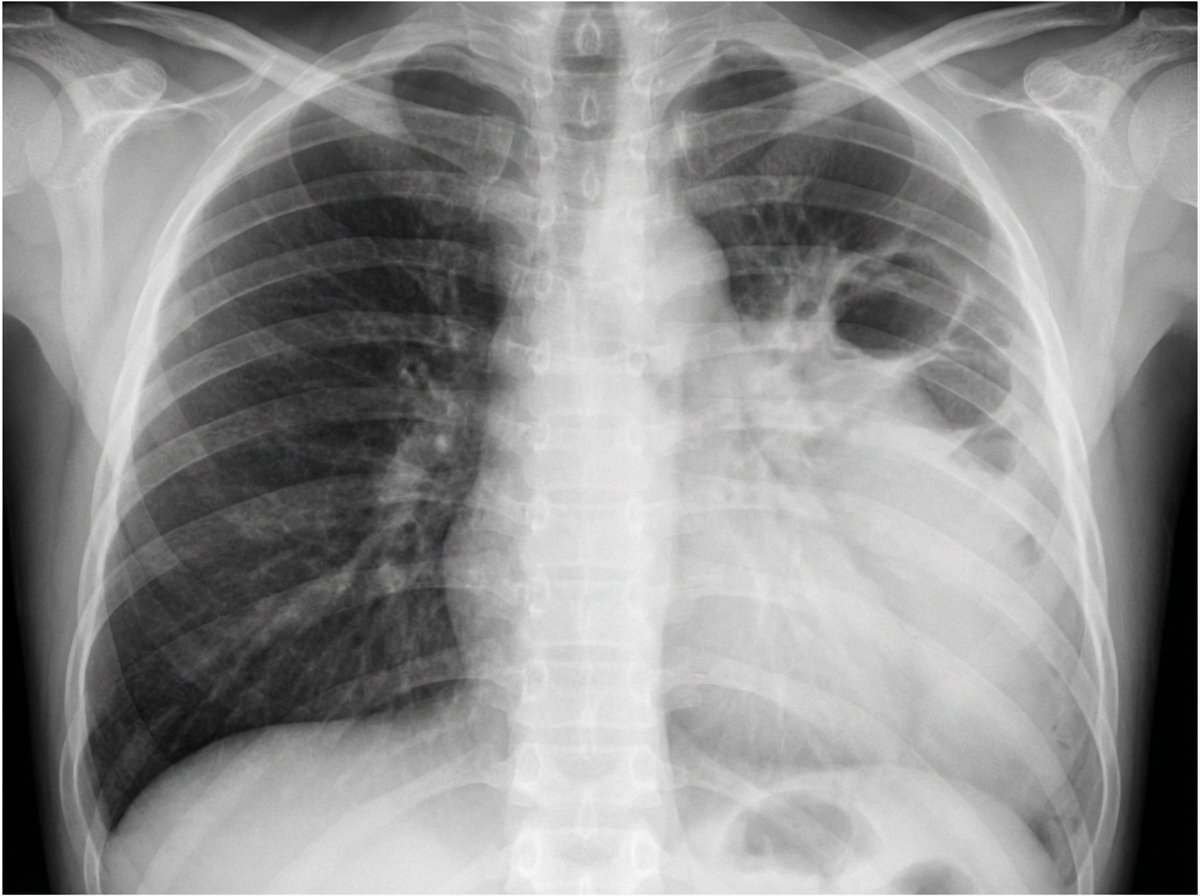
What is the most likely etiology in a 10-month-old child with a 7-day history of high-grade fever, exhibiting the following X-ray findings, and not responding to ceftriaxone?
Palivizumab, a monoclonal antibody, is used for the prophylaxis of:
Practice by Chapter
Upper Respiratory Tract Infections
Practice Questions
Lower Respiratory Tract Infections
Practice Questions
Asthma Management
Practice Questions
Cystic Fibrosis
Practice Questions
Bronchiolitis
Practice Questions
Foreign Body Aspiration
Practice Questions
Sleep-Disordered Breathing
Practice Questions
Congenital Lung Malformations
Practice Questions
Pleural Diseases
Practice Questions
Tuberculosis in Children
Practice Questions
Chronic Lung Disease in Premature Infants
Practice Questions
Pulmonary Function Testing
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
