Respiratory Diseases — MCQs

On this page
An infant presents with fever and persistent cough. Physical examination and a chest X-ray suggest pneumonia. Which of the following is the most likely cause of this infection?
A 3-year-old child with cystic fibrosis presents with weight loss, irritability, and a chronic productive cough. On physical exam, he is febrile and lung exam reveals intercostal retractions, wheezing, rhonchi, and rales. Chest x-ray demonstrates patchy infiltrates and atelectasis. Gram's stain of the sputum reveals slightly curved, motile gram-negative rods that grow aerobically. Which of the following diseases is most commonly caused by the microorganism responsible for this child's pneumonia?
A child experiences nocturnal asthma attacks twice a week and daytime attacks three or more times per week. According to asthma severity classification guidelines, how would this condition be categorized?
A 3-year-old boy presented with recurrent attacks of pneumonia and otitis media since his first birthday. Diagnosis is X-linked agammaglobulinemia. What is the most likely offending organism?
A 13-year-old known asthmatic presents with severe wheezing and a respiratory rate of 40. Her pulse rate is 120. What is the next best step in management of this patient?
What is the most common etiological agent for acute bronchiolitis in infancy?
Which of the following conditions is characterized by hyperinflation of the lungs on a chest X-ray?
What is the most common mode of treatment for a 1-year-old child with asthma?
A previously healthy 2-year-old black child has developed a chronic cough during the previous 6 weeks. He has been seen in different emergency rooms on two occasions during this period and has been placed on antibiotics for pneumonia. Upon auscultation, you hear normal breath sounds on the left. On the right side, you hear decreased air movement during inspiration but no air movement upon expiration. Inspiratory and expiratory radiographs of the chest are shown. Which of the following is the most appropriate next step in making the diagnosis in this patient?
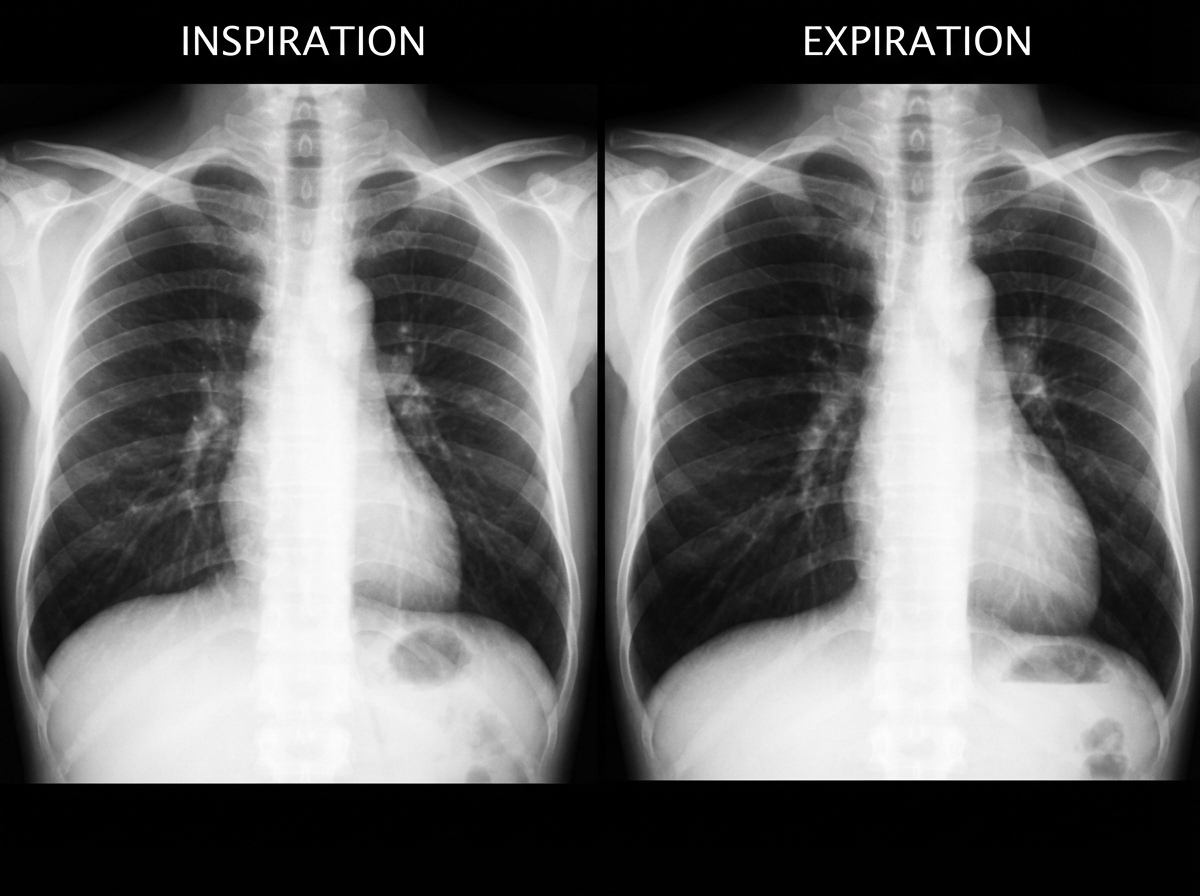
A 7.5-month-old child presents with cough and mild stridor, initially treated with oral antibiotics showing improvement. Subsequently, the child developed wheeze, productive cough, and mild fever. Radiography reveals hyperlucency, and pulmonary function tests demonstrate an obstructive pattern. What is the most probable diagnosis?
Practice by Chapter
Upper Respiratory Tract Infections
Practice Questions
Lower Respiratory Tract Infections
Practice Questions
Asthma Management
Practice Questions
Cystic Fibrosis
Practice Questions
Bronchiolitis
Practice Questions
Foreign Body Aspiration
Practice Questions
Sleep-Disordered Breathing
Practice Questions
Congenital Lung Malformations
Practice Questions
Pleural Diseases
Practice Questions
Tuberculosis in Children
Practice Questions
Chronic Lung Disease in Premature Infants
Practice Questions
Pulmonary Function Testing
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
